The Reference Denture Technique: An Interdisciplinary Case Study
By Effie Habsha on July 15, 2025 |Many edentulous patients wear their prostheses for longer than they should, often because they’re determined to avoid change. They fear a new denture might be less comfortable, less aesthetically pleasing, or simply different than the prosthesis to which they’ve grown accustomed.
The reference denture technique, sometimes called the denture duplication workflow, provides technicians with a digital record of a patient’s existing information and allows us to rehabilitate the dentures more confidently, predictably, and precisely than would otherwise be possible. This technique’s technically and clinically integrated workflow can reduce the number of required postoperative adjustments and visits, and when executed correctly, it allows for a high standard of precision care and craft when treating edentulous patients who are generally satisfied with their existing denture but need a replacement at the end of its regular lifespan.
Duplication, Modification, Fabrication
The reference denture process begins with a 360-degree scan of the patient’s existing denture(s). The detailed digital records direct the creation of a 3D-printed duplication, which is used to produce closed-mouth functional final impressions and capture a new centric relation record. With this workflow, the clinician can make any necessary adjustments to tissue-bearing surfaces or any areas of irritation or overextension during the clinical process.
After these procedures, the information is digitized using an intraoral scanner, and both the clinician and the attending technician possess the data necessary to create a functional try-in prosthesis for evaluating fit, form, function, aesthetic and phonetic performance. At this point, small but meaningful modifications can be communicated to the dental technician and precisely modified in the digital denture software before the final definitive restoration is fabricated.
This article showcases the fabrication of a complete maxillary denture and complete mandibular implant-supported overdenture using the reference denture technique.
Case Presentation
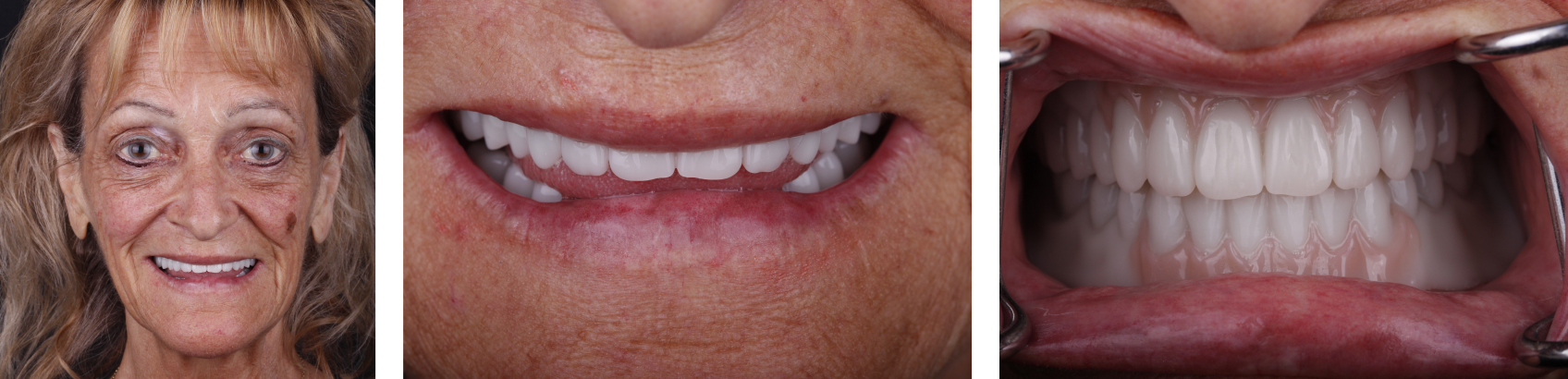
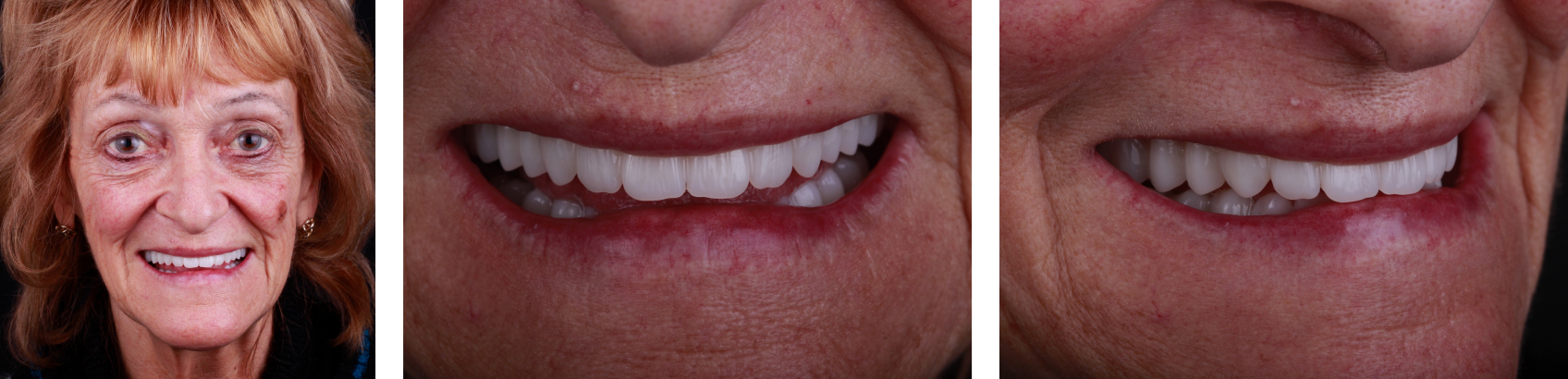
This patient was reluctant to commit to a new set of dentures because she was generally pleased with the fit and aesthetic appearance of her original ones, but she also realized that the occlusal surfaces had worn so much (Figures 1 and 2) that the dentures no longer functioned properly.
Her maxillary denture had been delivered immediately after the maxillary dentition had been extracted, while her mandibular implant-supported overdenture was a relined, retrofitted version of the original immediate complete mandibular prosthesis.
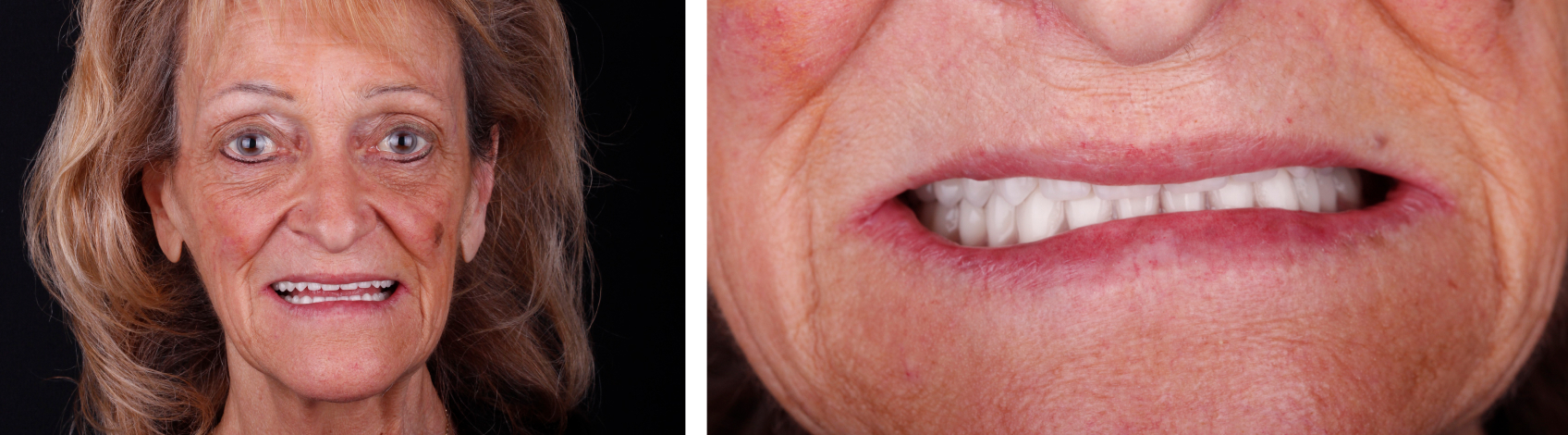
The patient asked for her new dentures to be as similar as possible to her current set, to which she had become anatomically and psychologically accustomed.
