The Truth About Exceptional Veneer Temporaries
Fabricating veneer temporaries can be an entirely different experience than fabricating full crown temporaries. The minimal reduction typically done and fragility of the thin temporaries makes the process sometimes challenging. In fact, many dentists avoided making veneer temporaries because of how frustrating the process was. However, it makes it extremely difficult to communicate critical elements of tooth size, form and color to the patient and the lab unless we temporize.
By necessity the process starts with a diagnostic wax up incorporating the proposed changes in tooth arrangement, incisal edge position, smile line and tooth form. The information for the wax up can be efficiently communicated to the lab with photos that have drawings on them of the desired changes. From the wax up a matrix is formed out of putty, or an alginate impression can be taken of the wax up and poured in stone. On the stone model a clear matrix can be heat pressed from materials such as copyplast, which is very accurate but also easy to remove from the temporary during fabrication.
The fabrication itself can be performed a number of different ways successfully. Many dentists prefer using the shrink-wrap technique, where the temporary is made on the prepped teeth and not removed. This approach is the most efficient but has the challenge of needing to remove any flash from the margins in the mouth with a bur while not damaging the already impressed preparations.
It also is more difficult to fine-tune gingival embrasures since the temporaries aren’t removed after fabrication. Having said that many excellent dentists use this approach. I personally prefer to make an impression of the preps and create a model of either stone or die silicone on which to make my veneer temporaries using the putty or copyplast matrix. This has the advantage of excellent control of all variables including fit, form, embrasures and polish.
Another thing to be aware of throughout the process is shade – especially when you’re dealing with multiple teeth. What I like to do is make the temporaries a shade I’m comfortable with and then have the patient give feedback on the shade of the temporary. This is an excellent way of determining the patient’s desires for the shade of the final veneers.
As for materials, many of the autocure temporaries do an excellent job and have reasonable shades to work with, my most commonly used material in that family of materials has been Pro-temp from 3M. The keys to great temporaries are time and attention to detail. Although fabricating veneer temporaries the way I do takes a bit more time and requires you charge your patients a fee for the diagnostic wax up and the provisional or temporary restorations, that has never been an obstacle once the patient realizes why the diagnostic wax up and provisional are a necessity to create the best final result possible. In general, it costs about 30 percent more of the total case cost to deliver exceptional veneer temporaries from a diagnostic wax up with highly esthetic results.
I get asked frequently how you can charge for wax ups and temporaries on PPO or insurance patients. My answer is that PPOs and insurance don’t cover veneers anyway, so these patients know their treatment is an out of pocket expense.
I would also like to comment on a statement I have heard for years, “you shouldn’t make the temporaries too good.” I have always believed quite the opposite. Excellent temporaries not only function as a great communication tool with patients and the lab, they also promote soft tissue health which makes the seating appointment much easier and can be a huge “BRAND” builder for your practice.
I always love it when my patients get comments from others about how great their smile looks, and my patient can say, oh these are just the temporaries. Inevitably the person wants to know the name of the dentist doing the treatment. In fact, I would say that in the 1980s I built a huge reputation in my community as the person to see for Esthetic dentistry because of what people saw in my temporaries.
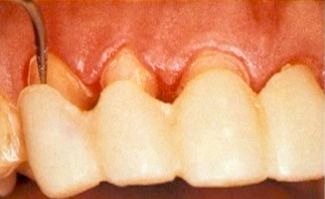
In conclusion, take a look at the image above from a publication discussing how the removal of temporaries encourages the tissue to bleed.
If you look closely, you’ll notice that this temporary doesn’t have any gingival or facial embrasures and the margins don’t fit properly. If your concept of a temporary is what is portrayed in this image you will undoubtedly struggle with bleeding tissues, and a limited ability to communicate esthetically with the patient and your lab. I would encourage you to do an anterior case doing the very best fitting and looking temporary you can make and see how big a difference it can make in the experience for you, the patient, and the lab.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Frank Spear
Date: February 23, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts