Connecting Teeth and Implants: Yes, No, Maybe?
Whether it’s acceptable to connect an implant to a tooth (or teeth) in a restoration is one of the most misunderstood areas of implant dentistry. The reason so much confusion exists is simple: There isn’t one correct answer.
To understand why, you must look at the mechanics of connecting an implant and a tooth, recognizing that the implant is essentially ankylosed with effectively no mobility, while the tooth has a PDL and may have minimal to significant levels of mobility (Fig. 1).

Under occlusal loading, the implant, being less mobile, will always be at greater risk of receiving increased load. The tooth will never be at risk of being overloaded, because it is more mobile and would move under the load, unlike the implant.
Connecting a single implant to a single tooth with significant mobility has the potential for the tooth to act as a cantilevered pontic extended from the implant. If one or more pontics are between the implant and mobile tooth, there is a longer lever arm and the load on the implant will be increased accordingly.
If the tooth has no mobility, the risk of significantly increasing the load on the implant is very low, even in the case of a fixed partial denture where there may be pontics between the implant and tooth.
There are other variables besides mobility to consider when contemplating connecting implants to teeth. Two significant considerations are the level of parafunctional activity of the patient and the number of implants and teeth being used in the restoration.
A patient with minimal to no parafunction and teeth with normal mobility presents minimal risk when being connected to an implant. This risk is reduced when more than one implant is involved in the restoration. Much of what we know today about connecting implants and teeth was learned in the 1980s, when we were in the infancy of working with osseointegrated implants in the U.S.
Example 1
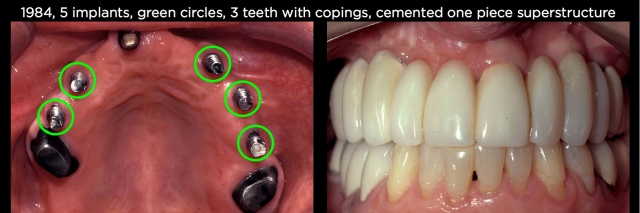
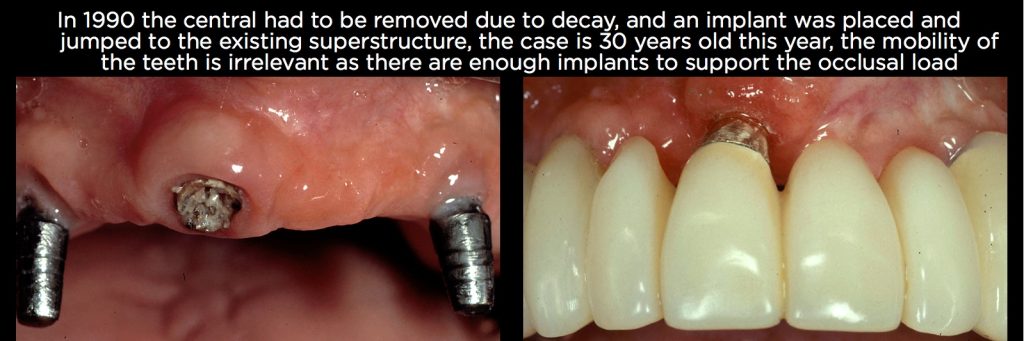
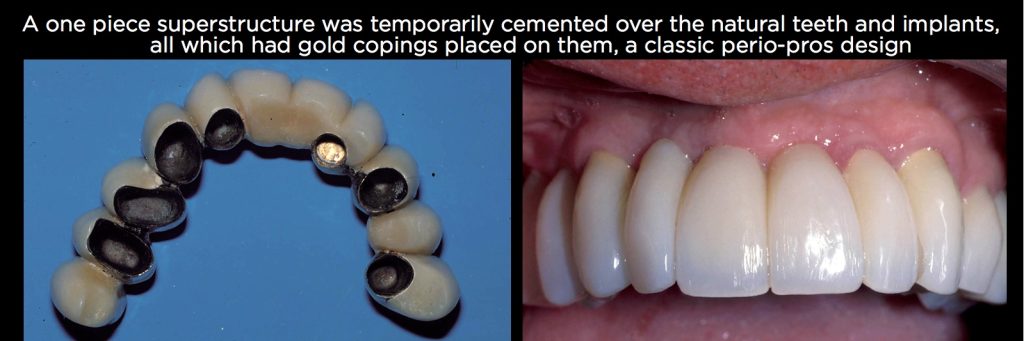
The patient shown in Figs. 2 and 3 above presented in 1984 with a maxillary central incisor that had endo, a post core and one remaining molar on each side. Back then, we rarely would have considered removing the natural teeth, so they were restored with permanently cemented gold copings. In addition, five implants were placed; three on one side and two on the other. Enough implants were placed to support the occlusion of the entire arch — in other words, the teeth were unnecessary. A one-piece superstructure was placed with temporary cement over all the teeth and implants.