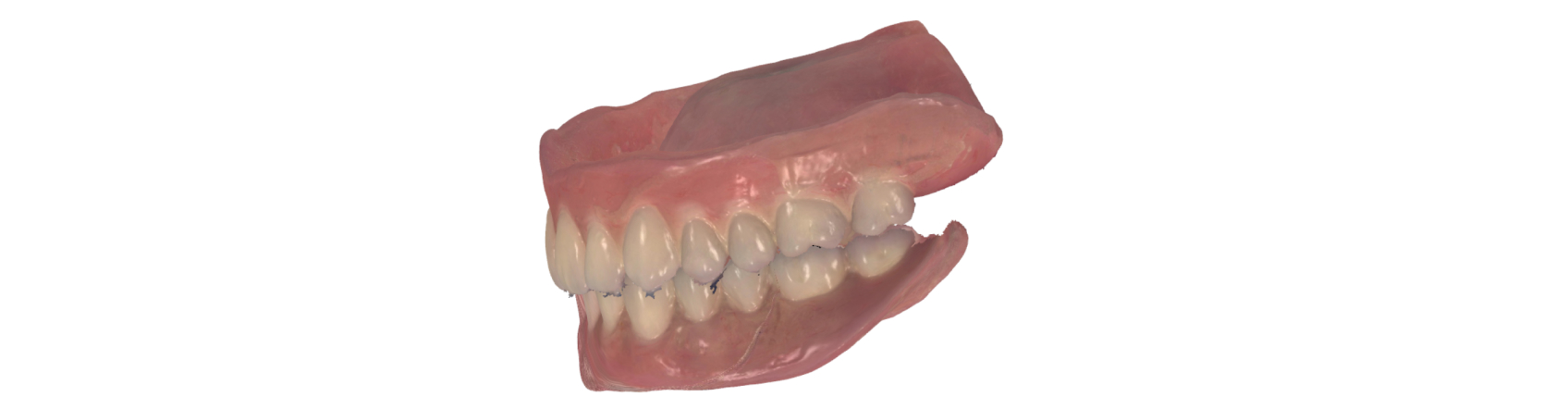
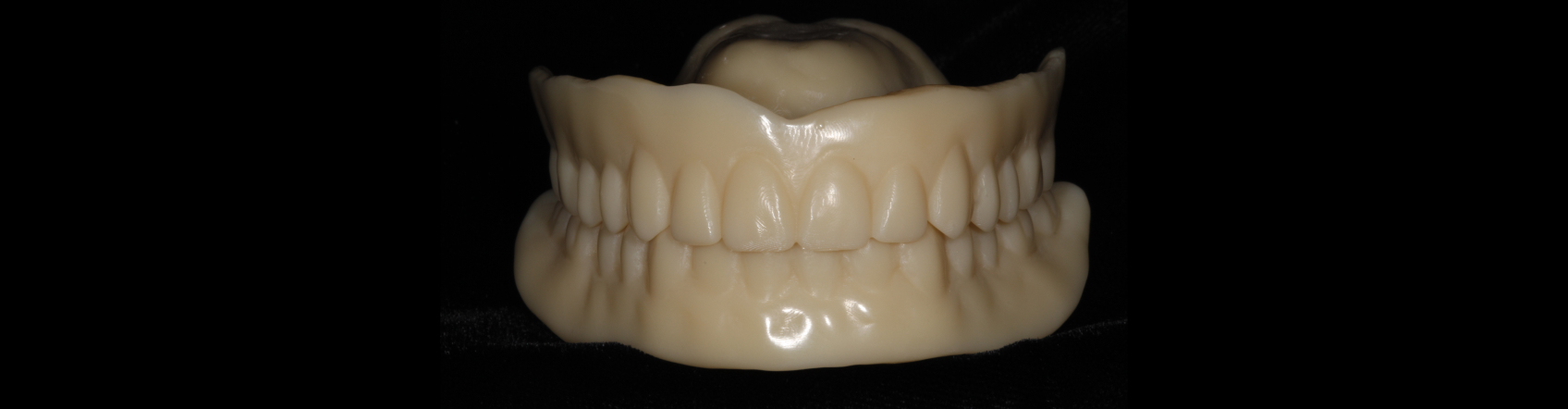
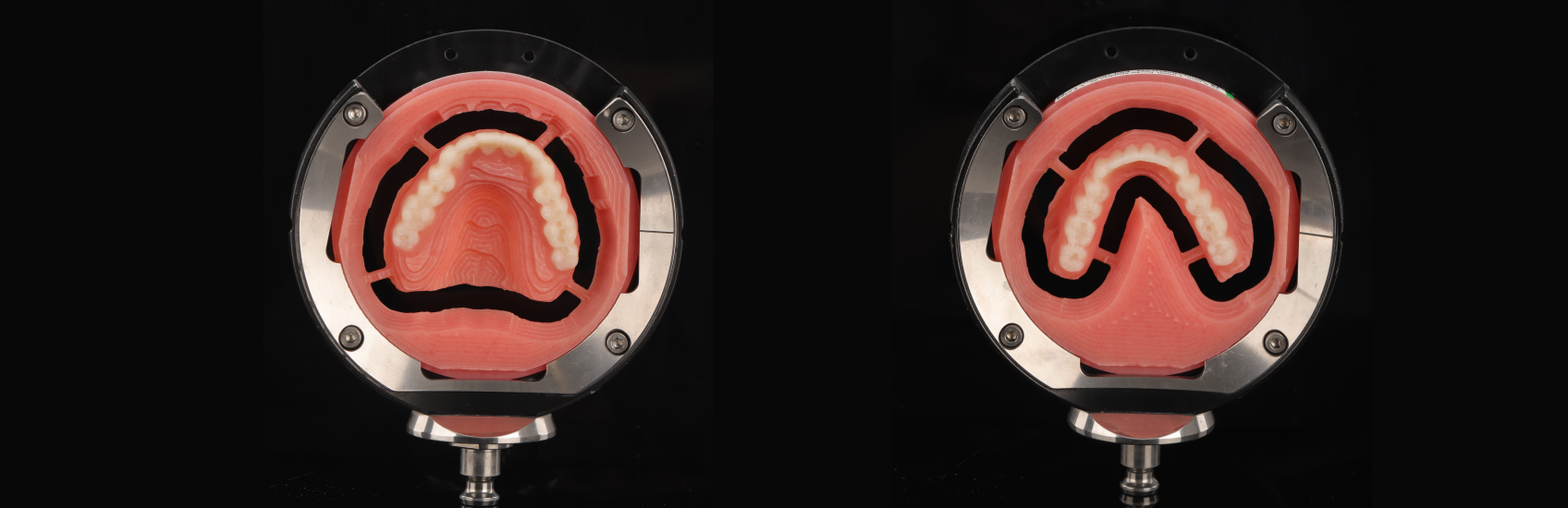
In Toronto, my team used an intraoral scanner (Trios, 3Shape) to capture the reference scan of the existing dentures (Figure 3). The data was sent to The Denture Center’s lab in Windsor, Ontario, where denturist Erick Kukucka and his team 3D-printed a duplication (Figure 4) based on the digital records. This duplication was used as a custom tray and centric relation recording device during the next clinical appointment.
