Where, Oh Where, Did That Tooth Wear Come From? Part 2
In Part 1 of this series, I discussed attrition, which is potentially the etiologic agent of tooth wear with the poorest long-term prognosis. In this article, I will discuss erosion, which in contrast to attrition can have an excellent long-term prognosis if managed well.
What is erosion?
Defined as the loss of tooth structure due to acids, either ingested or regurgitated, erosion can be present in locations where there is or is not occlusal contact. The wear is typically not sharp and flat as seen in attrition, but rather has a soft, satin and rounded appearance.1 (See Fig. 1.)
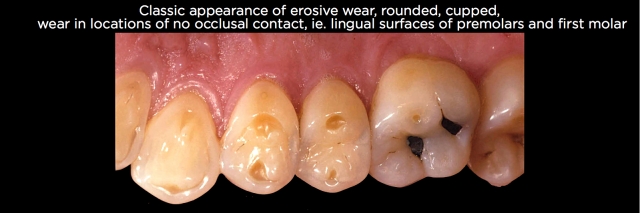
The mechanism by which erosive tooth wear occurs is through a demineralization of the tooth, similar to acid etching, followed by a loss of the demineralized layer through abrasion from the opposing tooth, tongue, cheeks, food or external objects such as a toothbrush.
The erosive effect
This process of erosive tooth wear explains some of the commonly seen, but confusing presentations of erosion, such as cupping on the cusps of posterior teeth. The acid demineralizes the entire occlusal surface, but the cusps are more vulnerable to abrasion following the demineralization than the fossa are. As the erosive wear occurs on the cusp tips it eventually penetrates to dentin, which wears at a faster rate then enamel. Once the dentin starts to cup under the enamel, the enamel now can collapse and the cup grows. These cupped lesions have been attributed in the past to occlusal issues, but it is easy to find examples where the opposing tooth is completely unworn, showing that erosion was responsible for the wear, not some strange occlusal behavior.
There are two primary categories for the acid which produces erosive wear: intrinsic (regurgitated) and extrinsic (ingested). Either source of acid can produce erosion, but in general they do have different appearances. Regurgitated acid tends to produce wear on the lingual and occlusal surfaces, while ingested acid tends to produce wear on the facial and occlusal surfaces.2, 3
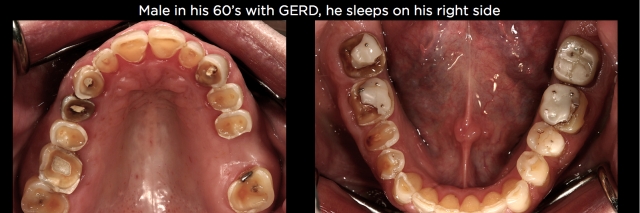
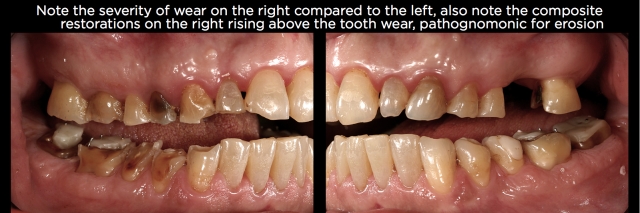
Along with the source of the acid, the individual’s head posture and gravity also play a role in the appearance of the erosion. For example, because gastric reflux often occurs during sleep, the position in which the person sleeps will impact where the acid ends up. If they sleep on their right side, the teeth on the right may show far more wear then the teeth on the left since the acid will pool on the left. (See Figs. 2 and 3.) In addition, when acid is ingested, most individuals’ heads are upright so gravity has the potential to produce greater erosion of the mandibular arch then the maxillary.
The easiestway to learn to see erosion is to look at images of the more common erosive conditions that tend to produce recognizable patterns, understanding that some erosive patterns are very difficult to identify because they relate to specific habits the patient may have, such as sucking on acidic candy or placing acidic products at specific locations in their mouth.
