The Mystery of Tooth Preparation
Have you ever done a tooth preparation and then found despite having reduced the prescribed amount of structure, you don’t have the proper amount of clearance for your restoration? If you’ve ever had this happen, you know how puzzling and frustrating it can be.
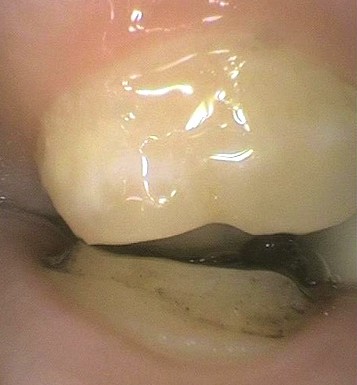
I’m currently treating a patient who came in complaining of TMD symptoms. The indications became progressively worse after some recent crowns she had done in another office. During splint therapy, one of her crowns came off; clearly the tooth had been reduced. The preparation was in contact with the opposing tooth. So what happened?
There are really only two possible causes for this. The first would be that the tooth was simply just not reduced enough. The second cause — which is more difficult and complicated to deal with — is that something changed with the patient’s bite, which in this case appeared to be at least part of the problem.
So what can change in our patient’s bite and cause the loss of occlusal clearance on a prepared tooth? Surprisingly, it’s pretty simple. If we accept, as documented in the literature, that the condyles on most of our patients are not seated, we must ask: What’s keeping them from doing so?
Usually the patient’s teeth are causing this. So what happens if we prepare away the spots keeping the condyles from seating? You guessed it — they seat.
It’s this seating that can cause you to lose the occlusal clearance you thought you made by reducing the tooth.
The simplest way to help manage this risk is to use a leaf gauge to find which teeth touch first when your patient’s condyles are seated. The one I prefer, which you can order from Great Lakes Orthodontics, is simply several thin pieces of plastic fastened together.
Basically, you place it between the central incisors and adjust it so no other teeth are touching when the patient tries to close. Then reduce the thickness of the gauge until you find the first teeth that contact.
In these cases, it’s best to take a step back and understand what you can expect to happen when you prepare these teeth and discuss how you plan to manage it with your patient.
John R. Carson, DDS, PC, Spear Visiting Faculty. [ www.johnrcarsondds.com ]
SPEAR STUDY CLUB
Join a Club and Unite with
Like-Minded Peers
In virtual meetings or in-person, Study Club encourages collaboration on exclusive, real-world cases supported by curriculum from the industry leader in dental CE. Find the club closest to you today!

By: John Carson
Date: January 21, 2013
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