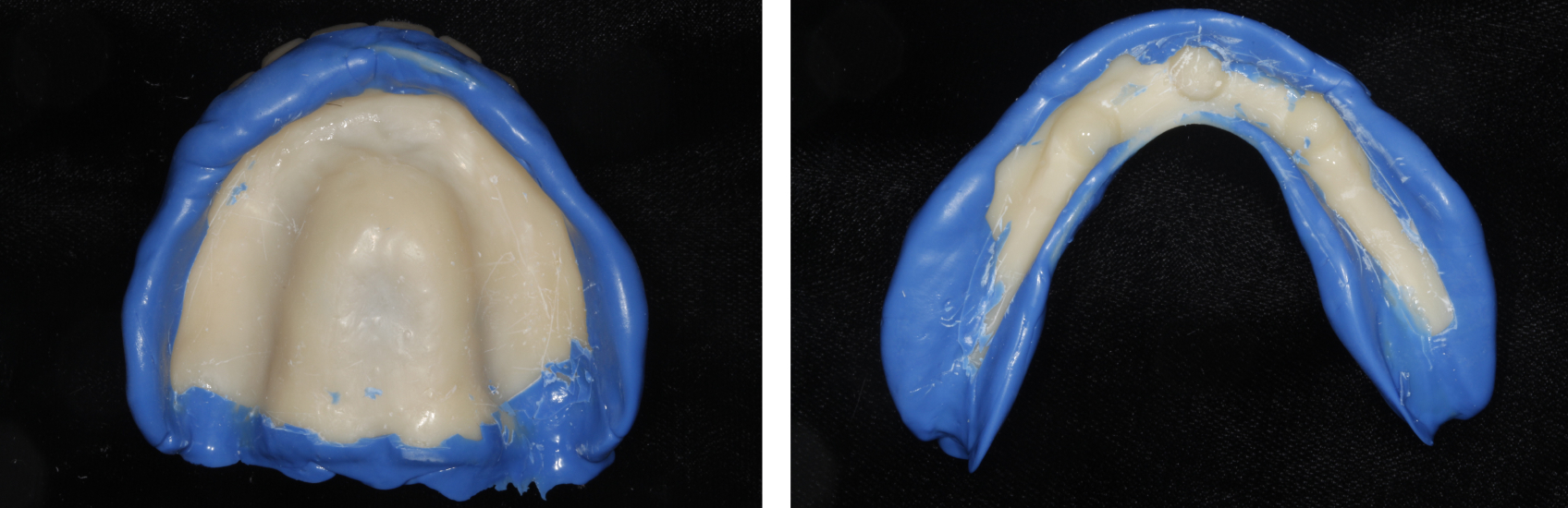
At the patient’s next appointment, closed-mouth functional impressions of both the maxillary and mandibular duplicated dentures were conducted to capture muscular mastication and facial expression. With this technique, impression material is distributed under the patient’s functional forces to capture the oral cavity in a functional state, usually using a heavy-body or monophase material (Virtual XD Heavy Body, Ivoclar Vivadent) for the borders (Figures 5 and 6) and light-body material (Virtual Light Body, Ivoclar Vivadent) for the intaglio/tissue-bearing surfaces (Figures 7 and 8). Then a centric relation record was registered (Figure 9).

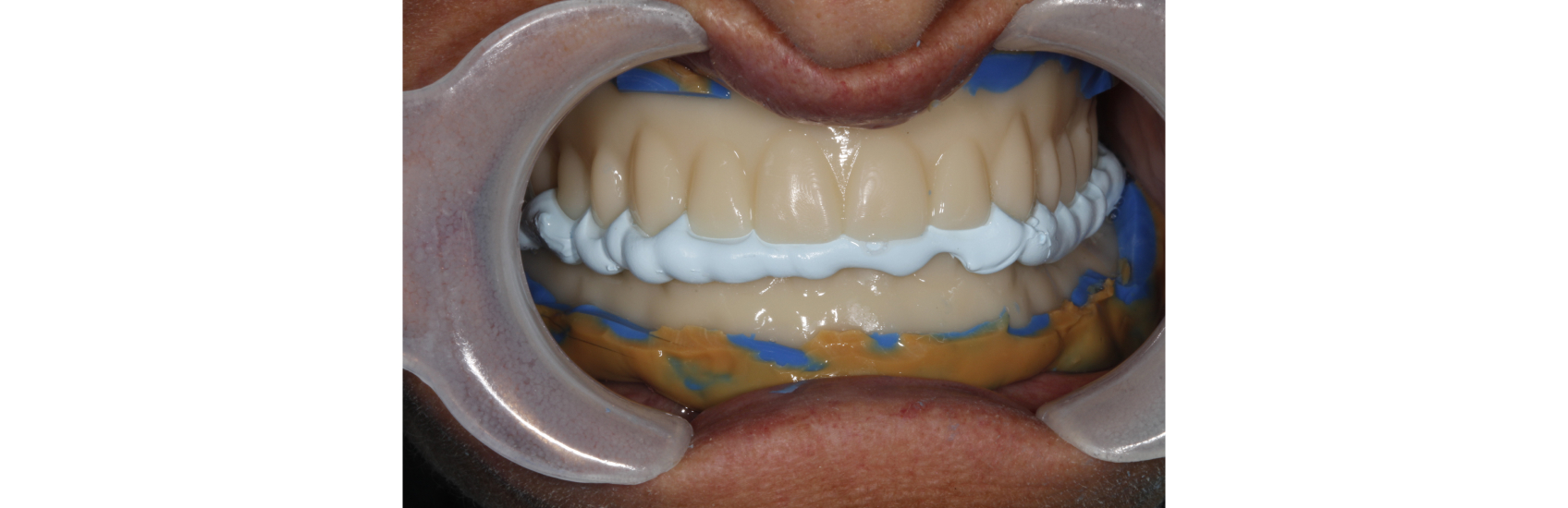
The patient’s records were then scanned (Figure 10) using the reference denture scan strategy to create global accuracy of the impression scans and centric relation record. These files were transferred back to The Denture Center lab through the 3Shape Communicate platform.
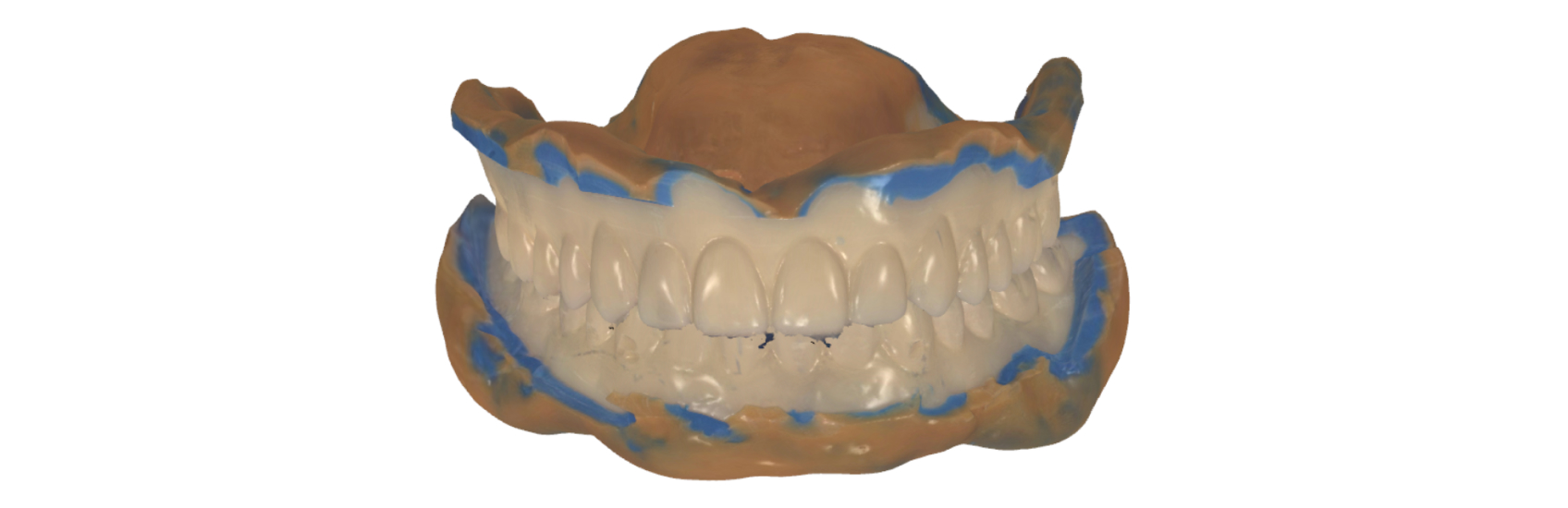
The Denture Center lab team used 3Shape Dental Systems software to design a new smile based on the clinical parameters (Figures 11 and 12), using the scanned reference dentures as a guide to position the anatomical tooth arches (Phonares S71–L50–NU3 NL3) and produce a functional try-in