The restoration is still successfully functioning 30 years after treatment. This approach has been referenced in the literature for decades and is generally quite successful, assuming an adequate number of implants to provide occlusal support is used or the teeth aren’t mobile.1,2
In contrast, a patient with high levels of parafunction and multiple mobile teeth is at high risk for overloading the implant if the implant is rigidly connected to mobile teeth. This usually isn’t producing a loss of integration but instead a structural problem; loose or fractured abutment screws would be an example. The risk is extremely high if an inadequate number of implants is used in the restoration.
Example 2
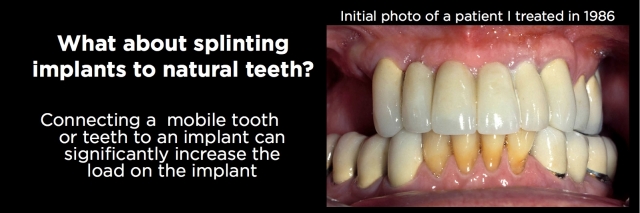
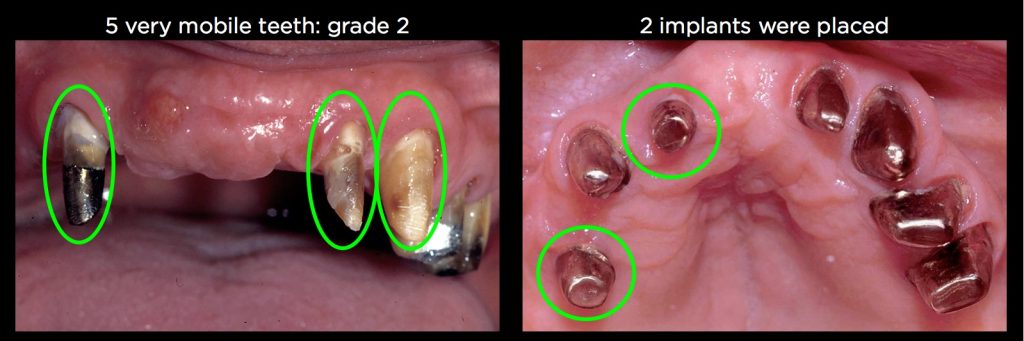
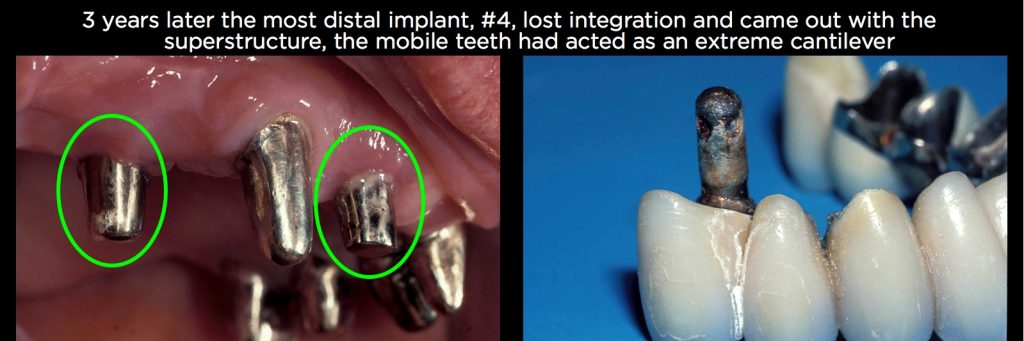
The patient shown in Figs. 4–7, for example, was referred to me in 1986 after fracturing porcelain and solder joints on his fourth reconstruction in only 10 years. (He has a history of severe bruxism.) After removing the old reconstruction, I was left with a maxillary right canine that had endo and a post core, and on the left side a lateral, a canine, and both premolars. All five remaining teeth had a Grade II mobility.
