Predictably Managing Deep Carious Lesions
Sometimes the decision of how to effectively manage deep carious lesions can seem overwhelming. Should we try to avoid a pulpal exposure, or immediately pursue endodontic treatment? Is this tooth restorable? What type of restoration is most appropriate?
When managing deep carious lesions, it helps to start with the diagnosis, select a caries excavation technique, and determine the choice of restoration.
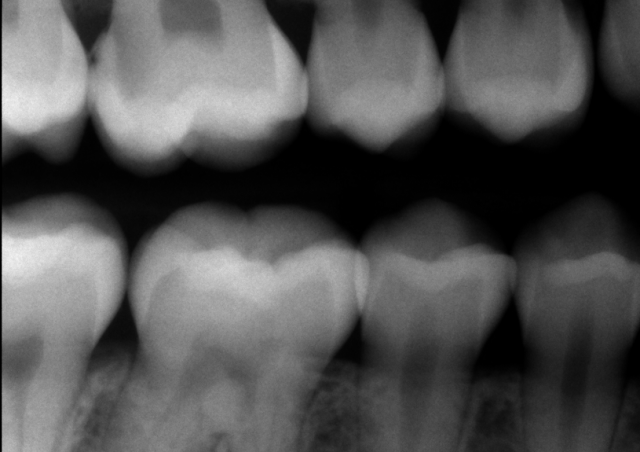
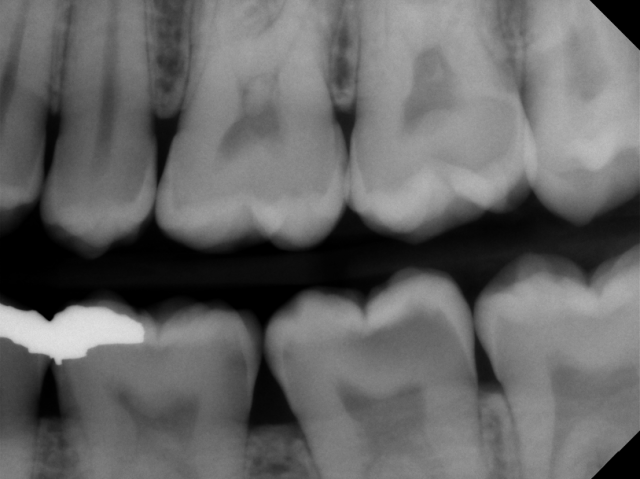
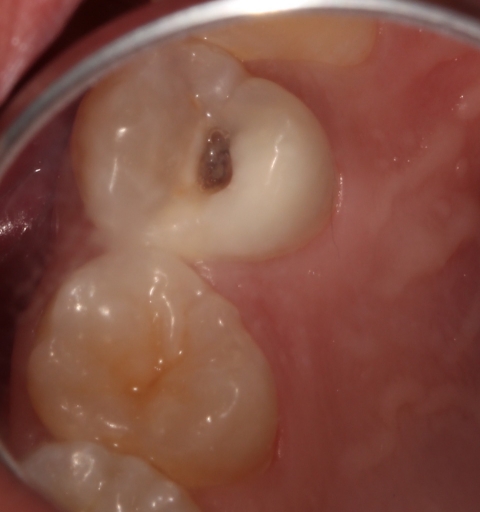
Pulpal and periapical diagnosis for deep carious lesions
The first step in managing deep carious lesions is to determine the pulpal and periapical diagnosis of the tooth in question by performing pulp vitality testing. Pulpal diagnosis can be determined using a variety of tests, including “Endo Ice” cold testing, electronic pulp testing, and heat testing. Periapical diagnosis is achieved by determining if the tooth is symptomatic to percussion or palpation or if a periapical radiograph shows asymptomatic periapical pathology.
In the event a tooth presents with irreversible pulpitis, pulpal necrosis, or periapical pathology, endodontic treatment must be pursued. However, if the tooth is asymptomatic, caries excavation and restoration can be considered.
Caries excavation
If a tooth with a deep carious lesion presents with a normal pulp and periapical tissue, there are various ways to excavate the decay.
- Single visit caries removal. This is the most common method of removing deep carious lesions. This is most effective when the risk of a pulpal exposure is minimal.
- Stepwise caries removal. In cases where pulpal exposure may result from a single-step caries excavation, a “stepwise” approach can be attempted. In the stepwise approach, most of the affected dentin is removed but some affected dentin close to the pulp is left. A provisional restoration, typically in glass ionomer or RMGI, is placed and a second appointment is scheduled to remove the provisional restoration and remaining affected dentin. When a stepwise approach is taken, the isolation of the carious lesion from the oral cavity changes the composition of the bacteria in the carious lesion, making pulpal exposure less likely during the second excavation appointment.
- Indirect pulp cap. Similar to a single-visit caries removal, the indirect pulp cap involves removing the carious lesion and placing a material that protects the pulp and helps promote secondary dentin formation. This can be considered when pulpal blushing is evident after caries excavation, and is especially useful for young immature teeth with an open apex.
- Direct pulp cap. In the event of a pulp exposure, the exposed pulp is covered with a medicament or restorative material that helps with the formation of a dentinal bridge. Direct pulp capping has been a controversial treatment, with many variables affecting the success rates. Generally, direct pulp capping is more successful if pulpal exposure is due to a mechanical exposure rather than a carious exposure.
In future articles, we’ll expand on these caries removal procedures to discuss when each is most appropriate.
Choice of restoration for teeth with deep carious lesions
There are many choices for restoring teeth with deep carious lesions. The three most common options are protective restorations, direct restorations, and indirect restorations.
Protective restorations are temporary restorations that are intended to be replaced at a later date. These are more commonly used when the pulpal prognosis of the tooth is questionable after caries excavation. Glass ionomer and RMGI materials are frequently used for protective restorations.
Direct restorations and indirect restorations can also be used to restore teeth with deep carious lesions. It’s imperative that there are no signs of irreversible pulpitis or pulpal necrosis when a definitive restoration is to be placed on a tooth with deep caries.
In summary, the daunting task of restoring a deep carious lesion can be simplified by determining the diagnosis, excavation technique, and restoration before working on the tooth. These three key factors help make the process of managing deep carious lesions a more predictable procedure.
FOUNDATIONS MEMBERSHIP
New Dentist?
This Program Is Just for You.
Spear’s Foundations membership is specifically for dentists in their first five years of practice. For less than you charge for one crown, get a full year of training that applies to your daily work, including guidance from trusted faculty and support from a community of peers.

By: Andy Janiga
Date: May 20, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


