How to Phase Treatment
In a previous article, I wrote about the advantage of phasing the treatment of larger cases. Phasing treatment takes a large case (e.g., full mouth) but breaks it into smaller segments or pieces instead of doing all the treatment simultaneously. Break the treatment up into smaller segments or pieces.
Treatment would be performed such that some of the definitive restorations are placed now, a few more restorations are completed the following year, and so on, spreading the overall treatment (and costs) over many years. I would like to discuss the “how to” behind phasing treatment in this article. To begin this conversation, I would like to break the process into two distinct parts: the planning and treatment phases.
The Planning Phase
In the planning phase, once the diagnosis and etiology have been determined, the entire treatment plan is developed per the Facially Generated Treatment Planning process, as if the treatment is to be completed all at once. This includes how tooth/tissue position will be altered (e.g., orthodontics, perio surgery, restorative).
Once the overall treatment plan has been developed, the options on how break the treatment up into smaller segments needs to be determined (so that some definitive restorations can be placed now, and others over time). To help in this process, ask yourself the question “what needs to be done to get the occlusal planes leveled?”
Leveling of the occlusal planes can be accomplished temporarily on some teeth (re-shaping, composite, prep-provisional) while definitive restorations are placed on others. The purpose behind leveling the occlusal planes is to manage the esthetics, but more importantly, to manage the occlusion throughout the course of phasing as it is much more predictable to control occlusal forces with level occlusal planes.
The Treatment Phase
Once treatment is started (treatment phase) any areas of active disease needs to be managed. If active disease is not addressed first, the current problems will only get worse.
In addition, the etiology must be addressed to prevent further breakdown as treatment progresses. There would be nothing worse than the first set of restorations failing before the entire treatment is finished.
Patient Example
This patient presented with a treatment plan from her current dentist for a full-mouth reconstruction with crowns and veneers, utilizing implants in all four posterior sextants. (Figs. 1A–1C)
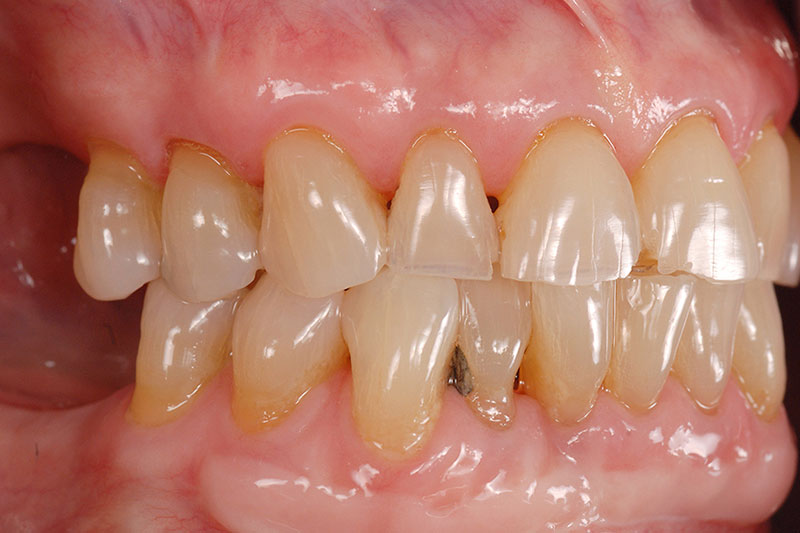

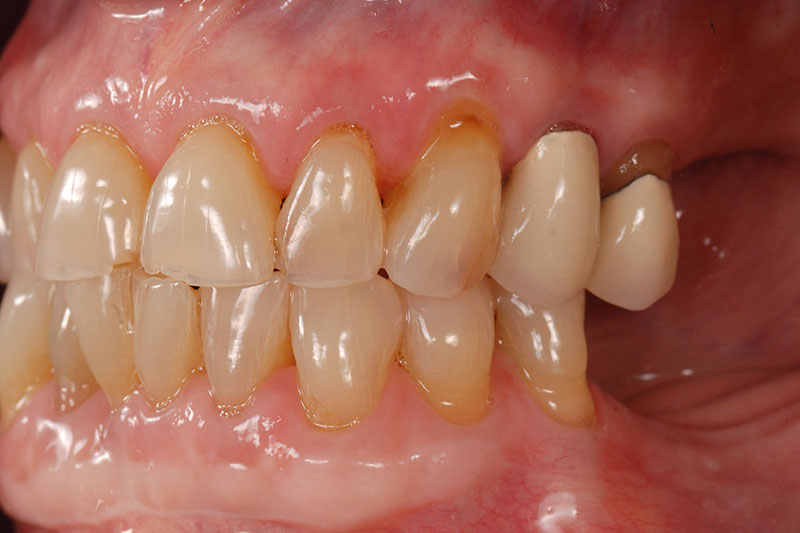
The patient’s treatment goal was to improve both the esthetics and function, as she didn’t feel she could eat normally without breaking the thin edges of her anterior teeth. The treatment plan I presented utilized composite resin to help restore the esthetics and function.
Given that she had been without molars for many years, she was fine with not having these teeth replaced. The treatment plan was developed using the FGTP process, beginning with determining the maxillary incisal edge position. (Figs. 2A-2B)
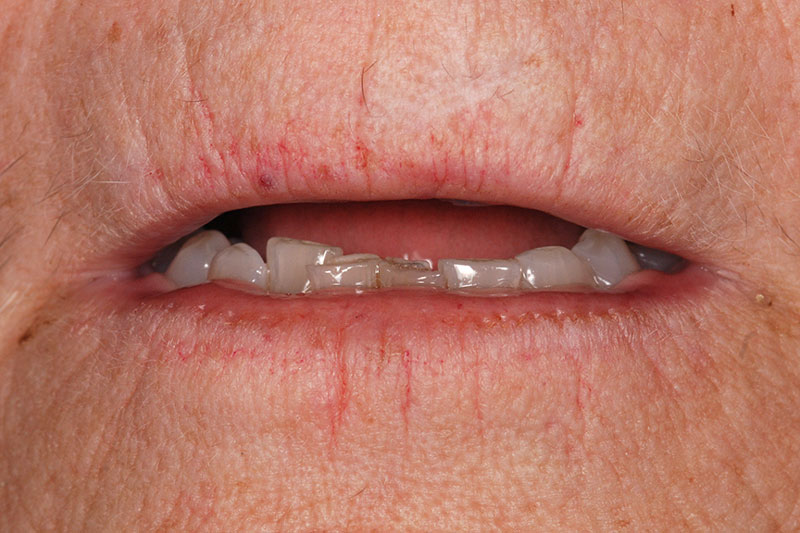
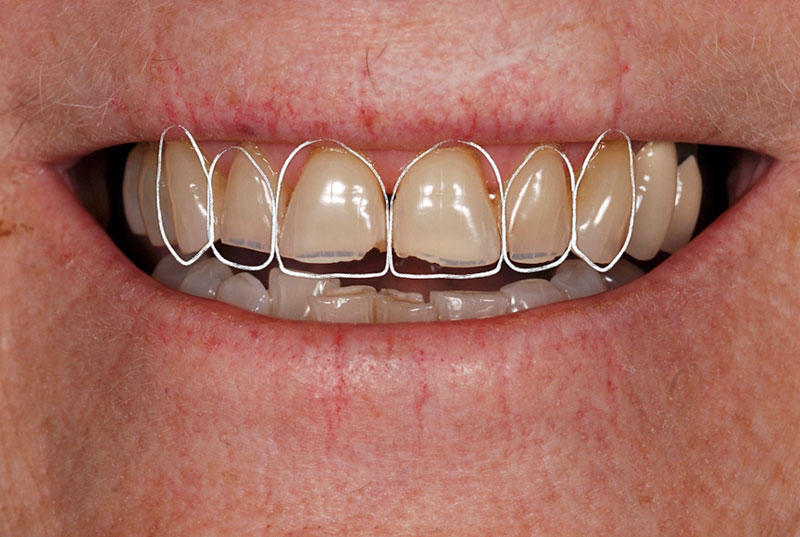
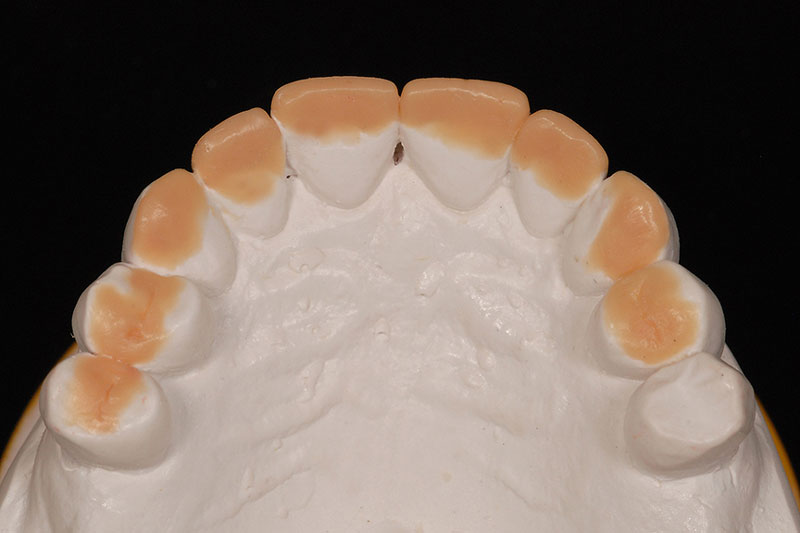
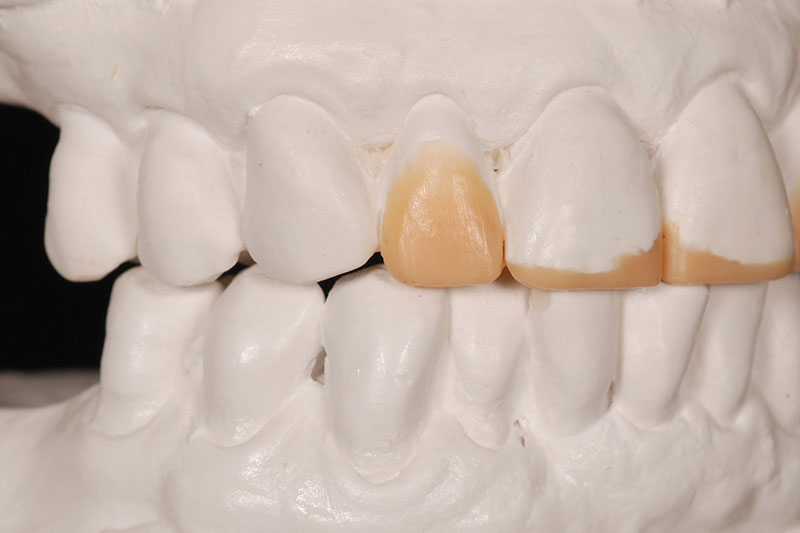
The entire occlusal thought process and design was worked out on mounted casts utilizing a diagnostic wax-up. (Figs. 3A-3C)

The placement of the direct composite was performed in a single visit and was well tolerated by the patient. (Figs. 4A-4C)


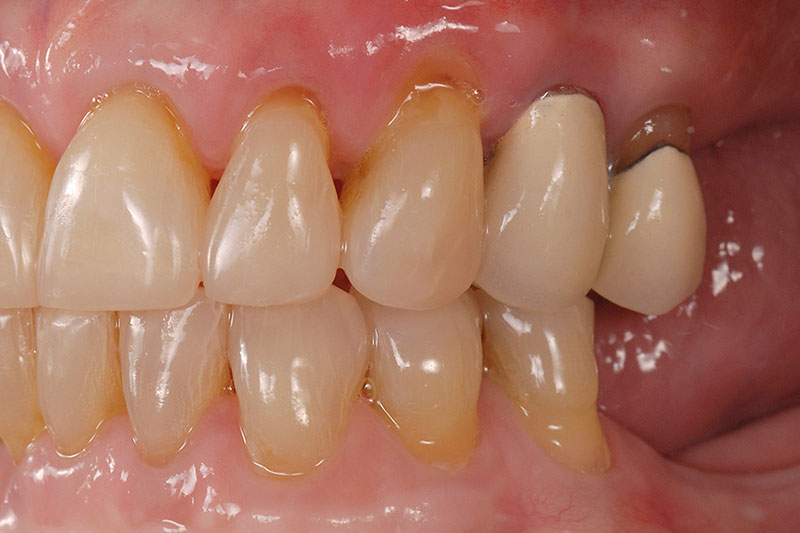
Although the composite in this situation was used as the definitive restorative material, this is essentially the same technique/sequence that would have been used if the definitive restorations had been ceramic. The desire was to phase the treatment.
References
- Hemmings, K. W., Darbar, U. R., & Vaughan, S. (2000). Tooth wear treated with direct composite restorations at an increased vertical dimension: results at 30 months. The Journal of Prosthetic Dentistry, 83(3), 287-293.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Greggory Kinzer
Date: July 8, 2020
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