As mentioned earlier, in the mid-1980s we rarely would have considered sacrificing a natural tooth to place an implant. So the surgeon placed two implants, one in the right lateral position and one in the right second premolar position. I then placed gold copings on all the natural teeth and the two implants. In addition, a one-piece superstructure was temporarily cemented over the teeth and implants.
The problem is that the one-piece restoration is effectively cantilevered off the two implants due to the Grade II mobility of the natural teeth. It took three years, but ultimately the patient lost the integration of the second premolar implant, which came out when I went to remove the temporarily cemented superstructure.
I then put the lateral incisor implant to sleep and used composite to turn the lateral and second premolar, where the implants had been, into pontics. When all the teeth are equally mobile and you use a one-piece restoration, it’s interesting to see how well they do: The patient went seven years before the right canine root finally fractured. We then removed all the teeth and went to a completely implant-supported restoration, using eight implants to support his high levels of muscle activity.
Having focused on the risk for the implant when connecting them to a natural tooth, there is one concern for the natural teeth: intrusion, the tooth moving apically out from under the prosthesis.
This is an issue that has occurred for decades — not just with teeth and implants. In the old days of periodontal prosthesis, where each tooth received a gold coping that was permanently cemented with a full-arch restoration temporarily cemented over the top, it was not unusual to see an isolated tooth or teeth intrude out from under the prosthesis, sometimes by as much as 1–1.5 mm (Fig. 8).

Example 3
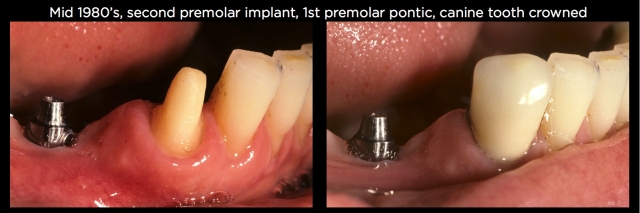
Intrusion has been shown to occur when the tooth is connected to the implant with a nonrigid connection that allows the tooth to move independently of the implant in an inferior direction. An example is the classic implant restorations from the mid- to late 1980s.3–7
Most of the implant companies back then didn’t have any type of antirotational implant abutments, so it was necessary to connect the single-tooth implant restorations to the adjacent tooth with a nonrigid connection so the implant restoration didn’t rotate and come loose. In addition, because of how weak the screw was connecting the restoration to the abutment, it was necessary to place the female portion of the nonrigid attachment on the natural tooth and the male on the implant. This allowed for removal and retrieval of broken or loose screws after the restorations were placed, but it also created a situation where the natural tooth could intrude relative to the implant, and on occasion they did (Figs. 9 and 10).
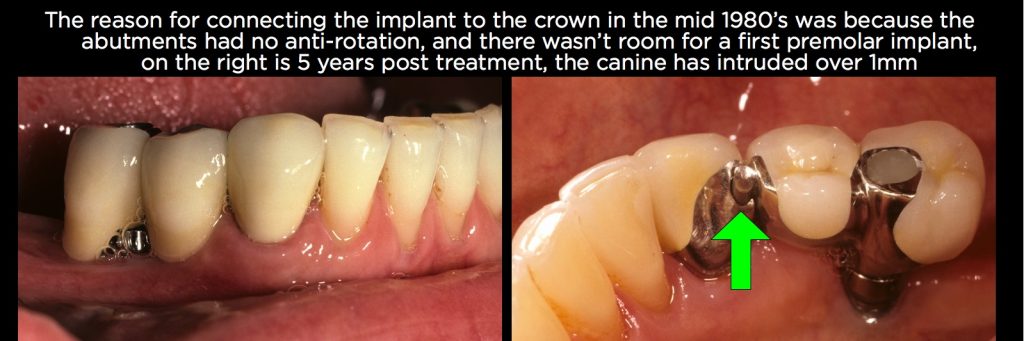
The classic coping and one-piece superstructure design used in the 1980s and 1990s (Figs. 2–7) is also susceptible to natural tooth intrusion. If the temporary cement washes out between a coping and the superstructure, it allows the natural tooth to move independently of the restoration, and intrusion was a possibility. Several theories have been postulated as to why intrusion occurs.8–10
With the risks of overloading of the implant, and intrusion of the teeth, it would seem reasonable to ask why you’d want to connect an implant and a tooth, but there are times where it may be necessary — and sometimes even desirable.
The most common reason would be because you have to. An example might be a patient missing a lower first and second molar. A surgeon places two implants, one for each missing molar, but what if the first molar implant doesn’t integrate? A new implant is placed for the first molar, but it also doesn’t integrate. The patient says no more, they want the restorations. Your only choice would be to connect the second-molar implant to the second premolar and do a three-unit FPD.
Example 4
An additional reason for choosing to connect implants and natural teeth is a situation where it simply isn’t possible to surgically place all the implants you’d like, so you need to connect the available implants to a tooth or teeth and use an FPD.
If it’s necessary to connect implants and teeth, the question becomes what the design of the restoration looks like. Ideally, the design accomplishes two things: prevent the tooth from intruding, and provide some stress relief for the implant if the tooth being connected is mobile. The stress relief primarily applies when connecting a mobile tooth to a single implant.
The other consideration when connecting an implant and a tooth is whether you’d like the implant restoration to be retrievable, so you can get the restoration off and deal with issues like loose or fractured abutment screws.
Design options
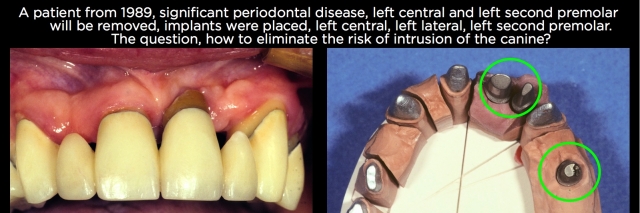
I’ll use the patient shown in Fig. 11 to illustrate some design options. She presented in 1989 with significant periodontal disease and an FPD from the left central to left canine to left second premolar. The left lateral and left first premolar were pontics. The decision was made to remove the left central and left second premolar because of the severity of the periodontal defects.
The surgeon placed three implants, one in the left central and lateral and one for the second premolar; the canine was acceptable periodontally and was retained. We will have to connect the implants to the canine to create an FPD. The first thing I would recognize is that the three implants are more than adequate to support the occlusion, so the canine isn’t necessary for the restoration to be successful, but it is present and the patient doesn’t want it removed.
My concern in planning the design of her restoration was primarily focused around two areas: preventing intrusion of the canine out from under the restoration, and providing the ability to remove the implant restoration to access the abutment screws. These were UCLA abutments, and in this era we didn’t even have torque drivers or gold screws yet, so screw loosening was a very real issue that had to be planned for.
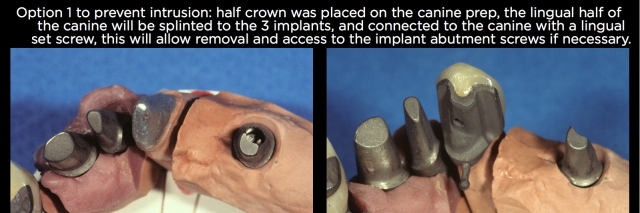
My solution can be seen in Figs. 12 and 13. I had the technician make the crown on the canine with a lingual that was cast separately, and had a small screw to retain it to the actual cemented crown. The crown was permanently cemented to the canine tooth, but the removable lingual was soldered to the implant restorations. The five-unit restoration was temporarily cemented and the lingual set screw placed to prevent intrusion of the canine.
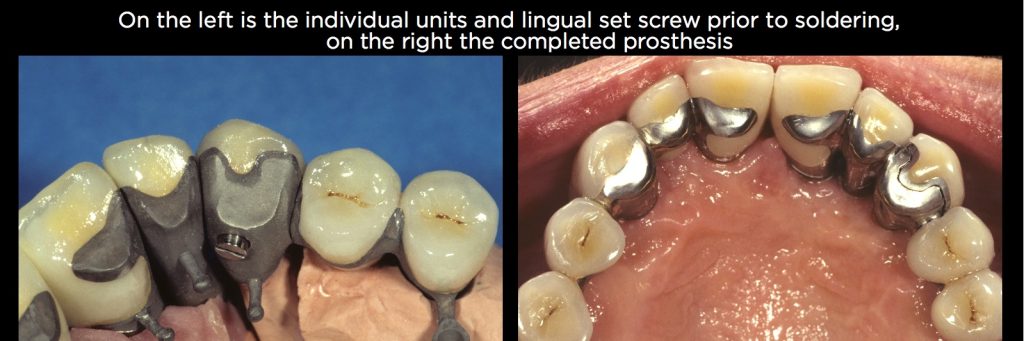
I could have left the central and laterals as single-unit restorations and just done a three-unit FPD from the canine to the second premolar implant. Instead, I connected the central and lateral, creating the five-unit splint, which had the advantage of eliminating any risk of implant overload due to the fact the canine had Grade I mobility. A relatively complex design, but it has worked for more than 25 years.
If I would have treated the same patient today with a retained canine and second premolar implant, I would have designed it as shown in Fig. 14. The biggest difference is today, I would have used a modern internal connection implant, such as a Straumann, which would have eliminated my concerns about screw loosening and needing the retrievability of removing the implant restoration to gain access to the abutment screw.
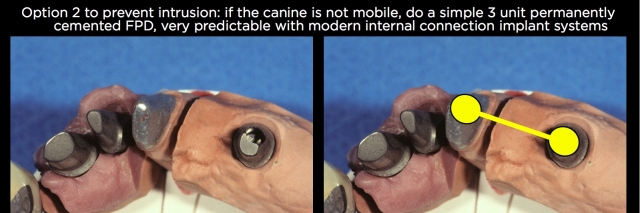
Without the need to have the implant restoration retrievable, I would have considered two design options based upon the mobility of the canine. If the canine had virtually no mobility, or what I would consider normal mobility, I would have torqued the abutment to place on the implant, then done a simple three-unit FPD, permanently cementing the restoration to the implant abutment and the canine. The permanent cementation eliminates the risk of the canine intruding.
If the canine had slight mobility, I would have connected the canine to the second premolar implant using a nonrigid connector, but the key is how you orient the connector to prevent intrusion of the canine. The traditional approach as seen in Fig. 10, where the female attachment is on the natural tooth, won’t prevent intrusion; instead the female needs to be placed on the mesial of the second premolar implant crown, which will be permanently cemented to the implant abutment. Then the male is attached to the distal of the first premolar pontic, which is attached to the canine. This approach will not allow the canine to intrude as long as the canine restoration is permanently cemented (Fig. 15).

The key when using a nonrigid connection to attach the slightly mobile canine to the implant is to be sure the attachment isn’t too rigid, as many precision attachments are. Before cementing the canine restoration I would try it in and see if you can mimic the mobility seen in the canine as a single tooth. If you can’t, I would rubber-wheel the male attachment to provide a greater amount of freedom in its fit into the female attachment.
Chee and Mordohai published a unique case in 2010, where rather than an attachment, they simply created a deep rest seat on the implant crown, similar to what would be done on a removable partial denture; the male portion of the rest was attached to the pontic, which was attached to the natural tooth.11
The biggest risk
The highest risk implant to tooth connection would be if the implant was to be used as a pier abutment, with a pontic and natural tooth on each side of it. I don’t have any clinical examples where I have used an implant as a pier abutment between natural teeth, but I have been asked about it several times by different clinicians. I am including a case of using natural teeth as pier abutments to illustrate the challenge.
The patient in this case is missing laterals and first and second premolars with the canines in the first premolar position. She was treated in 1985, before we had UCLA abutments, and was treated without implants. Today it would have been a very clean implant case and much less complex. The biggest challenge of pier abutments is they act as a fulcrum in the middle of the prosthesis, so when the patient bites on either end, there is a tension applied at the opposite end, which wants to unseat the restoration (Fig. 16).

The solution is to use attachments as stress-breakers. The typical location is what is seen in this patient — the distal of the pier abutment. In her case, the restoration is rigidly splinted from first premolar to the centrals and the opposite first premolar, and there are then female attachments on the distal of the first premolar pier abutments. The male is attached to the mesial of the second premolar pontics (Figs. 17–19).

