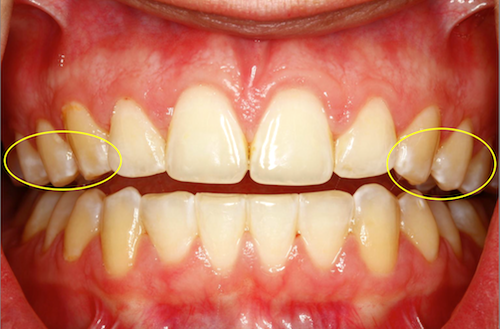
How to Manage White Spot Lesions
White spot lesions (WSL) are common during or after orthodontic treatment. Managing these lesions is a challenge. The following are best practices recommendations based on current research.
Most studies report the incidence of new clinically visible WSL occurring during orthodontic treatment to range between 30 to 70 percent of patients. Upper anterior teeth, especially maxillary laterals, are most commonly affected.
Prevention is key
Remineralization and restorative treatments for WSL are possible; but they either result in less than ideal cosmetic outcomes or they are too aggressive. Therefore, it is better to rely on prevention as the primary management strategy.
1. Identify risk
The following conditions indicate that patients are at high-risk:
- Existing WSL
- Poor oral hygiene and/or diet
- High DMFT
- New lesions that start during treatment
2. Plaque control
Effective motivation techniques tailored to the patient, use of disclosing solution and using an electric toothbrush are helpful in improving plaque control.
3. Fluorides and other adjuncts
- Prescribe 15000ppm Fl toothpaste. Compliance is better than fluoride rinse.
- Application of Fl varnish as frequent as every six-weeks. This is effective in preventing and reversing early demineralization.
- Prophylaxis every three months
- MI Paste: Before going to bed smear over teeth with help of a brush or apply with a fluoride delivery tray.
- Xylitol: Chew on xylitol gum three to four times a day. It increases salivation, which helps in reminerlization, and it causes reduction in the level of S.mutans.
- Chlorhexidine rinse: Once a day rinse for a week, repeated every month. It helps reduce the level of caries producing and pH reducing bacteria in the mouth.
4. New methods
The following emerging adjunctive therapies have shown promising results (more independent research is needed):
- Probiotics: They help shift the oral microflora balance towards higher pH producing caries free bacteria.
- CariFree: A proprietary product that claims to help restore the pH balance in the oral environment.
- Carbamide peroxide: Applying this has shown to improve the pH of the oral environment. Also an added benefit is whiter teeth, which would get easy acceptance with patients.
- Resin sealants: A proprietary resin material, Pro Seal is applied on the enamel before bonding brackets. Protects it from demineralization effect. For high-risk patients this can be used, especially for upper anterior teeth. It is a bit cumbersome to clean off and polish the teeth after de-bonding though.
References
Vivek Mehta DMD, FAGD, Visiting Faculty, Spear Education. Follow him on Twitter @Mehta_DMD.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Vivek Mehta
Date: January 5, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts