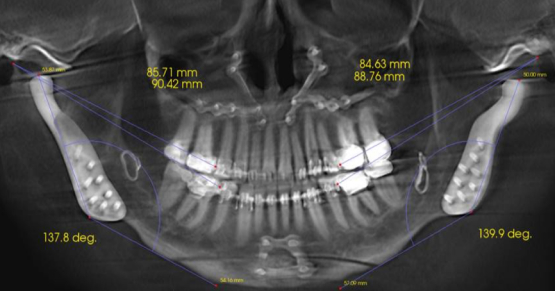
PCS: Evaluating Problems, Consequences and Solutions During a Consultation
“PCS” stands for Problem, Consequence, and Solution. In our practice, this system is not only used for clinical dentistry but can be applied to almost every area of our practice.
From a clinical perspective, I’m sure it comes naturally for most of us to think about the problems, consequences and solutions of a tooth with deep decay that is left untreated or a tooth with multiple cracks that the patient just wants to “watch.”
From a non-clinical standpoint, the same applies when we don’t make financial arrangements or when an appointment is not confirmed. For the sake of this article, we will focus on the clinical side of things and how utilizing a consultation to present what you see, review the consequences of inaction, and discuss treatment options can help you get more patients to say “yes” to treatment.

While taking the complex case planning workshop, a great piece of wisdom was shared — “You only see what you know and you only treat what you see.”
As I let that phrase sink in for a minute, I thought to myself, this really holds true and is applicable to every patient in our practice. I also thought to myself, now I have to get better at seeing more things, so I can enable myself to treat more things.
How to Help Dental Patients See Their Problem
This is where the “P” of PCS comes into play. Problems need to be identified before anything else. Spear Education has provided us with a great knowledge of dentistry and an effective system to perform the initial comprehensive exam, which, in turn, enables us to see more things and help patients achieve optimal oral health. We need to use this information to make our patients aware of what we see.
In our practice, we are typically making patients aware of things that they’ve never seen or heard before. Don’t get discouraged if the patients seem to be getting upset as you are telling them what you see. Just explain to them that you are giving them a tour of their mouth based on your observations.
This is where tools like the intraoral camera or digital SLR camera are very useful. I like to put the problems I see on a TV in the room for the patients to see. I feel most people are visual learners, and the ability for them to see it magnified on a screen really helps the patient own their problem(s).
Help Patients Understand Consequences
The “C” in PCS stands for consequences. I feel this is the most essential part of the equation. We constantly stress to our team that we want patients to want to do dentistry to avoid the consequences of inaction. We believe it’s the consequences of inaction that really motivate a patient to move forward with treatment.
Using the previously mentioned example, patients are usually quick to address a tooth with deep decay if we help them understand that the consequence of not treating that tooth could be a root canal.
Sometimes the tendency is to explain the problem, skip over the consequences and jump right into the solution. Again, we should do our best to focus on the consequences after identifying the problems. Once we discuss the problem and associated consequence, we typically hear patients saying, “what do we do about it?” or “how do we fix it?”
This is exactly what you want to hear. At this point, you know the patient is engaged and interested in doing something to correct the problem. When you feel the problems and consequences have been clearly identified and explained to the patient, the “S,” or solution, can be discussed.
Identifying Solutions for Optimal Oral Health
We don’t look at the solution as a decision that is made solely by us, and we never just hand the patient a treatment plan. We give treatment options and decide on a plan together after reviewing the pros and cons of each option. As a result, patients take more ownership of their oral health and are able to make more educated decisions moving forward. We’ve noticed that this approach has really helped increase our overall case acceptance.
So how does all of this apply to a consult? On some occasions, there just wasn’t enough time during a hygiene exam to cover the problems, consequences and solutions. If we felt we needed more time to discuss our findings, we would set up a separate consultation visit. This would give us the time to use the PCS model to our advantage. Using photographs, keynote presentations and patient education software, we are able to explain what we see, show potential consequences and review treatment options in a clear and concise manner.
To help identify patients we feel would benefit from a consultation, we set up “consult triggers.” We created these triggers based on the Spear model of EFSB: Esthetics, Function, Structure, and Biology. Here’s what our triggers look like:
Esthetics
- Patients unhappy with the appearance of their teeth.
The key here is to identify the patient’s specific concerns regarding their appearance. Is it the color, contours, shape, arrangement, etc.? A simple question to ask existing patients is, “Are you still happy with the appearance of your teeth?” If they are, we typically get a simple “yes” in return. If not, you can begin to investigate the patient’s concerns and the most logical way to move forward.
If appearance is the only trigger that exists, decide if it’s something that can be discussed during the hygiene exam or if you think the patient would benefit from a separate consultation.
Function
- An unstable occlusion — patient that can’t find a comfortable bite or feels their bite is changing
- TMD/muscle symptoms
- Evidence of patients going into centric relation
These are the types of conditions that are far too complicated to explain during a hygiene visit. We do our best to explain the problems that we see during that visit and explain to the patient the value of coming back for a consultation to help educate them on their current condition. Utilizing patient education software such as BiteFx can help the patient understand what’s going on and how it relates to their condition.
Structure
- Presence of structurally damaged teeth
- Cracks/fractures
- Multiple missing teeth
- Multiple teeth needing restorations
- Various types of tooth wear (attrition/erosion)
I’ve found that most patients who present with these types of problems rarely understand the potential causes or why they developed in the first place. A lot of patients attribute it to age. While age may be a contributing factor, we believe patients can benefit from understanding that there may be other factors involved, such as grinding their teeth or the presence of acid, that can result in the breakdown of their teeth.
We explain to the patient that we can give them back the structure that’s been lost, but the goal is to identify the underlying cause so we can prevent it from happening again. We’ve found utilizing a consult to review this information is much more effective than trying to review during a recall exam.
Biology
- Periodontal issues
- Radiographic pathology
- (Periapical radiolucency/resorption)
These types of issues are commonly reviewed during the recall exam with the assistance of intraoral photos and radiographs. We stress to our hygiene and assistant team to try and identify these biologic problems and take the appropriate records prior to us coming into the room. They should begin to educate the patient as to what they see and why they are taking the radiograph or photo.