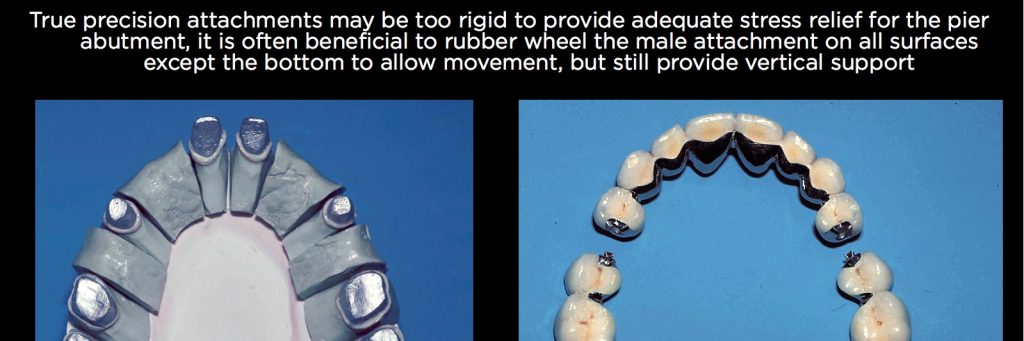
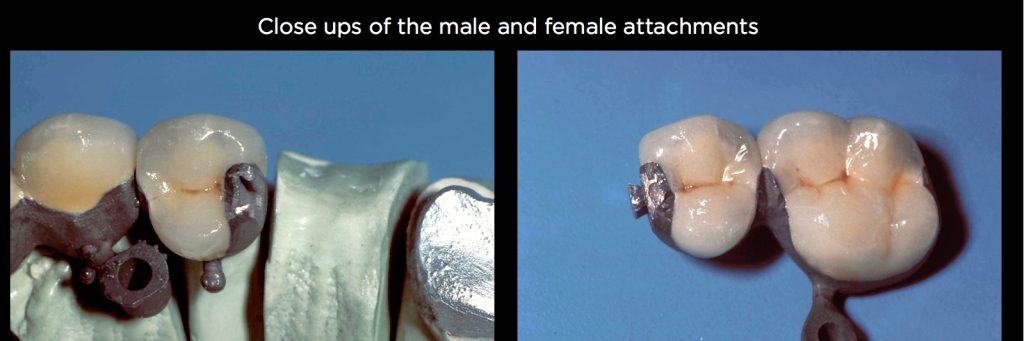
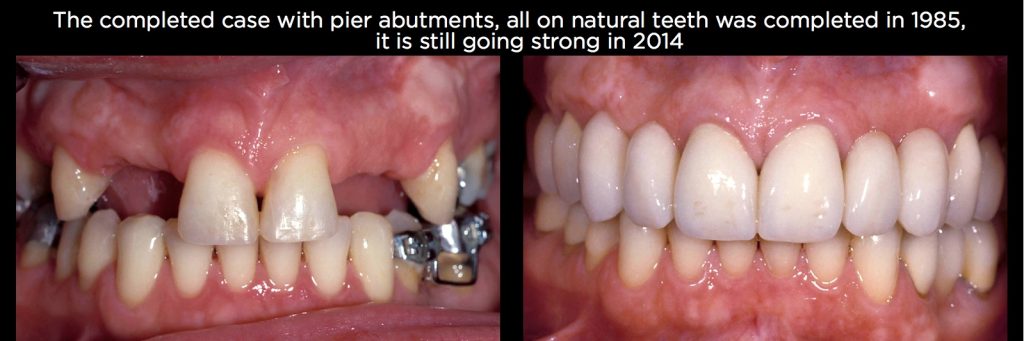
If the pier abutment was an implant, I might have also considered placing an attachment on the mesial of the pier abutment, dependent upon the mobility of the anterior teeth. The restoration seen on the patient in Fig. 20 is still functioning fine 29 years after placement.
Connecting to maintain mobile natural teeth
The final reason I have connected implants and natural teeth is to maintain mobile natural teeth in the anterior, which subsequently retains bone and soft tissue, specifically the papillae. Of course, the key is to use enough implants that the mobile tooth or teeth don’t risk overloading the implants and to permanently cement the restorations to prevent intrusion of the natural teeth.
The patient shown in Figs. 21–25 is an example. She is 63 years old, and has significant apical root resorption on the centrals and laterals. Interestingly enough, she did well with them for almost 50 years after orthodontic treatment as a child, but now the laterals have a Grade II+ mobility, and the centrals a Grade I+. Her chief complaint is that she can’t use her incisors to function.
