Three Techniques To Help Quick-Trigger Gag Reflex Patients

“How long does the impression have to stay in my mouth?”
Whatever your answer, 90 seconds or four minutes, the follow-up from the patient is typically some form of a deep breath and the explanation “I am a gagger,” to help set the tone for what we’re about to see. The anxiety is palpable — the patient feels the tension, as well as the dentist or the assistant about to make an impression.
Certainly, there’s a range as to what triggers the patient’s protective gag reflex. At one end of the spectrum is a patient who simply cannot tolerate anything in their mouth — toothbrush, mirror, or explorer. The other end of the spectrum relates to people who’ve simply had a bad experience with impression material oozing to induce panic in an attempt to maintain an airway.
How do you distinguish between a patient you can work with in the office versus one who should be referred out for counseling or treatment? We all want to help the patient. It’s rewarding to work through this challenge, although it’s much more rewarding to reminisce with the patient after working through the challenge.
The key factor separating patients with a manageable gag reflex relates to the sensitivity of the glossopharyngeal nerve (IX), with fibers in the posterior third of the tongue. A couple of manageable examples:
- A full-arch impression, alginate or silicone, with material oozing past the posterior extension of the tray and, as soon as it hits the patient’s tongue, creating an uncomfortable cycle alternating between controlled breathing and the convulsion associated with a gag reflex.
- A complete denture where the patient is able to tolerate the prosthesis onlyfor a specified period of time before they give up and remove their teeth out of frustration. It’s easy to imagine the posterior third of the tongue glancing across an abrupt transition between the soft palate and either the impression material or the posterior extension of the denture base.
How is a full-arch impression a manageable gag reflex situation? Adding boxing wax (Fig. 1) or Scotch tape to form a barrier simply to inhibit the flow of impression material is a simple trick that makes a difference for our patients.
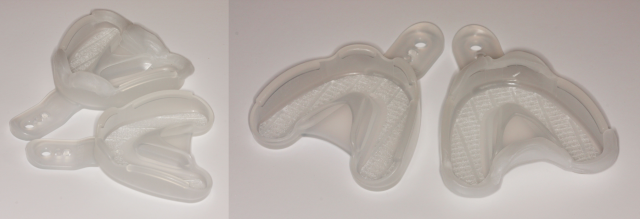
The important part is in helping the patient understand the cause of the gag reflex (back third of the tongue in contact with impression material), what you’re doing to help manage the feeling (creating a barrier with wax or tape to limit the ooze of material), and what they can do during the impression process at the moment the patient feels uncomfortable (position their tongue to avoid contact). The discussion helps the patient feel as though you have listened to their concern and, more importantly with the demonstration, that you understand their concern as well. Dr. Bob Winter has written a great article, “Tape Your Trays,” on this very topic.
Technique 1: Distraction
Distraction helps to orient the focus away from the trigger to the gag reflex. Telling the patient to breathe through their nose and lift their feet off the chair are simple and quick ways to distract the reflexive action, particularly if the first time the reflex becomes apparent is while making the impression.
Making use of simple pressure points provides another alternative; however, the technique and location of pressure points must be demonstrated in advance of the impression.
Try these simple pressure points:
- Have the patient squeeze their thumb by wrapping the four fingers of the same hand around the thumb — a fist with the thumb inside.
- Have the patient take their right hand and pinch the area between the thumb and index finger of their left hand.
- Have the patient press their thumb just below their lower lip and above the chin — while this creates a pain point, the success relates to the distraction away from the trigger to the gag reflex.
There are several other techniques that help to disengage the gag reflex and expand the working area. You can use topical anesthetic in the soft palate or tongue area, or simply add salt on a patient’s tongue to help work through a short-term challenge in the office. Dr. Jeff Lineberry has written a great article with some more tips: “Top 6 Methods for Managing Gagging Patients.”
Helping the patient understand the gag reflex while simultaneously gaining confidence in their ability to conquer this physiological or psychological barrier creates a long-term win.
Technique 2: Expansion
Expansion of the zone that triggers the gag reflex is another technique that requires the patient’s participation, particularly in the time between dental appointments. One method that can work with a dedicated effort is to have the patient work with a toothbrush or a tongue scraper with a goal of gaining some comfort in the sensitive areas that create a quicker-than-normal response to the gag reflex.
How about patients who are in a situation where they are working to tolerate a removable denture prosthesis? A record base made with the Ministar can help to provide a simulation of expanding the area of palatal coverage for an upper denture. The record base can be made of Copyplast covered by Splint Biocryl, where the patient can be given something to take home and wear in a concept similar to successive trays used to move natural teeth. Multiple record bases can be made where the extension toward the soft palate can be made progressively longer in an attempt to expand the patient’s zone of tolerance for coverage of the palatal aspect of the maxilla.
The question comes up as to how to distinguish between a patient in need of a serviceable complete removable upper denture you can work with in the office vs. a patient who should be referred out for treatment. How can we help the patient who is unable to tolerate their dentures without entering into a panic cycle that includes a gag reflex without taking a considerable amount of chair time to work through the process?
Three features to look for when evaluating a patient with a sensitive gag reflex in need of a complete denture:
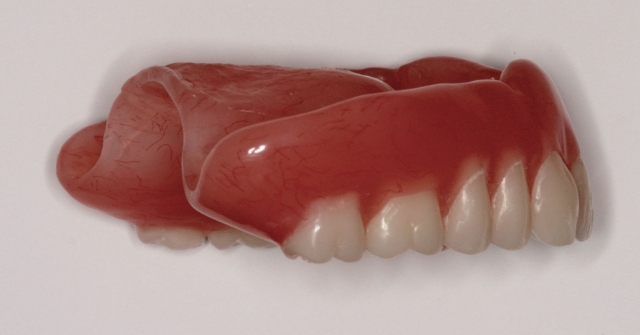
- Thickness of the existing acrylic base, where the space available for the patient’s tongue is limited. Think about what happens during a reline procedure, where more acrylic is cured onto the intaglio surface with the goal of improving the adaptation to the supporting tissues. If a patient has an ill-fitting complete denture that is tolerable, it may be easier to make a final impression using the familiar contours of the existing denture as a custom tray. The goal is ultimately to make a new prosthesis while limiting the thickness of the acrylic base by making a bilaminar thermoplastic record base with a MiniStar using Copyplast and Splint biocryl as the two layers, as shown in Fig. 2.
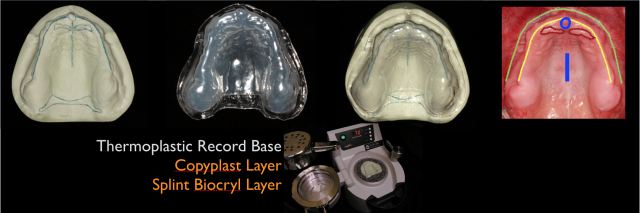
- The thickness of the denture base at the distal extension. It’s important to distinguish between the thickness at the distal extension and overextension onto the soft palate past the vibrating line. The function of the posterior palatal is to compensate for processing error, where the palatal area would rebound following removal from the master cast after processing. The thickness would allow for contact to maintain the seal of the upper denture. Today, with more advanced techniques to limit processing error, the idea of the posterior palatal seal is to create a positive contact where the thickness can be modified to allow for beveled contour or a feather edge. Think about the glossopharyngeal nerve fibers in the posterior third of the tongue: If the patient cannot feel a noticeable transition between the soft palate and the start of the denture base, then the trigger for the gag reflex has been mitigated. Fig. 3 demonstrates the thickness in the posterior palatal seal area before adjustment to create a beveled transition or a feathered edge with minimal thickness at the posterior extension of the denture base.
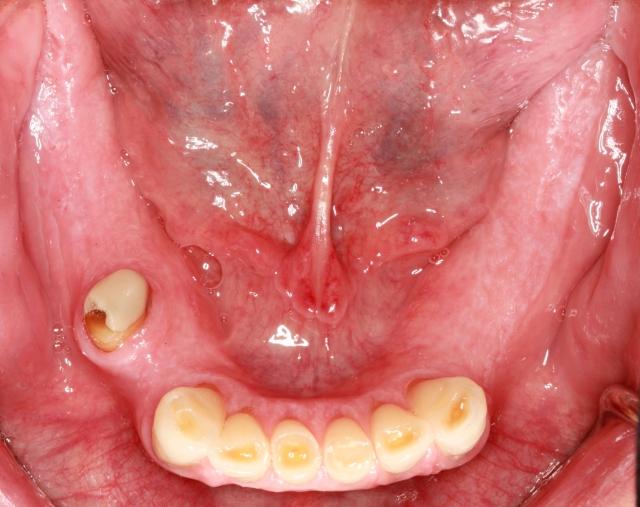
- The opposing occlusal contacting surfaces can also contribute to the patient’s ability to tolerate the palatal coverage of a maxillary removable denture. A patient who has full stabilizing contact with lower teeth is very different than a patient with an upper denture opposing lower teeth in the canine-to-canine area. Imagine the challenge to the seal of an upper removable denture when the only functional opposing contact is in the anterior segment, as would be the case with Fig. 4. When the denture comes loose in the posterior segment, a cycle is created where the protective reflex is initiated by the contact with the posterior third of the tongue brushing against the posterior denture base that has dropped down. In a contrasting thought, it might be interesting to investigate sleep apnea for a patient curiously devoid of a trigger to the gag reflex.
Technique 3: Multidisciplinary
The multidisciplinary management of a sensitive gag reflex becomes an option to help patients for a variety of reasons.
- Counseling may be beneficial for psychogenic etiology such as fear, anxiety, apprehension, visual or olfactory stimuli, or simply an overactive imagination.
- Involvement of a psychiatrist may be beneficial when working with medications deigned to depress the parasympathetic nervous system.
- There can be several etiologies that may or may not be discovered during a routine dental examination, such as a history of stomach cancer or gastrointestinal disorders as well as history of sexual abuse.
One possibility for helping patients through the process, particularly when working with a quick trigger to the gag reflex, is to sedate the patient while maintaining the airway. It is easy to see that what would seemingly be a simple, routine procedure in the dental office could become quite involved for some patients.
Certainly, digital image capture is available for tooth- and dental implant-supported restorations, with cameras that have become smaller and much more tolerable to patients. It is likely that digital image capture will eliminate the need for impression materials, particularly for edentulous patients similar to what’s possible with teeth and dental implants. It’s also possible with today’s technology to work with a dental implant-supported prosthesis to simulate the form and function of natural teeth while avoiding the palatal coverage of a maxillary complete removable denture.
(Click this link to read more about digital dentistry.)
It is also possible that a new technique or perhaps a new medication can create a situation to help the patient with a quick trigger to the gag reflex. At present, success depends on clinical management that includes the chairside manner, patient participation, and a technical approach that communicates and demonstrates empathy.
I look forward to hearing or reading about your experiences!
SPEAR Membership
Learn Faster. Treat Better.
Whether you have 10 minutes or time to dive deeper, Spear Membership gives you the learning, tools, and support to keep improving.
Choose the level of support and structure that fits your goals.

By: Doug Benting
Date: June 8, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts