Solving the Silent Epidemic of Cracked Teeth
At a recent Spear Study Club group meeting, one of our specialists in the group, an endodontist, shared a great topic of discussion and one that has been of personal interest: cracked teeth. We reviewed what the current research is suggesting and what is to come in this ever-evolving area of discussion and research.
(Getting to hear varying experiences and points of view is just one of the many great perks about having a Spear Study Club. Click this link to learn more.)
In Part I of this series, I will discuss some of the basics on cracked or fractured teeth, including risk factors and some findings to consider. In future articles, I’ll review the different types of cracks and fractures and discuss restoring fractured and cracked teeth.
The Silent Epidemic
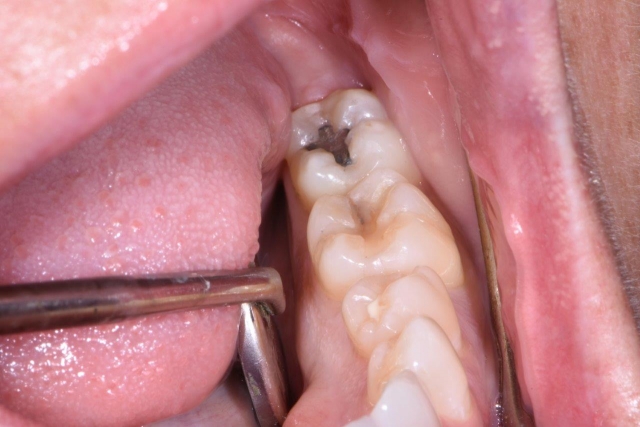
Cracked teeth were described in 2007 by David Clark in Dentistry Today as an epidemic, and were also described as such at the 2015 American Association of Endodontists. Cracked teeth are now recognized as the third leading cause of tooth loss and as such, it led the AAE to recently form a Special Committee on Methodology of Cracked Tooth Studies.
Cracked teeth or cracked tooth syndrome has for many years been used as a diagnosis for a tooth that often has pain on biting, thermal sensitivity and, at times, even fractures or breaks. Fracturing of teeth is a poorly understood process and finding fractures or cracks in teeth is often an observation, not a diagnosis. The current definition of cracked teeth by the AAE for 2015 is “a thin surface disruption of enamel and dentin, and possibly cementum, of unknown depth or extension.”
Many times, cracks/fractures are found in teeth on a daily basis in the restorative practice, especially after removing an existing restoration, having little to no symptoms. This can be described as an incomplete fracture if it involves one marginal ridge and a complete fracture if it involves both marginal ridges. It is a silent situation until the fracture worsens.
(Sound familiar? Decay often is similar in nature; it is often seen well before it causes pain and symptoms in our patients.)
Hence, the reason I have described this as a silent epidemic: it is often an observation in our patients well before it becomes symptomatic with pain and sensitivity, leading to a diagnosis of a cracked tooth syndrome. In a recent study,1 cracks in teeth were histologically detected and cracks in all teeth were colonized by bacterial biofilms. When the cracks reached the dentin, dentinal tubules were invaded by bacteria, leading to inflammatory cell infiltration into the adjacent pulp tissue. The pulpal response is “based on the location, direction, and extent of the crack.”1 Not only do we have to be concerned about overall structural stability of the tooth and fracture, we also have to keep in mind that bacteria are invading the fracture/crack as well and have to be managed.
Diagnosing Cracked Teeth
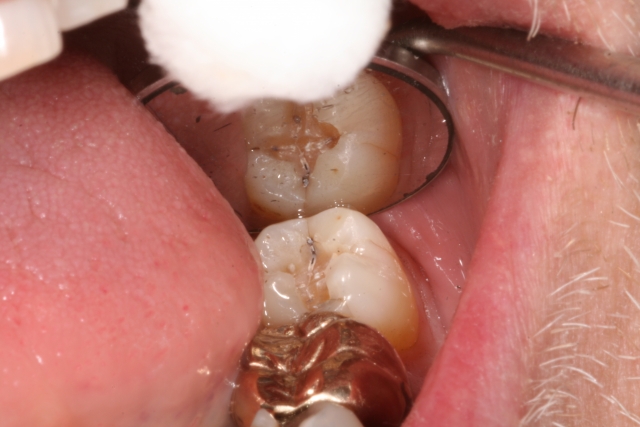
If your patient comes in with no symptoms, how and when can you tell if a tooth is cracked without symptoms? First and foremost, magnification and visualization are key components. How much magnification? Often in general dental practices, we utilize loupes up to six times magnification along with intraoral cameras to help see and diagnose cracks, but 13 times is the minimum needed to seek cracks/fractures visually.2,3 It has been shown that we can also use staining such as with methylene blue in addition to magnification to help identify cracks.4
We can also use a high-intensity, focused light for transillumination to help us visualize incomplete fractures/cracks in teeth. Without proper magnification and other techniques (use of a surgical operating microscope, which is found on a regular basis in most endodontic practices), and with no symptoms present, fractures in teeth can be challenging to visualize and/or identify and subsequently, to treat appropriately.
