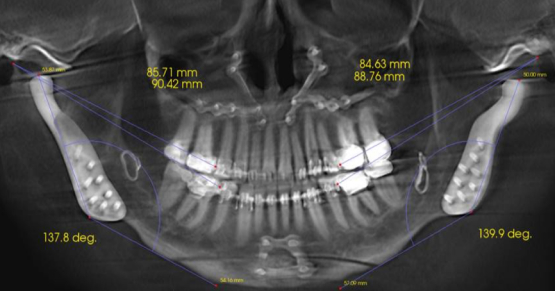
Managing Patients With Multiple Bites
Have you ever had a patient ask you which one of their bites you want when you ask them to close? If so, you know that if there is any restorative work needed, you’re in for some challenges managing their bite. The human bite is a complicated thing and while some individuals can adapt to changes in their bite, others respond poorly.
Patients who have multiple bites have the potential for bite issues. Take for example the different bites from the patient pictured below and the three different bites she showed me during her initial exam.
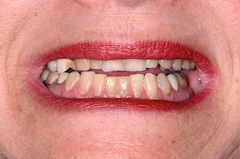
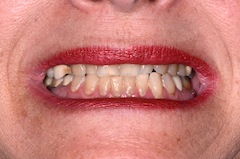
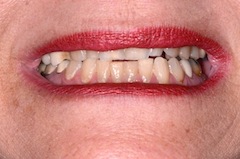
The best way to manage patients with multiple bites is to identify this fact as early as possible during your initial exam and before any restorative treatment. Once you know you are dealing with a patient with multiple bites it’s critical to make sure you know how you plan to manage their bite prior to starting treatment. It’s important to be sure that you and the patient realize and are accepting of the fact that no matter how you manage things, there will be increased risk in their treatment. The good news is that with the right training, knowledge and patience, you can often reduce the level of risk and make moving forward with these patients relatively predictable.
Typically my first step when treating these patients is to make them an occlusal orthotic. This is usually a lower full arch appliance fabricated from hard acrylic that simulates the desired post treatment occlusion. It’s worth noting that sometimes you will have to go through several occlusal schemes to find the one that will work for your patient. Both you and your patient need to be ready to spend the time needed.
Once you find a stable treatment position and bite on the appliance, the next step is to mount models in that position. You then have to figure out what how to make the patient’s teeth work the same way without the appliance in place. In some cases it may be as simple as an equilibration, while in others it may mean significant restorative work and/or orthodontics needs to be done.
The beauty about starting with an occlusal orthotic is that it’s typically reversible. This means that if you can’t get your patient to a stable, treatable point, if they simply stop using it they will typically (but not always) go back to their pre-treatment state. In many cases you will be able to find a predictable path forward with your patient; however, there are some cases where this may not be possible. Either way, the most important thing is to be as clear as possible with your patient about what to expect before you start treatment so that both you and your patient are comfortable.
John R. Carson, DDS, PC, Spear Visiting Faculty and Contributing Author [ www.johnrcarsondds.com ]
FOUNDATIONS MEMBERSHIP
New Dentist?
This Program Is Just for You!
Spear’s Foundations membership is specifically for dentists in their first 0–5 years of practice. For less than you charge for one crown, get a full year of training that applies to your daily work, including guidance from trusted faculty and support from a community of peers — all for only $599 a year.

By: John Carson
Date: April 14, 2014
Featured Digest articles
Insights and advice from Spear Faculty and industry experts