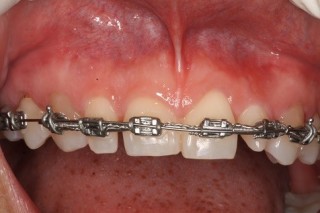
Why Gingivectomies Fail
At one time or another, we all want or need to move gingival tissues. While our patients may need us to do that in order to reach their goals, it is a safe bet that no one ever wants to have it done. It’s similar to surgery – no one really wants surgery (however minor it may be) if they can get results in another way. As we know, the simplest way to move gingival tissue is to simply cut if off. While this is typically quick and easy, the fact is that sometimes when we do this the tissue comes back. That presents the question: Can we know when we can expect the gum tissue we remove to come back? The answer typically is yes as we know from the literature that gingival levels follow bone levels, therefore, if we remove gingiva in an area that is following bone we can expect it to come back. Our only shot at a successful gingivectomy is in an area of localized gingival excess compared to the rest of the mouth.
This brings us to the important question: How do we determine the bone levels and when and if do gingivectomies have a shot at being successful? Radiographs are of course the first thing for us to use when gathering our information. The important thing for us to remember when using radiographs for this purpose is that they must not be overly angled. Instead, they should be taken with sensor or film as parallel to the tooth as possible and with the x-ray beam as perpendicular to the film or sensor as possible so that we can get the most accurate representation of the bone levels.
The next thing we can do is use bone sounding to physically determine the bone levels.To do this simply anesthetize the patient in the area to be measured and then use firm pressure to probe the bone using a periodontal probe. The key is that you need to be sure the tip of your probe stays close to the root and contacts the highest point of the bone. It is worth noting that this can be easier said than done since the bone at the highest level is often thin, making it easy for the probe to land on a thicker area of bone that is more apical to the true height. One big down side to remember when bone sounding is the fact that you only know the bone level of the areas you actually sound which means you are going to have “gaps” in the information you gather since you are obviously not going to probe each and every spot of the bone. While we can extrapolate the probable bone level between the sounding points it is important to remember that we are only estimating these areas.
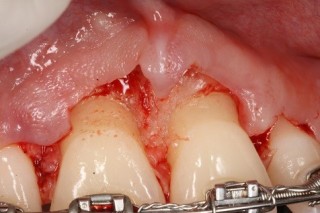
So what’s the only way to know where all the bone is with 100 percent certainty? As I am sure you guessed, it is surgery to visualize the bone. The issues with doing surgery are obvious. First, not every case needs osseous surgery. Second, there are risks, as we know, with any surgery. Third, surgery adds healing time and increases the expense of a case. The upside to doing the surgery when indicated is the fact that often times it is the only way to get the gingival tissue to stay where we want/need it to be. The fact of the matter is not doing the osseous surgery when indicated and only doing a gingivectomy will result in the gingival tissue growing back, which means your patients will then need a second surgery to get the bone and tissue where it is needed/desired. Take for example the case pictured here. The top photo is a pre-operative photo and the second photo shows the bone that was influencing the gingiva. As you can clearly see if only a gingivectomy had been done the gingival tissue would have grown back. Therefore, the only way to get the results the patient desired was to recontour the bone.
John R. Carson, DDS, PC, Spear Visiting Faculty and Contributing Author www.johncarsondds.com
VIRTUAL SEMINARS
Stay Sharp. Stay Current. Stay Ahead.
Join live, focused training designed to help you implement immediately and strengthen your expertise.

By: John Carson
Date: April 2, 2015
Featured Digest articles
Insights and advice from Spear Faculty and industry experts