- Techniques / Materials
10 Steps to Posterior Crown Prep

Crown preparations are a common restorative procedure that we encounter every day. Therefore, they should be quick, predictable, and easy to perform.
In this article, I will do a quick review of a method that has worked for me and offer a step-by-step guide to get your preparations done quickly and efficiently. The guide will also help you ensure your final crown preparation allows you to give your patient an excellent final restoration.
First and foremost, you have to begin with the end in mind, meaning that you have to decide the type of material out of which your crown will be made. Will it be monolithic or layered? Gold, PFM, e.max or zirconia?
Why must you think about this first? Because each material requires different reduction amounts and preparation design, you must decide which will allow you to reach or exceed your patient’s final desired result.
Once you have decided what is best for your patient and their situation, where do you start?
Preparing Posterior Crowns
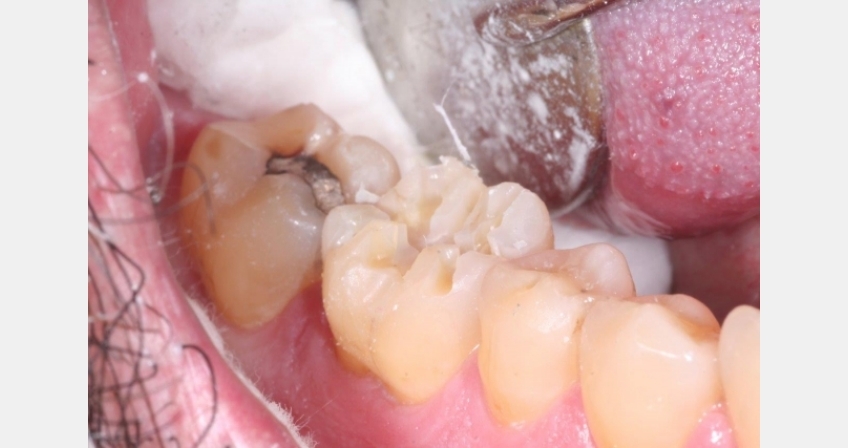
- Remove old restorative material and decay to verify restorability in its current state and need for possible root canal therapy and/or crown lengthening. I also determine if a crown restoration is going to be the most conservative and longest lasting or would the tooth and patient be better served doing an inlay or onlay restoration?
- Isolate the tooth for proper bonding and adhesive protocol to place the build-up material of choice (personally, I like light-cured resin and/or dual-cured resin in areas where light penetration may be challenging. Ensure that your build-up material and bonding agent are compatible. Don’t overbuild the tooth, as this wastes material and can affect the next step’s simplicity.
- Now we are ready for the crown preparation (if a tooth will definitely need a crown, e.g. root canal posterior molar with large filling, then I will start with this step first). First thing first: I start with depth cuts on the occlusal table with a known length bur (there are specific depth-cutting burs as well) that is for the needed reduction of the restoration of choice. I take this bur down the central groove, across the cusps, and out the grooves to depth. Now, there is no confusion of how much to remove.
- I will then place a small-diameter bur (KS0 is my bur of choice) to remove the pieces of tooth sticking up between the depth cuts. I essentially place the bur in the groove and either push or pull, which cuts or “amputates” that segment of the tooth off rather quickly and efficiently.
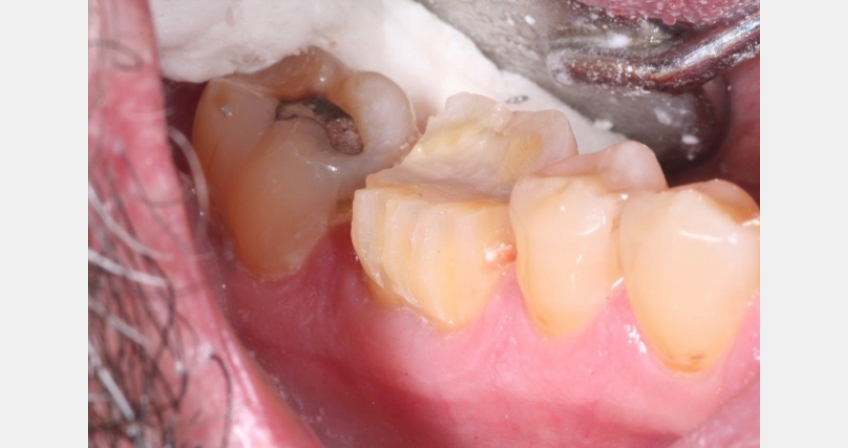
- I will then take the same bur on the facial and lingual and do depth cuts in two planes: in the incisal 1/3 and then to an approximate area of the margin along the gingival height. This bur is 1.0 mm in diameter, so adjust as needed for material choice. Be sure to account for the facial/lingual area where you need added thickness for the functional cuspal area.
- Place the bur back in the depth cuts and pull/push again to quickly remove the segments of tooth remaining between the depth cuts. Cutting these segments away at this stage is more efficient than milling the tooth back and forth. Once the enamel is reduced, you can easily smooth and refine the margins.
- Carry the bur carefully between the interproximal areas to break contact and follow the gingival contours and/or restorative material.
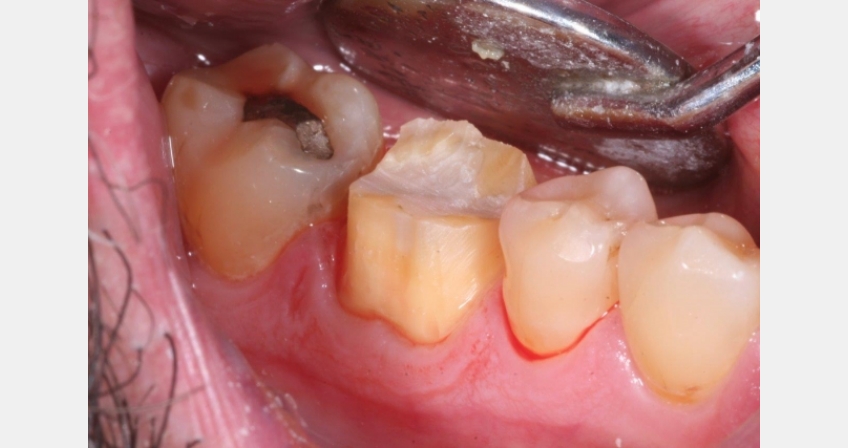
- Rough finish the margins with this bur and round off any immediate edges or ledges.
- Switch to a larger, finer diamond bur to refine and smooth margins and preparation overall.
- Done!
Most teeth I prepare day in and day out are posterior teeth, but here is a link to an excellent video in the Spear Education Course Library on anterior tooth preparation. I have also taken the restorative design workshop, a hands-on course that is an excellent review of preparation design. You also get to prep a lot of teeth on models!
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Jeff Lineberry
Date: December 17, 2021
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