By no means are they giving the patient a definitive diagnosis, but they can begin to come up with some possibilities. The hygienist or assistant then “hands off” the information in front of the patient, and we are then able to expand on what we see. This approach enables us to reinforce the problem and saves time, so there isn’t much need for a separate consultation.
That being said, at times there are multiple biologic issues going on that may require the assistance of a specialist such as a periodontist, endodontist or oral surgeon. If that’s the case, and we feel like there’s too much information to cover at a recall exam, we will reappoint a separate consultation visit to give the patient a clear understanding of how to manage the problems we discussed.
As for the actual consultation, we like to have up-to-date radiographs, mounted models, photographs and information from the most recent exam. There are also educational tools such as BiteFx, Spear Education software and the TMJ Tutor that can really help convey a clear message to the patient regarding their current condition. There’s not one right formula to prepare a consult for your patient. The key is to find what works best for you and use it to your advantage.
It’s always a good idea to get the entire team on the same page when identifying patients who would benefit from a separate consultation. Once everyone is on the same page and talking about dentistry in the “Problem, Consequence, and Solution” format, I believe you will see a noticeable difference in patients accepting treatment and being able to do the type of comprehensive dentistry you’ve always envisioned.
SPEAR NAVIGATOR
Transform how your practice runs by engaging the team through
coaching and training
A guided path to excellence through structured coaching and self-guided resources that will align your team, streamline processes and drive growth. Transform your practice by implementing Spear’s proven playbooks for developing and retaining a high-performing dental team.

By: David Monokian
Date: December 6, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts