An Introduction to Silver Diamine Fluoride
Silver diamine fluoride, or SDF, has become a hot topic in preventative and caries-management dentistry in the last decade. As a newer product, many questions about its history and usage as a preventative and caries-management tool have yet to be answered. This article addresses the history of using silver-based products for caries management and how silver diamine fluoride is utilized to prevent caries and arrest the progression of active carious lesions.
History of Caries Prevention
Dental caries has been a human problem for millennia. The first known use of mitigating dental decay through caries prevention can be seen centuries ago in Asia, where the concept of “tooth darkening” was introduced.
This treatment utilized different solutions to stain and darken the teeth to a jet-black appearance. In Japan, the “ohaguro” concept of staining teeth was seen as a form of beauty. A secondary effect of this staining was that the teeth became resistant to dental decay.
Years later, medicaments explicitly designed to prevent tooth decay were applied to teeth by dental professionals. In the Americas, silver nitrate was utilized in the early 1900s to help conservatively arrest and manage dental caries.
Solutions such as silver nitrate were used to arrest carious lesions in patients with substantial dental decay. However, with the advent of local anesthetics and new materials for dental restorations, most of these conservative caries management treatment options decreased in popularity.
In 2014, the FDA approved SDF for use as a desensitizing agent in the United States. Although SDF has been approved for use as a desensitizing agent, it has been effectively used off-label for its caries prevention and caries-arresting properties.
Most products today comprise 38% SDF in solution. Silver diamine fluoride is a liquid solution with a pH of approximately 10 composed of silver, fluoride, and ammonia particles. It can be applied to both primary and permanent teeth to aid in caries prevention and management.
SDF for Caries Prevention
SDF is a valuable tool in the prevention of dental caries. Laboratory studies performed on extracted teeth have found that biofilms could not form on teeth treated with SDF. Additionally, SDF kills the bacteria that lead to dental caries.
One unique advantage of SDF is its widespread preventative effect in the oral cavity. Even when SDF is applied to only a single tooth, the preventative effect is experienced on the adjacent teeth. This antimicrobial effect is profound, leading to a “zombie effect” in which bacteria killed after being exposed to SDF can contribute to killing other active cariogenic bacteria in the mouth.
SDF is especially advantageous for caries prevention in populations more susceptible to developing decay. Studies have shown that one annual application of SDF has a greater preventative effect than repeated applications of other preventative medicaments, such as topical fluoride.
SDF for Arresting Caries
Recently, SDF has gained popularity as a conservative method for arresting active carious lesions. Current research on SDF has shown it is extremely effective at this. In a study investigating the effectiveness of arresting root caries in elderly patients, 90% of carious lesions were arrested after a single application of SDF.
SDF can be a useful tool for conservative management of dental caries in specific clinical scenarios. Patients who have limited access to dental care, have medical or behavioral concerns that make traditional operative dentistry an extreme challenge, and have rampant dental caries can benefit from the utilization of silver diamine fluoride.
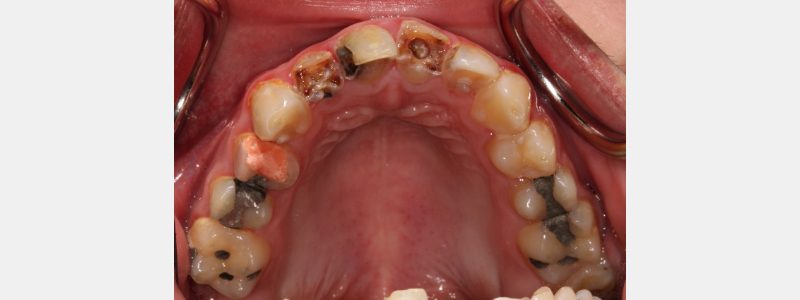
After SDF has been applied, the solution starts to kill the bacteria that have caused the carious lesion. Over a few weeks, the initial lesion will harden due to remineralization of the tooth structure.
As this occurs, the carious lesion will become darker and jet-black. The dentin in this dark, arrested carious lesion is more resistant to attack from carious bacteria than sound, unaffected dentin.
Since this dark lesion may present as an esthetic dilemma, it is advised to inform patients of the staining that SDF can cause and to have an informed consent form reviewed by the patient or their guardian prior to application of SDF.
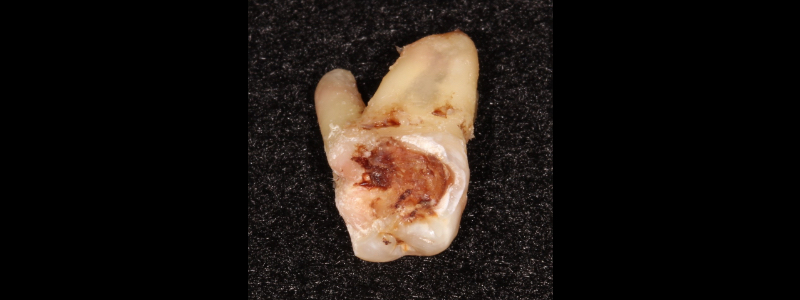
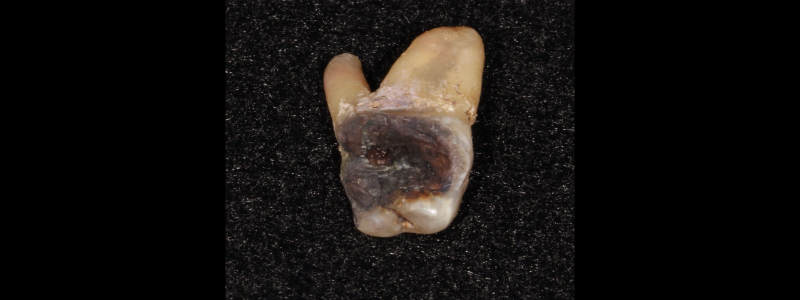
Teeth treated with SDF can still be restored. Both total-etch and self-etch methods have proven effective in bonding composite to non-carious dentin treated with SDF. Glass ionomers can also be effectively placed on teeth treated with SDF.
Disadvantages and Side Effects
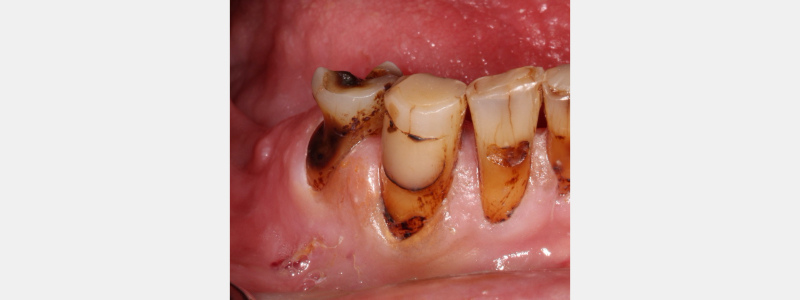
The main disadvantage of SDF is its tendency to stain active carious lesions. Healthy, unaffected enamel and dentin are resistant to staining from SDF. However dentin with carious bacteria will stain jet-black after being exposed to SDF.
A saturated potassium iodide solution can be applied to reduce this dark staining. This solution will bind to excess silver particles and reduce the level of staining. However, initial research has shown that minimal staining reduction occurs after applying potassium iodide.
SDF staining will also occur on gloves, tabletops, clothing, or any other surface that SDF comes into contact with. Care must be taken to protect surfaces and the patient’s clothing to avoid accidentally staining these areas.
Since SDF contains silver particles, some patients report a metallic taste during the application. This is typically transient and will dissipate shortly after the treatment is completed.
SDF should not be applied if a patient is known to have an allergy to silver. SDF can also irritate the gingiva, so it is contraindicated in patients with mucositis or desquamating gingivitis.
Application Protocol
The maximum dosage of SDF is one drop of liquid for every 10 kg of the patient’s weight, and it should never be exceeded. One drop of SDF can effectively be applied to up to five teeth.
Various protocols for application of SDF exist. The protocol below is based off some of the most current strategies for caries management using SDF:
- Isolate the area using cotton rolls and/or gauze.
- If near the gingiva, consider applying a layer of petroleum jelly to protect the gingiva from irritation.
- Dry the area that SDF will be applied.
- Using a microbrush, apply SDF to the affected area. Allow the solution to remain on the tooth for one minute.
- Remove excess SDF solution with a cotton roll.
- Rinse area with water.
Repeating applications multiple times per year is advised to maximize the prevention and caries arresting effects of SDF.
Conclusions
SDF is a newer product that can help aid in the caries management process. It is beneficial for patients at a high caries risk and for patients with limitations that prevent them from performing adequate oral hygiene, home care, or undergoing traditional restorative dentistry procedures.
While it is not a panacea for preventing and managing dental caries, SDF is a useful tool that when applied in the proper clinical situations can help our patients with the prevention and management of their dental decay.
References
- Quock, R. L., Barros, J. A., Yang, S. W., & Patel, S. A. (2012). Effect of silver diamine fluoride on microtensile bond strength to dentin. Operative Dentistry, 37(6), 610-616.
- Horst, J. A., Ellenikiotis, H., & Milgrom, P. L. (2016). UCSF protocol for caries arrest using silver diamine fluoride: rationale, indications and consent. Journal of the California Dental Association, 44(1), 17-28.
- Knight, G. M., McIntyre, J. M., Craig, G. G., Zilm, P. S., & Gully, N. J. (2009). Inability to form a biofilm of Streptococcus mutans on silver fluoride-and potassium iodide-treated demineralized dentin. Quintessence International, 40(2).
- Mei, M. L., Lo, E. C., & Chu, C. H. (2016). Clinical use of silver diamine fluoride in dental treatment. Compendium of Continuing Education in Dentistry, 37(2), 93-98.
- Horst, J. A., & Heima, M. (2019). Prevention of dental caries by silver diamine fluoride. Compendium of Continuing Education in Dentistry, 40(3), 158-163.
- Li, R., Lo, E. C. M., Liu, B. Y., Wong, M. C. M., & Chu, C. H. (2016). Randomized clinical trial on arresting dental root caries through silver diammine fluoride applications in community-dwelling elders. Journal of Dentistry, 51, 15-20.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Andy Janiga
Date: March 31, 2021
Featured Digest articles
Insights and advice from Spear Faculty and industry experts