Tongue Tie and Sleep Apnea: The Craniofacial Connection
An anatomically compromised upper airway appears to be one of the significant factors in the “creation” of the patient with apnea. Maxillary hypoplasia, septal deviation, retrognathic maxilla, and/or mandible restrict the ability to breathe without resistance, and continued effortful breathing can lead to apnea over time. Large tonsils and adenoids get most of the blame for creating abnormal growth. Recent studies, however, have identified ankyloglossia (tongue tie) as an explanation for the compromised growth and increased apnea risk. This article summarizes 71 articles’ findings on the link between tongue tie and sleep apnea.
Tongue ties limit tongue movement. The inability to move the tongue correctly impairs oral function: sucking, chewing, swallowing, and speaking. It can also compromise the ability to breastfeed, a principal factor in craniofacial development. In addition, the inability to maintain force in the palate while breathing through the nose appears to alter the growth of the maxilla.
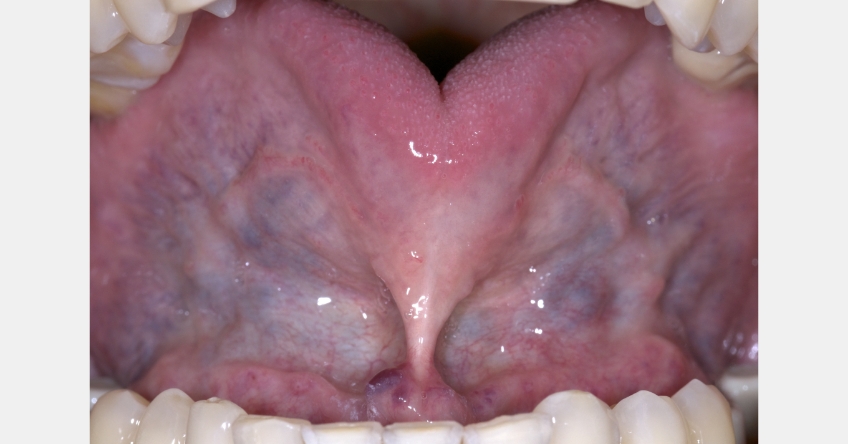
Article Summary: Connection Between Tongue Tie and Sleep Apnea
- Guilleminault et al. examined two groups of children between 3 and 12 years old (n=150): those who were functionally tongue-tied and those with normal attachment. Ankyloglossia was significantly related to higher apnea levels in boys. The conclusion was that a shortened frenulum was associated with apnea as they aged.
- Villa et. al. examined 504 children between the ages of 6 and 14 for tongue ties. They found forty-two children who would subjectively be at risk for apnea. Of that group, 42.8% had a shortened lingual frenulum. Their analysis showed that the risk of apnea in these children was significantly higher than other factors such as obesity, age, gender, and tongue tone.
- A prospective study followed 37 children with short lingual frenulae from 13 months to 12 years after frenectomy. Twenty-four were snorers before the surgery. After surgery, improvement was noted in 16 patients. The study cited improved sleep as well as improvements in speech and swallowing.
- Zaghi’s retrospective cohort followed 110 children aged all over who underwent frenectomy combined with myofunctional therapy. The study found that frenuloplasty paired with myofunctional therapy is safe and effective for treating mouth breathing, snoring, bruxism, and myofascial tension.
Guilleminault’s article noted significant anatomic differences between the tongue-tied and normal groups. They found that the ankyloglossia group had a higher palate and greater maxillary hypoplasia.
This raises some questions: How closely connected are tongue tie and sleep apnea? Would correcting the tongue tie have an impact on preventing the apnea?
If we use long-term follow-up studies on adenotonsillectomy (AT) as an indicator, the answer would be no; it will not help overall. Removal of lymph tissue does have a short-term benefit. However, many of the patients needing AT are craniofacially altered because of their dysfunctional breathing patterns. Those changes eventually cause a return of sleep-disordered breathing. Therefore, Guilleminault’s article stresses that early detection and elimination of the tie for future benefit is essential. If the anatomy has already been damaged, correction is of vital importance.
The Benefits of Myofunctional Therapy
The studies also highlighted the importance of myofunctional therapy to improve the results of the frenectomy. The strategy for the physical therapy currently varies between practitioners.
In my office, we prefer to have appointments before and after the surgery to maximize tongue mobility and reduce discomfort. It is also suggested that, when possible, the therapist be at the surgery to ensure a full release. This may prevent the need for an additional surgery.
Direct and Indirect Factors
The tongue tie is a direct and indirect factor in apnea. The restriction prevents the tongue from rising out of the throat and sitting against the palate, which can be a direct cause of apnea. Indirectly, the inability to position the tongue on the palate alters the growth and development of the oral and nasal cavities.
The underdeveloped anatomy will create more stressful breathing for a lifetime. Because of the maxillary atresia accompanying a tongue tie, I recommend orthopedic intervention (expansion) before releasing a tongue tie on more severe apnea patients. The tie may be the only thing preventing an extreme airway collapse. No studies to date have analyzed this, but it seems prudent.
What began as conjecture is now getting scientific support. Tongue tie and sleep apnea do have a correlation. Tongue ties have an impact on the airway and skeletal development and should be corrected as soon as they are detected. When the tie is missed at birth, the treatment will routinely be interdisciplinary: orthopedic expansion and myofunctional therapy.
References
- Bussi, M. T., de Castro Corrêa, C., Cassettari, A. J., Giacomin, L. T., Faria, A. C., Moreira, A. P. S. M., … & Júnior, A. J. M. (2022). Is ankyloglossia associated with obstructive sleep apnea?. Brazilian Journal of Otorhinolaryngology, 88, S156-S162.
- Guilleminault, C., Huseni, S., & Lo, L. (2016). A frequent phenotype for paediatric sleep apnoea: short lingual frenulum. ERJ Open Research, 2(3).
- Villa, M. P., Evangelisti, M., Barreto, M., Cecili, M., & Kaditis, A. (2020). Short lingual frenulum as a risk factor for sleep-disordered breathing in school-age children. Sleep Medicine, 66, 119-122.
- Baxter, R., Merkel-Walsh, R., Baxter, B. S., Lashley, A., & Rendell, N. R. (2020). Functional improvements of speech, feeding, and sleep after lingual frenectomy tongue-tie release: a prospective cohort study. Clinical Pediatrics, 59(9-10), 885-892.
- Zaghi, S., Valcu‐Pinkerton, S., Jabara, M., Norouz‐Knutsen, L., Govardhan, C., Moeller, J., … & Liu, S. Y. C. (2019). Lingual frenuloplasty with myofunctional therapy: Exploring safety and efficacy in 348 cases. Laryngoscope Investigative Otolaryngology, 4(5), 489-496.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Jeffrey Rouse
Date: December 6, 2022
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