Why are so many teeth fracturing/cracking, leading to eventual pulpal necrosis or tooth loss? There are many reasons that cause fractures/cracks — weakened tooth structure due to large previous restorations and the common “G.V. Black” cavity preparations, caries, resorption, heavy mastication, clenching/grinding/parafunctional habits, and trauma, to name but some of the main culprits.
Which teeth do we observe and are frequently diagnosed with fractures? We see it most frequently in mandibular molars, then maxillary premolars, and upper first molars. Interestingly, it is more common in women than men, and we rarely see them in anterior teeth.
(Click this link to learn about utilizing Facially Generated Treatment Planning in wear cases.)
But what about when the crack/fracture extends deep enough to cause pain and sensitivity? It’s important to gain clarity of the current situation by gathering information about the patient’s history. When patients have pain associated with a cracked tooth, it can mimic or be similar to many other common diagnoses in dentistry, including, but not limited to, periapical or periodontal abscess, loose crown/filling, parafunctional habits/bruxism/clenching, sinusitis (upper teeth), loose teeth, etc. You can ask questions like, “Have you cracked other teeth? Can you point to the tooth in question? Any history of an event or trauma or biting down on something hard? Do you grind your teeth? Have you had any recent dental treatment?”
Visually, we have to be observant of our patients and look for wear facets, cracked restorations, hypertrophy in jaw muscles, and other missing teeth, craze lines, etc. We also must do an examination that ideally reproduces the symptoms that the patient is experiencing, but also know that just because we can’t reproduce the symptoms, it does not mean the tooth is not cracked. We need to do an examination looking closely at the area in question, as well as exploring the tooth in a tactile way for any “sticks,” pain or irregularities of the tooth surface. This can be done by variety of methods, including bite tests (a Tooth Slooth is a nice tool to use and isolate individual cusps/teeth), vitality testing, magnification, transillumination, visual and tactile examination, periodontal probing for isolated pockets, radiographic examination, including CBCT 3D exams, and even removal of an existing restoration.
Newer technology using quantitative light-induced fluorescence (QLF) is showing promise in helping detect cracks/fractures in enamel.5 Along with dental optical coherence tomography,6 these new pieces of technology may be the future for early detection and prevention of cracks and fractures and, hopefully, helping our patients avoid cracked-tooth syndrome.
Special thanks to our endodontic specialist and Spear Study Club member Luis A. Charmorro, DMD, MPH, for sharing his information and wealth of knowledge on this topic and sharing freely with me and our group.
References
- Ricucci D, Siqueira JF, Loghin S, Berman LH. The Cracked Tooth: Histopathologic and Histobacteriologic Aspects. Journal of Endodontics 2015;41(3):343–352.
- Clark DJ, Sheets CG, Paquette JM. Definitive Diagnosis of Early Enamel and Dentin Cracks Based on Microscopic Evaluation. Journal of Esthetic and Restorative Dentistry 2003;15(7):391–401.
- Clark DJ. The Epidemic of Cracked and Fracturing Teeth | Dentistry Today. Dentistry Today 2007.
- van As GA. Evaluation of Enamel and Dentinal Cracks Using Methylene Blue Dye and the Operating Microscope. dentalAEGIS 2007.
- Jun M-K, Ku H-M, Kim E, Kim H-E, Kwon H-K, Kim B-I. Detection and Analysis of Enamel Cracks by Quantitative Light-induced Fluorescence Technology. Journal of Endodontics, 2016;42(3):500–504.
- Lee S-H, Lee J-J, Chung H-J, Park J-T, Kim H-J. Dental optical coherence tomography: new potential diagnostic system for cracked-tooth syndrome. Surgical and Radiologic Anatomy Surg Radiol Anat 2015;38(1):49–54..
SPEAR Membership
Learn Faster. Treat Better.
Whether you have 10 minutes or time to dive deeper, Spear Membership gives you the learning, tools, and support to keep improving.
Choose the level of support and structure that fits your goals.

By: Jeff Lineberry
Date: July 23, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts