Restorative Design and the Sterile Pencil
Esthetic and functional restorative dentistry depends on outcome-based thinking, design, and application. Correct tooth preparation reduction is essential to achieve predictable and long-lasting ceramic restorations. Inadequate ceramic thickness may result in improper shade, inadequate strength, and potential restoration failure due to fracture. It is critical to incorporate strategies and techniques for accomplishing predictable results during the tooth reduction phase of restoration.
Every material requires a specific thickness for strength and durability. In the Restorative Design workshop, a systematic tooth reduction approach is outlined. Depth reduction burs are utilized to provide controlled tooth removal. The design of the bur eliminates the guesswork of tooth reduction. The definitive depths produced from these burs guide the restorative dentist toward an ideal preparation contour.
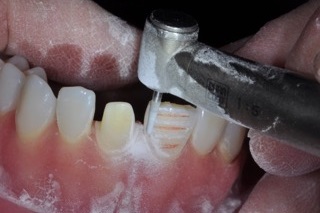
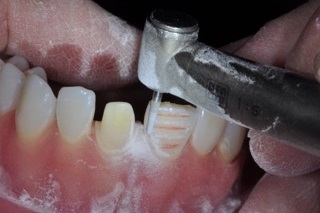
The technique of drawing red pencil lines in the depth cuts is introduced to provide a frame of reference as to the extent of tooth reduction. The participants are instructed to maintain these red lines throughout the tooth preparation. Visual evidence of these lines after reduction and refinement provides confidence regarding the amount of tooth removal.
There is never a workshop in which at least one participant questions the sterility of the red pencil. In the past, we have jokingly asked the participants to take the “sterile red pencil” from the drawer to mark the teeth. Generally, there is laughter from the group. But in reality, there is genuine concern for having our instruments and materials “sterile.” Maintaining cleanliness in all we do is in the patient’s best interest.
The question of sterility is important and valid. As dentists, we practice sterile technique routinely. Instruments, gauze, and cotton rolls are sterilized in our packs and trays for each patient. We don’t think twice about that process. But the “sterile pencil” question was bothersome to me. An assumption was inferred that red pencils could not be made sterile.
As I considered this dilemma, it occurred to me that my office routinely inserts wooden cotton applicators (“Q-tips”) into each of my instrument packs prior to sterilization. As they do not “burn up” during a high heat cycle, I proposed that red pencils could also be included in the packs.
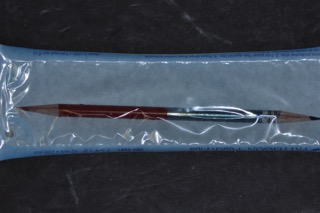

Pencils are made from graphite rather than lead. The solid graphite core is a combination of graphite and a clay binder. The casing around the graphite is typically made from wood, but plastic and other materials are also used. The casing is not bound to the graphite core. The consistency of the core determines the hardness or softness of the pencil. The more clay, the more complex the pencil’s lead.
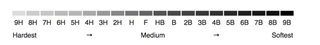
Pencils are classified by degree of hardness and blackness. The scale ranges from zero to nine. One end of the scale designates hardness, “H.” The other end is softness, “B.” The harder the pencil, the lighter the color. Conversely, the darker the pencil, the blacker the color. A #2H pencil is softer than a #3H pencil. A soft pencil will leave a greater trail of core material than a harder pencil.
Colored pencil lead contains a wax or oil-based pigment. The amount of color pigment determines the color intensity of the core. Colored pencils vary greatly in quality, concentration of pigment, solubility and softness.
I ran a test by placing a red/blue pencil into a sterilization bag. My biggest concern was whether the red lead would melt in the high heat of the autoclave. Depending on the amount of wax used, the pencil could be rendered unusable.


To my pleasure, I discovered that the red pencil successfully underwent the sterilization process. Aside from the outer paint covering blistering from the high heat, the pencil and point were intact. The prepared teeth depth cuts can be adequately marked with the sterilized pencil!
Multiple sterilization cycles will result in the complete loss of external red pencil paint. However, the pencil will continue to work for tooth reduction marking. I suggest sharpening the pencil after each use, prior to the subsequent sterilization cycle.
An alternative method for creating sterile marking pencils with sharp points could be to include a metal mechanical pencil in the patient packets. The mechanical pencil could be routinely sterilized and the pencil tip advanced, as needed, for sharpness.
As a side note, black pencils are not recommended for this tooth-marking process. Black graphite particles have the potential to become ingrained into tooth structure and previous restorations. This could negatively interfere with tooth shade and brightness value. Using a soft black pencil would be even worse.
I hope this article and experiment provide some insight into preparation design and eliminate any uneasiness around the “sterile” red pencil tooth-marking dilemma.
VIRTUAL SEMINARS
The Campus CE Experience
– Online, Anywhere
Spear Virtual Seminars give you versatility to refine your clinical skills following the same lessons that you would at the Spear Campus in Scottsdale — but from anywhere, as a safe online alternative to large-attendance campus events. Ask an advisor how your practice can take advantage of this new CE option.

By: Jeffrey Bonk
Date: February 27, 2019
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