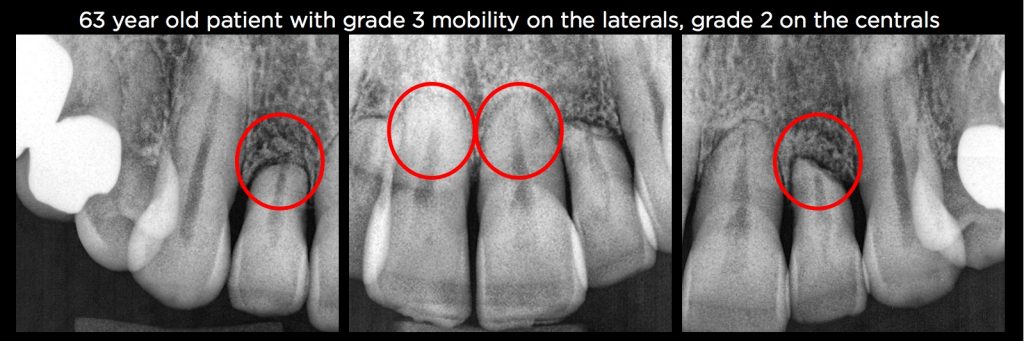
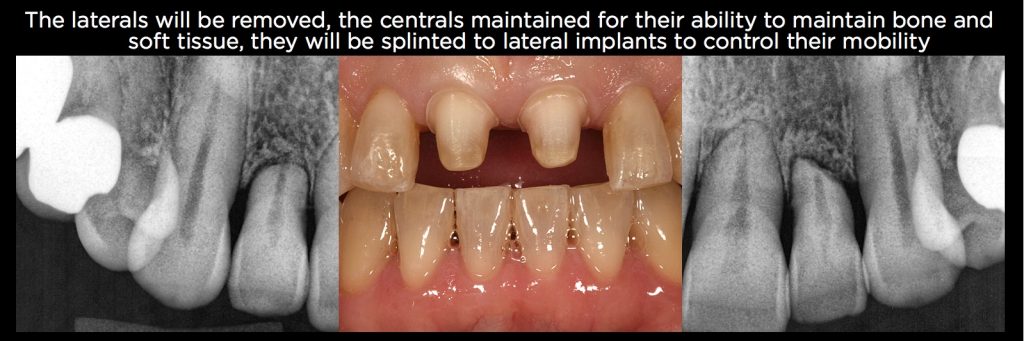
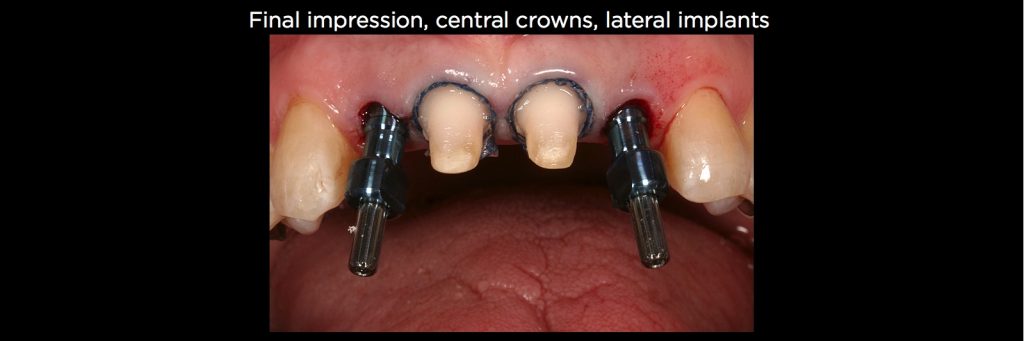

The original plan was to consider removing all four incisors and placing two implants either in the central location or lateral location, then do a four-unit FPD. But in reality, the centrals are quite healthy except for the mobility, so the decision was made to remove the laterals, place implants, then prepare the centrals for crowns and splint them rigidly to the lateral implants.
