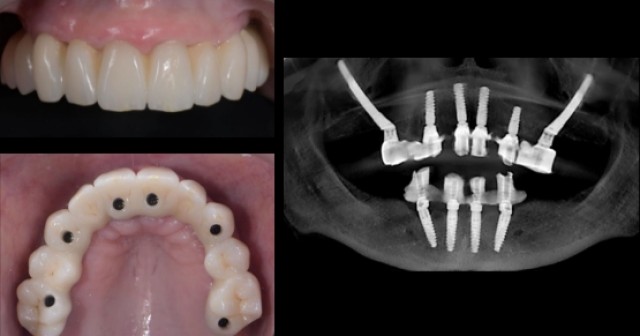
Zygomatic Implants vs. Bone Grafting for Full Arch-Solutions
Zygomatic implants are a safe and predictable first line of treatment and should be an essential addition to the modern interdisciplinary team — particularly when treating patients requiring a full-arch solution. In this article, I will compare zygomatic implants and bone-grafting procedures for these patients.
Zygomatic implants: Background and uses
Zygomatic implants have been around for a while, and most competent oral and maxillofacial surgeons and skilled periodontists should be comfortable managing and mastering the surgical technique.
There are multiple indications for the use of ZI:
- Patients with an atrophic maxillary arch
- Patients who have gone through maxillectomies due to tumor resection
- Patients with an alveolar extension of the maxillary sinuses
- In situations where we want to avoid grafting sinuses
- As a rescue treatment, when there are failing conventional implants.
Dr. Edmond Bedrossian’s 2008 bone availability classification system divides the maxilla into three zones. Based on bone availability, the classification provides implant design recommendations.
- Zone 1: Intercanine or premaxilla region
- Zone 2: Premolar region
- Zone 3: Molar region
Placing standard dental implants axially is recommended if the maxillary bone is available in Zones 1, 2, or 3.
- In cases where bone is available in Zones 1 and 2, the recommendation is to place 4–6 standard implants, tilting the distal fixtures to create a more favorable anteroposterior distribution of the implants (also known as “AP spread”) while avoiding utilizing long distal cantilevers.
- When bone is available only in Zone 1, placing 2–4 standard dental implants in the premaxilla and one bilaterally ZI is recommended.
- If no bone is available in either Zones 2 or 3, the recommendation calls for a quad-zygoma layout, which means placing two ZIs on each side.
Bedrossian’s bone availability classification system does not consider grafting the maxillary sinuses or the premaxilla; it circumvents them and places ZIs to compensate for the atrophic segments within the arch.
Zygomatic implants vs. bone grafting
When choosing between either grafted and nongrafted solutions, you must evaluate the three following areas:
Bone requirement
ZIs are suitable for patients with severe bone loss because they use the zygomatic bone as an anchoring point. This eliminates the need for a significant amount of bone in the maxillary arch.
Sinus grafts are typically performed when there is insufficient bone height in the posterior maxilla because of the expansion of the maxillary sinuses. This procedure adds bone material to create a suitable base for implant placement.
Surgical complexity
ZI surgery is considered more complex than traditional dental implant placement because of the proximity to the zygomatic bone and the need for precise placement. It requires expertise and broad surgical implantology experience.
Sinus grafts involve lifting the sinus membrane and placing bone graft material in the sinus area. While it is a delicate and meticulous surgical procedure, it is generally considered less complex than ZI surgery.
Treatment time
ZIs offer the advantage of immediate loading, meaning that provisional restorations can often be delivered on the same day as implant placement. This can significantly reduce the treatment time, compared with traditional implants.
Sinus grafts typically require a healing period of several months to allow the grafted bone to integrate and stabilize before dental implant placement can occur. This extended healing time may prolong the overall treatment duration.
Zygomatic implants vs. sinus grafting
Advantages of zygomatic implants
- Provides posterior anchorage in the case of atrophic maxilla.
- Represents a graftless alternative to the maxillary sinus and premaxilla grafting.
- Includes a definite immediate loading potential.
- Reduces clinical times.
- Provides financial benefits for the patient.
- Remains an arguably less invasive protocol, being it avoids additional surgical interventions.
- Is relatively simple.
Advantages of sinus grafting
- Increases bone volume.
- Is a relatively simple surgical procedure.
- Avoids more invasive procedures.
- Preserves anatomical structures.
- Contributes to long-term implant success.
How does this play out clinically?
Our patient is a 66-year-old woman who presented with three remaining teeth in the maxillary arch and a fixed-hybrid temporary reconstruction in the mandible. She came looking for a second opinion regarding treating her maxillary arch.
Her previous dentist suggested a similar approach to what was done in the mandible, which entailed removing the few remaining teeth and removing bone and soft tissue to place four implants for a fixed-hybrid provisional restoration.
Even though she went through this protocol with her lower jaw, she wanted to know if there were alternatives to treat her condition in the maxilla because the bone and tissue removal aspect did not appeal to her. She was told elsewhere that this was the only predictable way of treating her condition.
Even though there were only three remaining teeth, they were so severely compromised that they were hopeless; however, their presence, as well as the support provided by the flipper type of removable provisional restoration, helped enormously in preserving a rather pleasing gingival architecture, which would be destroyed if we chose a fixed-hybrid restoration.
This makes her a lip-tooth-ridge Class I patient according to the published classification. According to Dr. Mish’s classification, she is an FPI, which means her preexisting condition is conducive for an all-white, implant-supported fixed dental prosthesis without any pink ceramics.
The challenge is that bone availability is limited to her premaxilla, so we must either graft the sinuses to incorporate distal implants or bypass the sinuses and place one ZI bilaterally. Both approaches are perfectly doable and predictable because they’re supported in the scientific peer-reviewed dental literature. They also present nuanced implications that need to be reviewed and understood by the treating team and the patient, who is the ultimate decision-maker.
Her pneumatized sinuses do not allow grafting and implant placement simultaneously. This means we would need a staged approach — perform an initial procedure limited to grafting and a subsequent procedure for implant placement.
This translates to a significant increase in treatment time and financial commitment by the patient. However, bypassing the sinuses and placing a ZI bilaterally would expedite the overall treatment time and represent a financial benefit.
Once the patient understood the nuances between graft vs. a graft-less solution, she opted for a combination of anterior and ZIs instead of grafting the sinuses.
Case study
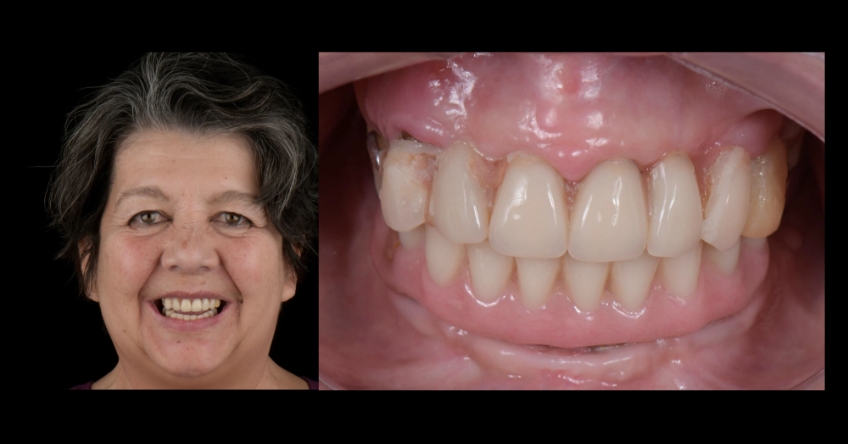
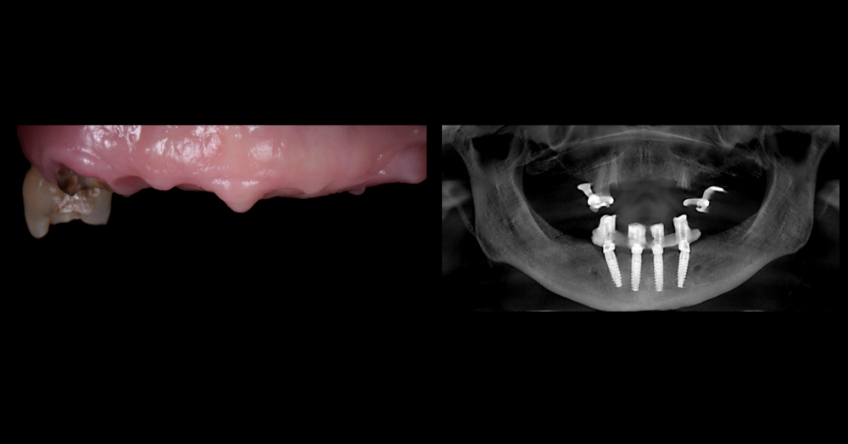
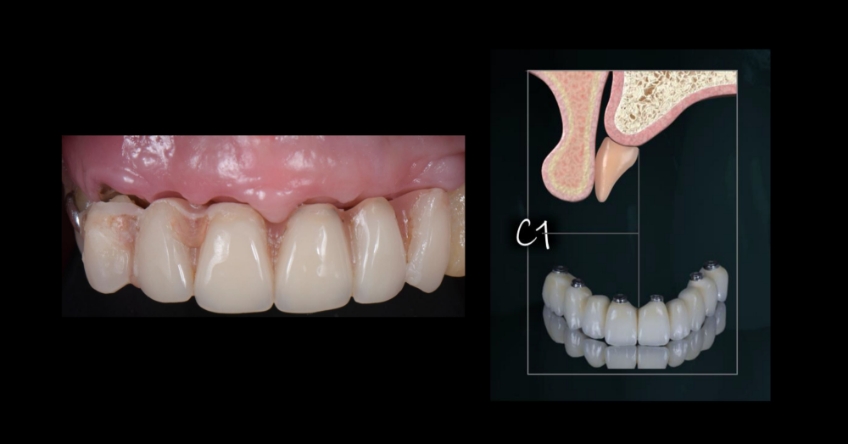
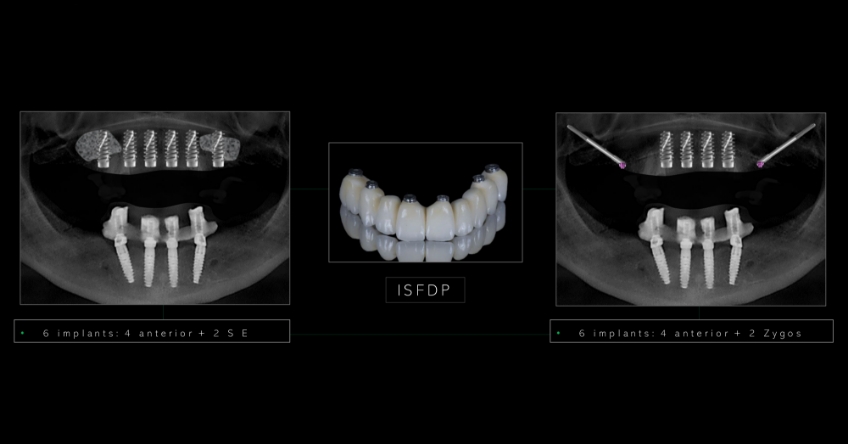
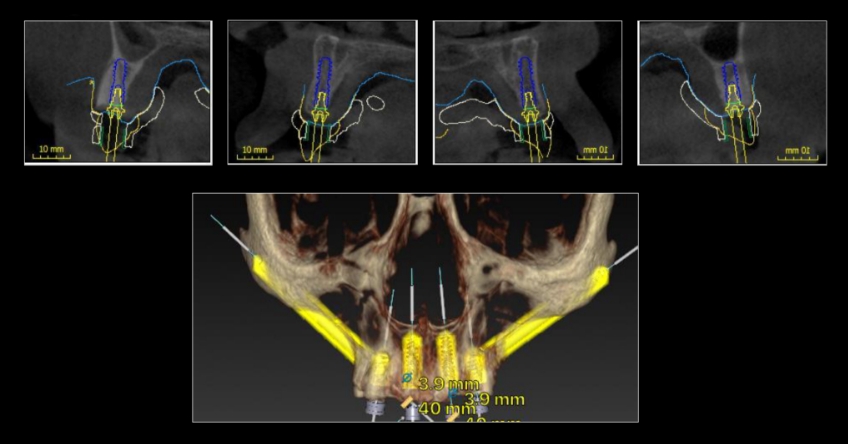
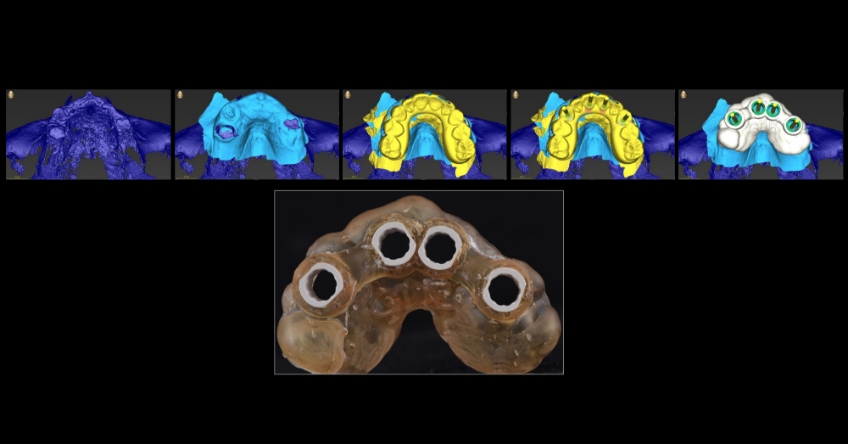
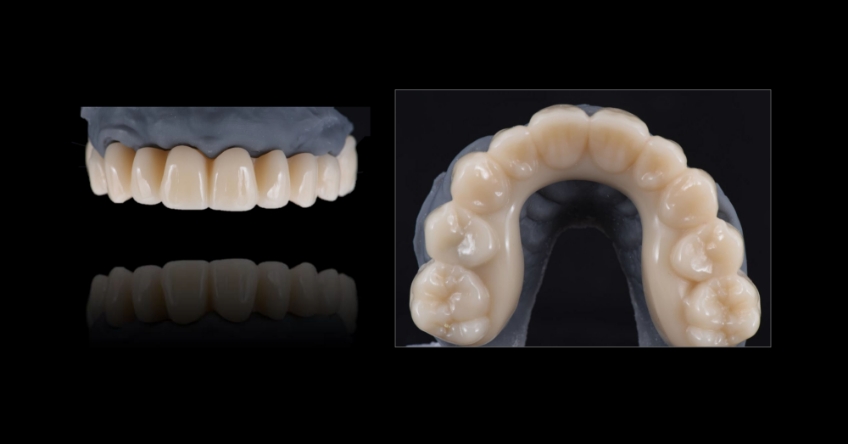
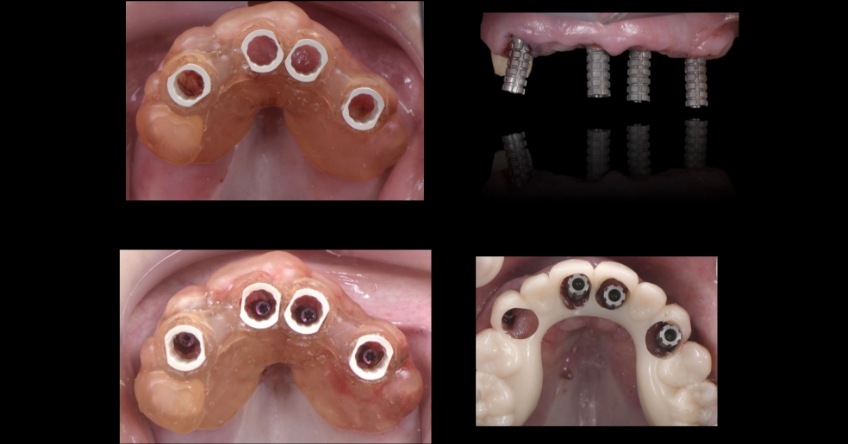
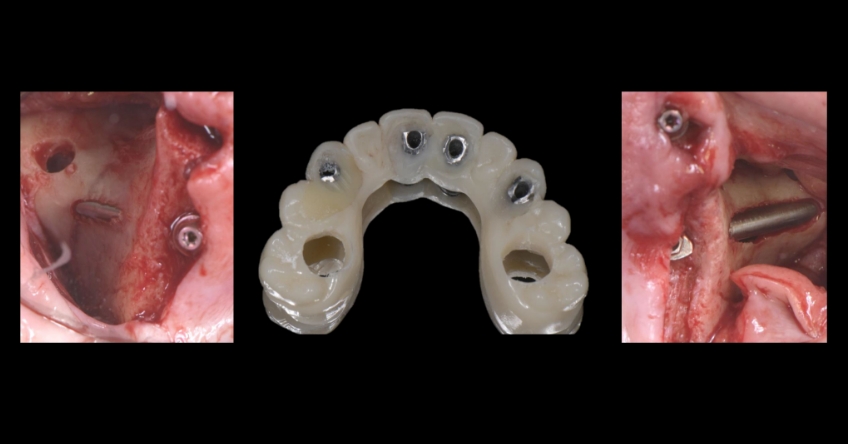
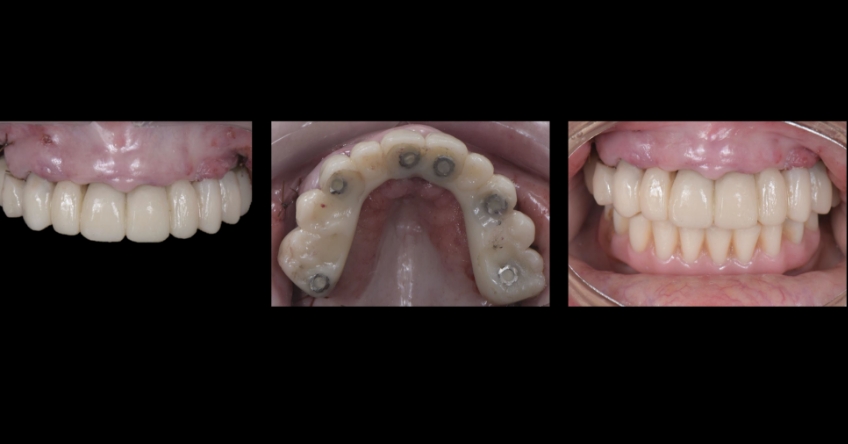
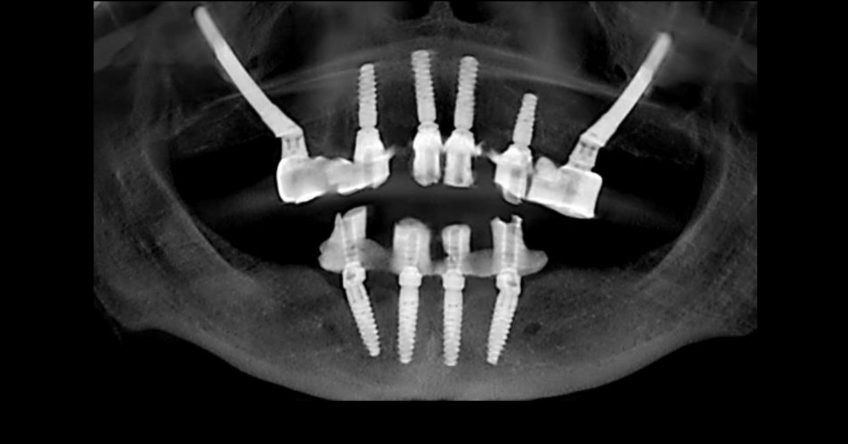
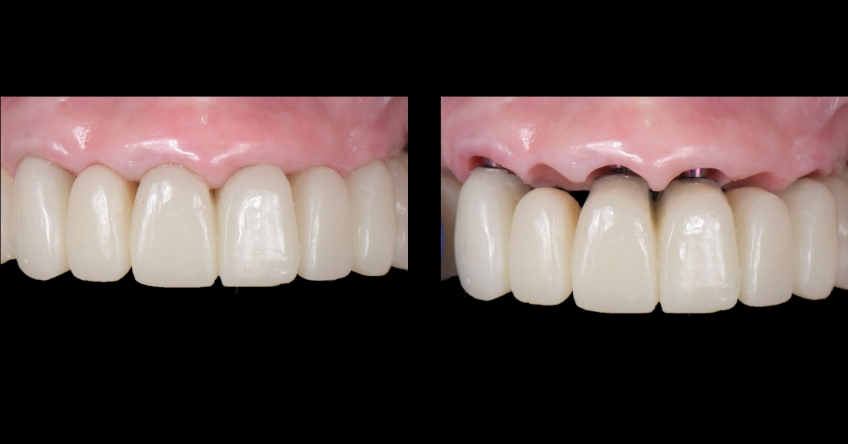
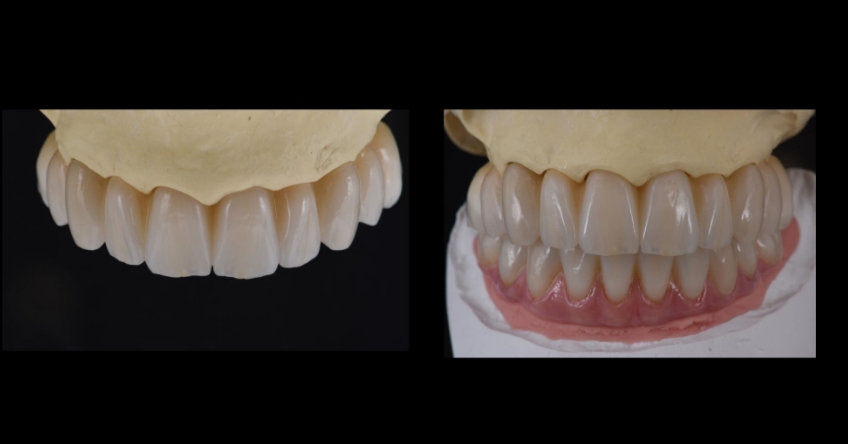
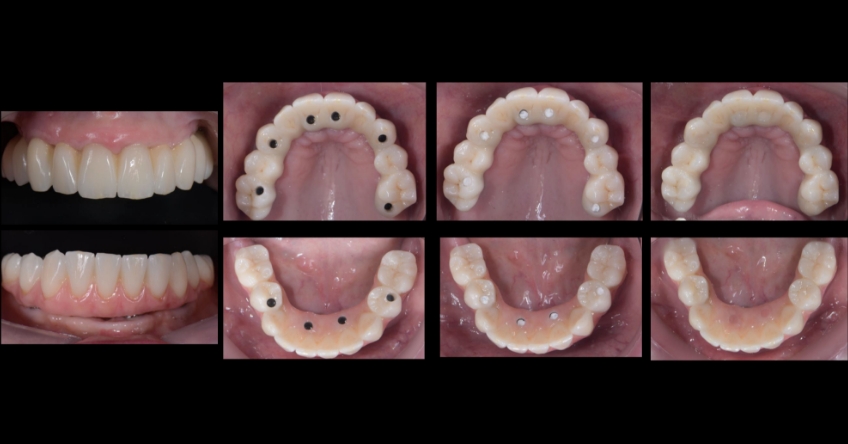
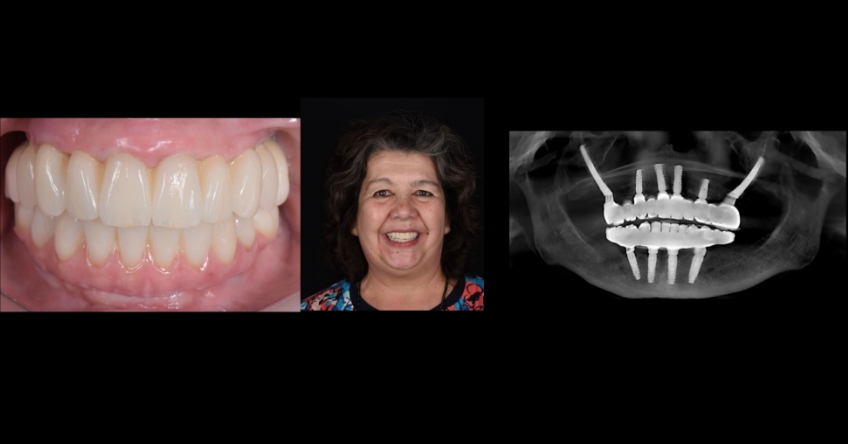
Case study analysis and conclusion
Ultimately, the patient was treated using a combination of traditional and zygomatic implants, allowing her to transition into the definitive prosthesis uneventfully and in a reasonable time frame. This prosthetic design aimed to improve the distribution of occlusal forces and provide enhanced structural support for the final prosthesis.
ZIs, with or without traditional dental implants, are a safe and predictable first line of treatment compared to more time-consuming and financially burdensome traditional bone grafting approaches.
Comparing zygomatic implants (ZI) vs. bone grating can affect the outcome for your patient. The selection of the proper combination of traditional and ZIs is based on the amount of residual maxillary alveolar bone, the biomechanical requirements of the final dental implant rehabilitation, finances, and surgeon and restorative dentist preferences and experience. The most critical factor for success is the establishment of a prosthetically driven treatment plan between the surgeon and the restorative dentist.
Reference
Bedrossian, E., Sullivan, R. M., Fortin, Y., Malo, P., & Indresano, T. (2008). Fixed-prosthetic implant restoration of the edentulous maxilla: a systematic pretreatment evaluation method. Journal of Oral and Maxillofacial Surgery, 66(1), 112-122.
SPEAR STUDY CLUB
Join a Club and Unite with
Like-Minded Peers
In virtual meetings or in-person, Study Club encourages collaboration on exclusive, real-world cases supported by curriculum from the industry leader in dental CE. Find the club closest to you today!

By: Ricardo Mitrani
Date: October 5, 2023
Featured Digest articles
Insights and advice from Spear Faculty and industry experts