Dentistry and the Three Common Causes of Compromised Craniofacial Anatomy
A compromised craniofacial anatomy can affect a dentist’s ability to treatment-plan, but it doesn’t have to. When finding ENT support for adenotonsillectomy (AT) can pose a hurdle, it is no wonder dentists become disheartened when their referrals go without action.
Future Spear Digest articles will focus on strategies to find the correct ENT office and building a relationship. In this article, I’ll outline my thoughts about what to do if you can’t get AT performed. It can be frustrating, but it should never stop you from moving forward with treatment of some kind. Just do dentistry.
This challenge has remained unchanged since I began speaking about airway issues in children. The difference today is that AT is not only being recognized for the role it plays in reducing apnea (OSA) and sleep-disturbed breathing events, but also for its use as a treatment for ADHD/anxiety, systemic disease, and altered craniofacial growth.
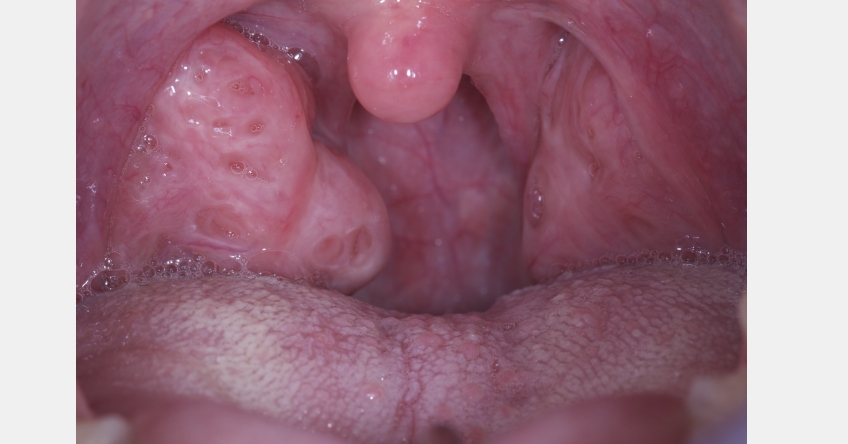
Phenotyping the typical apnea patient starts with recognizing it as an anatomic problem. Over time, the nightly stress of apnea makes the patient more neurologically damaged and their ability to adapt to the airway challenges lessens. Interestingly, the routine solutions for apnea are CPAP or advancement appliances, neither of which fixes the anatomy; they try to overwhelm the problem with air pressure or mandibular protrusion.
Let’s look at the three most common causes of compromised craniofacial anatomy and patient care.
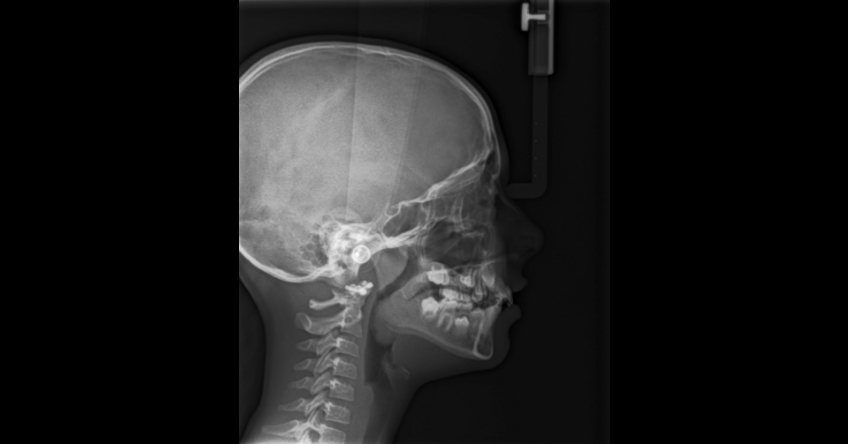
Genetics
If the issue is genetic, my recommendation is to immediately begin dentistry to redirect the growth to a more positive pattern. The problem I’ve run into is the belief in the orthodontic community that you can wait and treat during a growth spurt and you’ll the same result as treating early. While I find significant flaws in the historical literature supporting that view, I won’t argue the point here. The important thing to understand is that orthodontics in these patients is no longer about smiles and function.