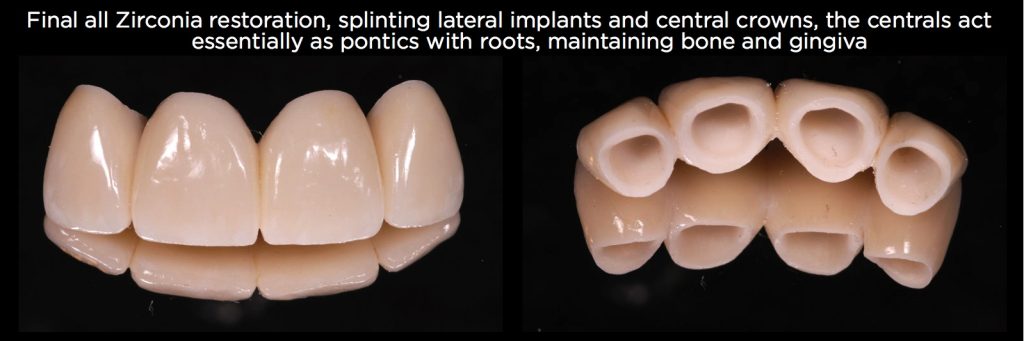
There’s no risk of overloading the implants because the two implants don’t need the central support, and there’s also no risk of the central intruding because they’re rigidly connected to the implants and permanently cemented to the central preps.
While the original plan would have been successful, this approach maintains the gingiva and papillae across the anterior.
In conclusion, it would be safe to say that the most predictable and least risky restoration would leave the teeth and implants freestanding, but experience and the literature make it clear that implants can be safely connected to natural teeth as long as consideration is given to the challenges of implant overload and preventing intrusion of the natural teeth.12–14
References
- Hosny M, Duyck J, van Steenberghe D, Naert I. Within-subject comparison between connected and nonconnected tooth-to-implant fixed partial prostheses: up to 14-year follow-up study. Int J Prosthodont. 2000 Jul-Aug; 13(4):340-6.
- Biomed Tech (Berl). 2012 Feb;57(1):39-43. doi: 10.1515/bmt-2011-0033. Retrievable, tooth-implant-supported, complete-arch fixed restorations in the maxilla: a 6-year retrospective study. Mundt T, Heinemann F, Schwahn C, Biffar R.
- Reider C E. Copings on tooth and implant abutments for superstructure prostheses. Int J Periodont Rest Dent 1990; 6: 437-453.
- Garcia L T, Oesterle L J. Natural tooth intrusion phenomenon with implants: A survey. Int J Oral Maxillofac Implants 1998; 13: 227-231.
- Schlumberger T L, Bowley J F, Maze G I. Intrusion phenomenon in combination tooth-implant restorations: A review of the literature. J Prosthet Dent 1998; 80: 199-203.
- Pesun I J. Intrusion of teeth in the combination implant-to natural-tooth fixed partial denture: a review of the theories. J Prosthodont 1997; 6: 268-277.
- Chee W W, Cho G C. A rationale for not connecting implants to natural teeth. J Prosthodont 1997; 6: 7-10.
- Cho G C, Chee W W. Apparent intrusion of natural teeth under an implant-supported prosthesis: a clinical report. J Prosthet Dent 1992; 68: 3-5.
- Cohn S A. Disuse atrophy of the periodontium in mice. Arch Oral Biol 1965; 10: 909-919.
- Cohn S A. Disuse atrophy of the periodontium in mice following partial loss of function. Arch Oral Biol 1966; 11: 95-102.
- Sheets C G, Earthman J C. Natural tooth intrusion and reversal in implant assisted prosthesis: evidence and a hypothesis for the occurrence. J Prosthet Dent 1993; 70: 513-520.
- Clin Implant Dent Relat Res. 2010 Jun 1;12(2):122-33. Tooth-to-implant connection: a systematic review of the literature and a case report utilizing a new connection design. Chee WW1, Mordohai N.
- Naert I E, Duyck J A, Hosny M M, Van Steenberghe D. Freestanding and tooth-implant connected prostheses in the treatment of partially edentulous patients. Part I: An up to 15-years clinical evaluation. Clin Oral Implants Res 2001;12: 237-244.
- Naert I E, Duyck J A, Hosny M M et al. Freestanding and tooth-implant connected prostheses in the treatment of partially edentulous patients Part II: An up to 15-years radiographic evaluation. Clin Oral Implants Res 2001;12: 245-251.
- Block M S, Lirette D, Gardiner D et al. Prospective evaluation of implants connected to teeth. Int J Oral Maxillofac Implants 2002; 17: 473-487.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Frank Spear
Date: May 7, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


