Technology Doesn’t Always Make for Better Dentistry
As restorative dentists, our training and experience has taught us that diagnosing a problem of dental origin can be very complicated, and this is very true.
It’s also true that when the approach to the diagnosis is systematic and verified every step of the way, meaning that any necessary therapeutic step is also interpreted for its diagnostic information, we can usually reach a solid diagnosis. We can also help the patient see that this is a different kind of practice and that you’re a different kind of dentist.
A new patient came to me with this chief complaint: “My front veneers keep breaking. My dentist has fixed them three times, but they keep breaking. I have to travel to Africa in the not-too-distant future and I’m afraid they’ll break again.”
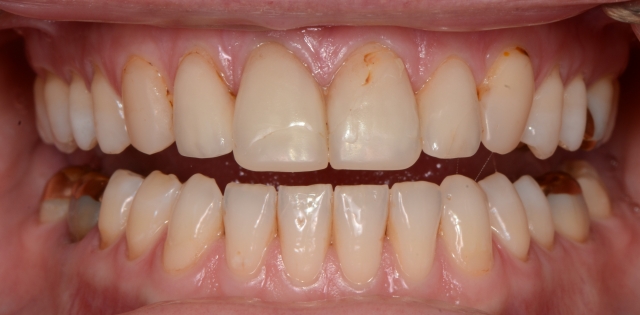
You could look, judge what that previous dentist did, and think: “Dang, what cheap bonding system did this dentist use? I can do better than that!”
Cut them off and replace them, and maybe you’ll get lucky. But you might have missed the real reason for the failure and have the patient appear back in your chair with pieces in her hands and a very unpleasant look on her face.
I slowed down and looked at her through the lens of co-discovery. I did my usual evaluation following the AEFSB protocol I learned in Spear seminars and workshops, looking at the teeth and smile in relation to the facial esthetic parameters, joints, muscles, occlusion, tooth structure, perio, soft tissue, endo, and bone.
Several interesting discoveries followed. First, I recognized that the teeth were not visible under the lip with the lip at rest.

I also noted that tooth wear was not distributed evenly on the dentition. The lingual aspect of the maxillary anterior teeth looked severely worn.
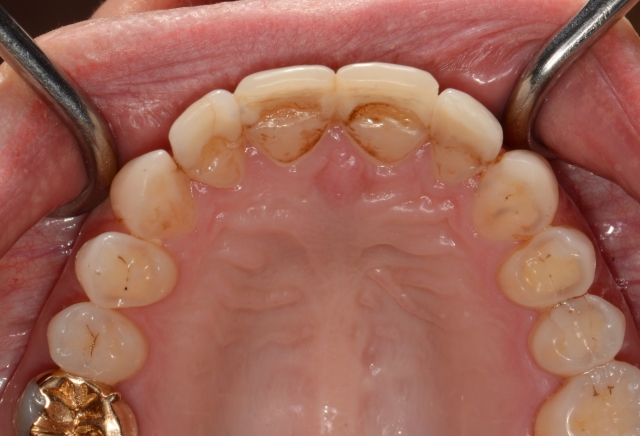
I pulled out the leaf gauge to confirmed the joints could be loaded, and began progressively decreasing the number of leaves to discover the first point of contact at the seated condylar position. I discovered a posterior initial contact at a significantly open position that deflected the mandible so the mandibular anterior teeth ran into the lingual aspect of the anterior teeth at the very place where her veneers had been breaking.
The patient felt the first contact, felt the shift, and felt the lower teeth contact her front teeth. In that moment, the patient had an epiphany. Her eyes opened wide, she quickly opened her mouth and said, “Wow, is that why I keep breaking the veneers?!”
Good question. Could be. Let’s find out!
I fitted and adjusted an anterior bite, eliminating the interference and allowing for muscular deprogramming. Upon appliance removal from the mouth, the patient experienced hitting on the same first contact we found with the leaf gauge and the shift into her front teeth. Soon, after a few closures to swallow, the contact disappeared to her and the teeth felt like they fit again immediately upon closing. She understood the programming of her engram.
We mounted diagnostic casts in centric relation based on a leaf-gauge bite registration before the first point of contact, confirmed the same posterior initial contact and shift we saw in the mouth, and waxed up a new occlusion by making changes that created coincidence between the seated condylar position and maximum intercuspal tooth contact. These changes provided for space in the anterior to create appropriate form and smooth function.
We designed the teeth to be restored and fabricated milled provisionals by scanning the wax-up and creating a set of PPMA (Anaxdent Multi) provisional restorations. These served as the “appliance” to test our theory regarding the stability of the restorations. We bonded the milled provisionals and gave the patient the opportunity to test the new occlusion for about three months.
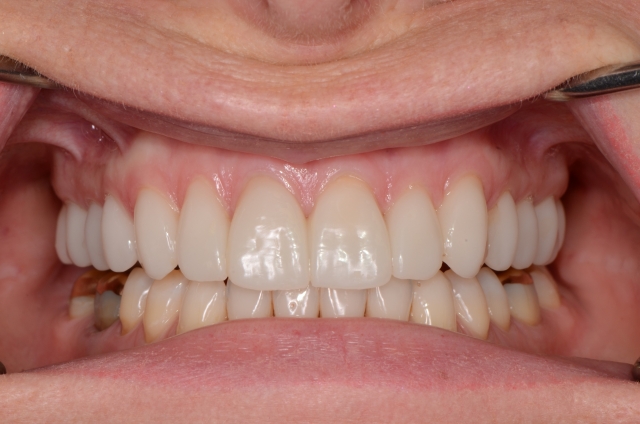
The provisionals remained completely stable. The patient noted these changes and told me that she felt much more relaxed, more rested, more comfortable, more confident. Stability is a beautiful thing.
We finished the case using the designed-and-adjusted provisionals as our guide. Happy patient, happy dentist. Much more enjoyable trip to Africa.
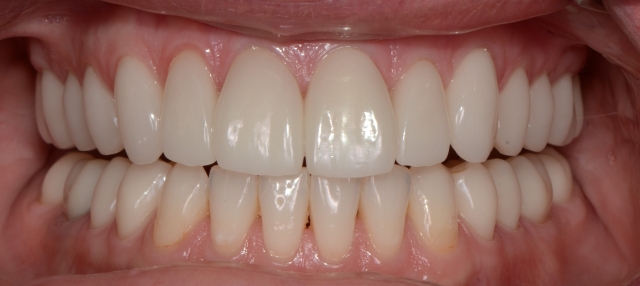
The AEFSB protocol, slowing down to see more, and using a leaf gauge as an aid to locate seated condylar position — all things taught in the Occlusion in Clinical Practice workshop — meant the difference in the success of this significant restorative case. In many instances, it’s not the sophistication of our technology that makes us better dentists; it’s the knowledge to know when and why we need to slow down, to observe more, and to better understand what we are seeing that makes the difference. Application of straightforward protocol in diagnosis and planning is often the key.
Technology can assist in many dilemmas, but it often is not necessary to understand and address the problems with which our patients present.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Costin Marinescu
Date: January 11, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