Six common forms of erosion
Here are the more common forms of erosion and images to show their appearance:
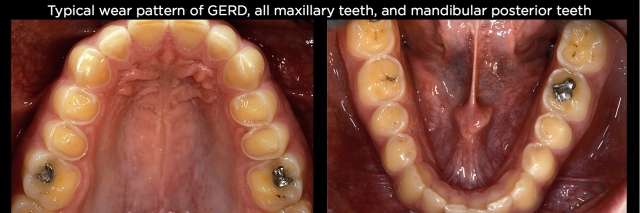
- Gastric Reflux (GERD) – This regurgitated acid typically produces wear on the lingual and occlusal of all maxillary teeth, usually with less wear on the molars then the premolars, as well as wear on the lingual of the maxillary anterior teeth and wear on the occlusal of mandibular posterior teeth. As stated earlier, it may be worse on one side than the other due to sleep positions.4, 5 (See Fig. 4.) The article at this link explains more about the dental diagnosis of GERD.
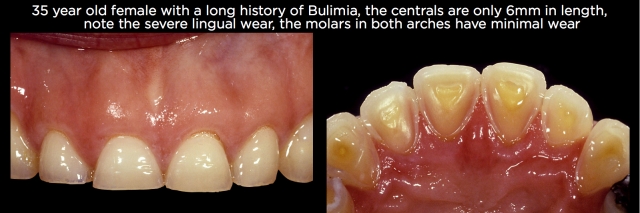
- Bulimia – This is also regurgitated acid but with a significantly different head posture then GERD. The head is typically tipped forward, and the regurgitation is physically induced at high velocity. This produces massive wear on the maxillary anterior teeth and often the lingual of the first premolars. Compared to GERD, there is much less wear on the maxillary or mandibular posterior teeth. In addition, GERD produces wear on the lingual of the maxillary anterior teeth, but may not result in them being reduced in length significantly. Bulimia often devastates the length and lingual thickness of the maxillary anteriors. (See Fig. 5.)
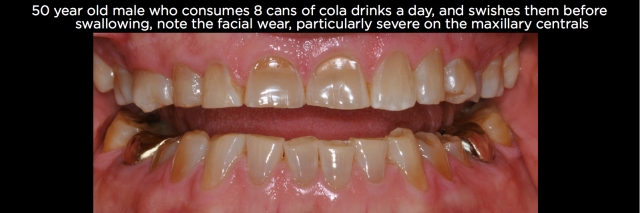
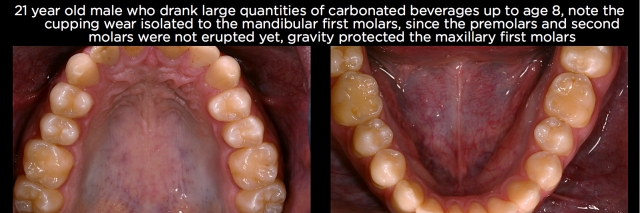
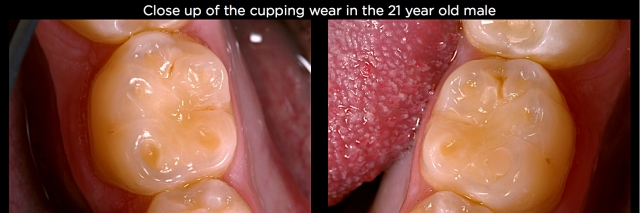
- Acidic beverages – These are ingested acids that produce variable patterns of wear dependent upon the individual’s habits after ingesting them. Carbonated beverages, energy drinks, Gatorade and many other beverages have an acid content capable of producing erosive wear. If the individual ingests the beverage and then swishes it around their mouth prior to swallowing, the wear often shows up on the facial surfaces of teeth, particularly the maxillary anteriors. (See Fig. 6.) If the individual ingests the beverage and then lets it sit in the floor of the mouth prior to swallowing, the mandibular posteriors will show the most wear. (See Figs. 7 and 8.) Check out this article for more on dietary acids.
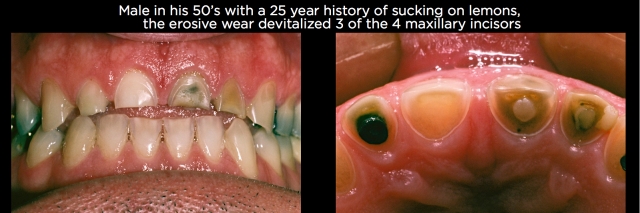
- Citrus fruits – Just as with acidic beverages, the pattern of wear is determined by how an individual ingests the fruit. If the person bites through the fruit and sucks the juice out of it, such as sucking on lemons, the anterior teeth will start to look like the blades of a screwdriver. (See Fig. 9.) If they only penetrate the fruit with the maxillary anterior teeth, they will be the most affected. Additionally, the facials of the adjacent premolars will show the typical signs of erosion – a satin appearing surface. If the individual mulls the fruit, which means they place it in the posterior portion of their mouth and chew it like a cow, the posterior occlusal surfaces will show the most wear.
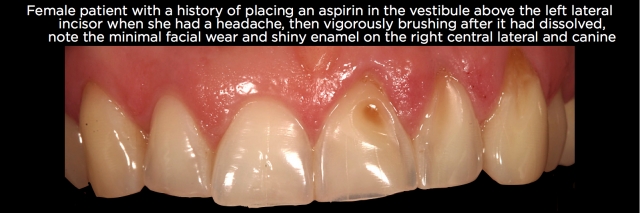
- Habits – Any product with a high acid content that is placed locally in the mouth can produce isolated patterns of erosive wear. Items such as an aspirin tablet, acidic fizzy candies or certain illegal drugs would be common examples. (See Figs. 10 and 11.)
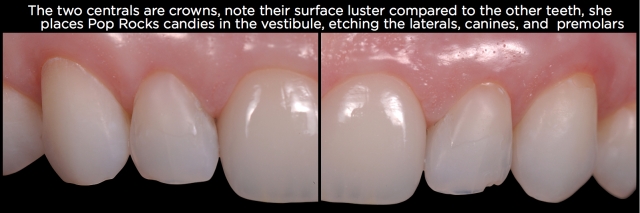
- Other – There are other etiologies of erosive wear of which a clinician needs to be aware that can mimic some of the conditions above. Two significant examples are a lack of normal salivary buffering capacity and asthmatic inhalers. Both tend to mimic GERD. Acidic medications can also mimic other patterns of wear.6
There are countless other examples of erosive tooth wear, but these example should provide a clinician with visuals to aid in identifying erosion as the etiologic cause of the wear in many or their patients. Of particular significance is recognizing that many cases of GERD are undiagnosed, and the erosive wear may be the first sign of its presence. This is critical because GERD can lead to Barrett’s esophagitis, which can be a precursor to esophageal cancer.
The good news about erosive tooth wear, assuming the patient doesn’t have attrition as well, is that once the teeth are restored with margins placed onto non-eroded tooth structure, the long-term prognosis for the patient is excellent.
References
1. Int Dent J. 2005;55(4 Suppl 1):277-84.
The role of erosion in tooth wear: aetiology, prevention and management.
Prosthodontics, King’s College, London, UK
2. N Z Dent J. 2003 Jun;99(2):33-41.
Dental erosion: part 1. Aetiology and prevalence of dental erosion.
Biomaterials Research Unit, University of Sydney, National Innovation Centre, Eveleigh, NSW, Australia.
3. Monogr Oral Sci. 2006;20:119-39.
Intrinsic causes of erosion.
Department of Prosthodontics, GKT Dental Institute, London, UK.
4. J Pediatr. 2002 Apr;140(4):474-8.
Gastroesophageal reflux disease and dental erosion in children.
Division of Pediatric Gastroenterology, Oklahoma University College of Medicine, Tulsa 74129, USA.
5. Gen Dent. 2003 May-Jun;51(3):250-4.
Gastroesophageal reflux disease: a dental concern.
Department of Restorative Dentistry, University of Tennessee College of Dentistry, Memphis, USA.
6. J Dent. 2004 Aug;32(6):489-94.
Dental erosion, gastro-oesophageal reflux disease and saliva: how are they related?
Department of Conservative Dentistry, Floor 25 Guy’s Tower, St Thomas’ Street, London Bridge, London SE1 9RT, United Kingdom.
VIRTUAL SEMINARS
Stay Sharp. Stay Current. Stay Ahead.
Join live, focused training designed to help you implement immediately and strengthen your expertise.

By: Frank Spear
Date: September 14, 2015
Featured Digest articles
Insights and advice from Spear Faculty and industry experts