The advantage to early intervention is improving brain and body health. The contemporary literature is replete with studies showing that children suffer when we choose to not intervene. Most don’t grow out of these problems; they tend to grow into them. Dentistry must move beyond the mechanical nature of our profession and recognize the powerful tools we must use to change lives by improving breathing and sleep.
Breathing against resistance caused by large lymphoid tissues
If the child is breathing against the resistance offered by the tonsils and adenoids, they will grow abnormally, whether a little or a lot. Therefore, any child receiving AT should have orthodontic treatment to help normalize their growth. If you can’t get the tissue removed surgically, the child’s abnormal growth pattern will continue until breathing is normalized (nasal breathing).
An interesting article published this year (linked here and in References) looks at the impact maxillary expansion has on the size of tonsil and adenoids in children. A one-year follow-up after expansion demonstrated a significant reduction of adenoid and tonsil size, compared with control patients not undergoing expansion. This impact was seen in more than 90% of patients. The authors suggest that improvement in nasal volume and resistance lead to more nasal breathing, which in turn reduces the bacterial challenge.
Tethered oral tissues
Ankyloglossia (tongue-tie) is also a risk factor for altered oral anatomy, including a narrower maxilla and long soft palate. Both changes increase the patient’s risk of having or developing apnea. Screening and treatment are critical, because studies are now concluding that a short lingual frenulum left untreated at birth is associated with OSA later in life. Finally, after the release, myofunctional therapy is necessary to improve the tongue’s rest position and pressure, swallowing pattern, and lip closure for nasal breathing.
If your pediatric patient has the hallmark signs and symptoms of sleep-disordered breathing paired with large tonsils and adenoids, and surgery is not an option (whether because of parental or surgeon resistance or confounding anatomy), focus on normalizing the anatomy and function. Orthopedic expansion and protraction, tongue release, and physical therapy for the tongue are all essential. Remember, myofunctional therapy is not releasing a tie; it is ensuring proper tongue position, swallowing pattern, and nasal breathing.
Ankyloglossia prevents these patients from achieving their goals. What is the proper order? Currently, I recommend orthopedic treatment before myofunctional therapy and tongue release. My logic is that we want to maximize the space available for the tongue before removing the tie. It improves the results of the myofunctional therapy and minimizes the risk that a child with apnea will get worse after the release because the tongue now can relax further down the airway. I have also experienced having a patient relapse from the benefits of therapy after the expansion when they did the myofunctional first.
Compromised craniofacial anatomy and dentistry
Clinicians who treat children with airway issues typically become very enthusiastic about their mission, and it can be disheartening when we don’t receive the support from our medical colleagues. The key in compromised craniofacial anatomy is not to give up but rather “just do dentistry.” Orthopedic and orthodontic improvement of anatomy for health is within our purview. Then, once the skeletal and dentoalveolar anatomy is better, work to make the patient a nasal breather through myofunctional therapy. The impact that dentistry like this can have on children’s lives is immeasurable.
References
- Jang, SJ, Cha, BK, Ngan P, Choi DS, Lee SK, Jang I. (2011). Relationship between the lingual frenulum and craniofacial morphology in adults. American Journal of Orthodontics and Dentofacial Orthopedics, 139(4), e361–e367.
- Yoon A, Abdelwahab M, Bockow R, Vakili A, Lovell K, Chang I, et al. (2022). Impact of rapid palatal expansion on the size of adenoids and tonsils in children. Sleep Medicine, 92, 96–102.
- Villa MP, Evangelisti M, Barreto M, Cecili M, Kaditis A. (2020). Short lingual frenulum as a risk factor for sleep-disordered breathing in school-age children. Sleep Medicine, 66, 119–122.
VIRTUAL SEMINARS
The Campus CE Experience
– Online, Anywhere
Spear Virtual Seminars give you versatility to refine your clinical skills following the same lessons that you would at the Spear Campus in Scottsdale — but from anywhere, as a safe online alternative to large-attendance campus events. Ask an advisor how your practice can take advantage of this new CE option.

By: Jeffrey Rouse
Date: November 10, 2022
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