prosthesis. This transitional product allowed me to evaluate the fit, form, function, aesthetic and phonetic performance of a denture in progress.
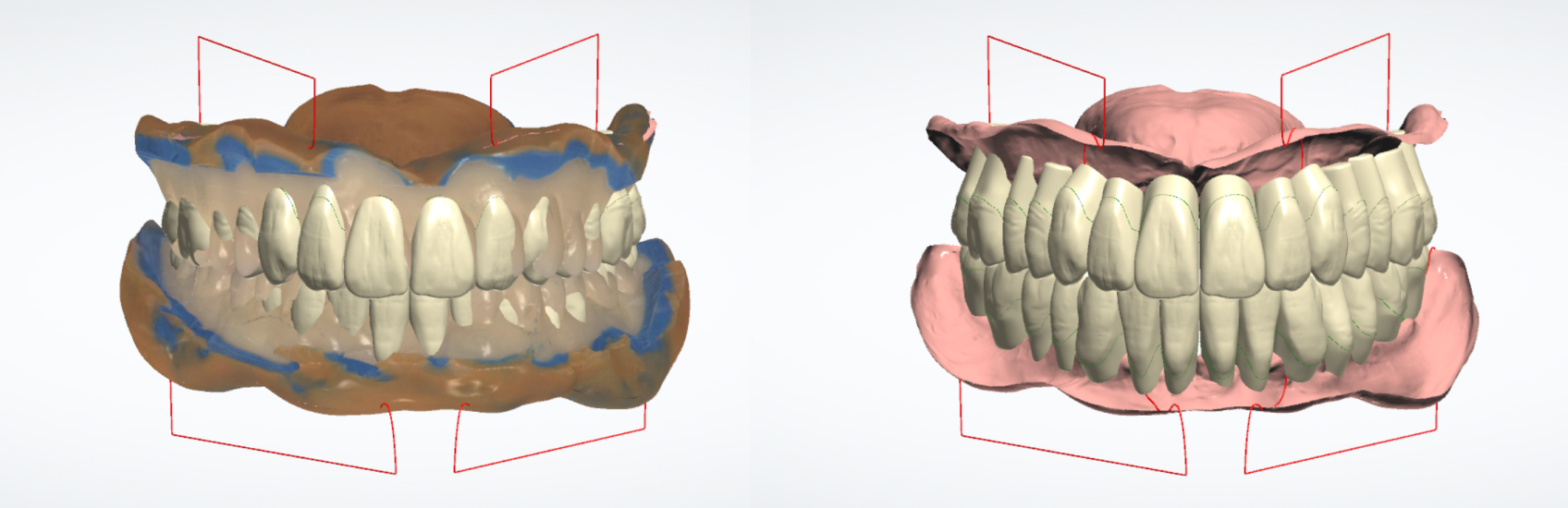
For a comparative demonstration, the Denture Center team produced and presented the patient with two slightly different try-in prostheses. The first option (Figure 13) included some gingival composite (SR, Nexco) added to the gingiva and interdental papillae regions of the anterior teeth in both arches to highlight the high smile line for the patient’s benefit. The second option (Figure 14), a monoblock try-in, omitted the gingival composite and was a solid shade.
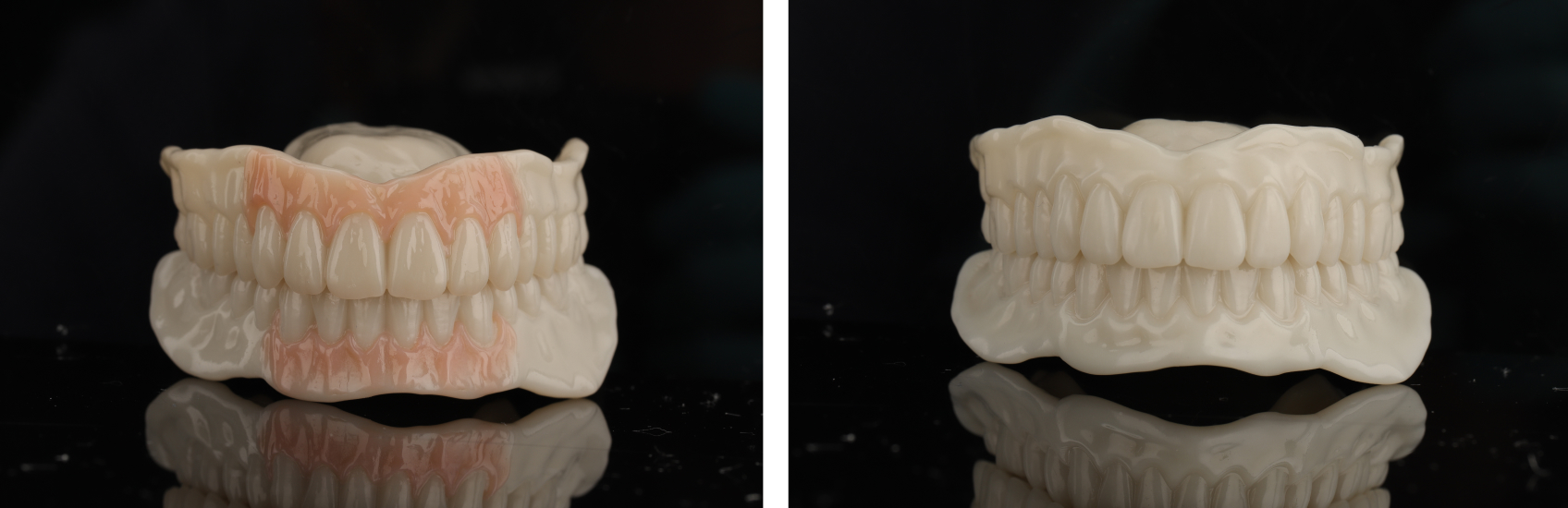
The patient was already enthusiastic about the result after the initial proposal, but I requested some minor prosthetic changes to enhance the prosthetic's aesthetic appearance (Figure 15):
- The maxillary central incisors of Teeth 11 and 21 were made one millimeter longer.
- The buccal cusps of Teeth 14 and 24 were modified (Figures 16 and 17).
These changes were conducted in the 3Shape Denture Design software with precision and simplicity.
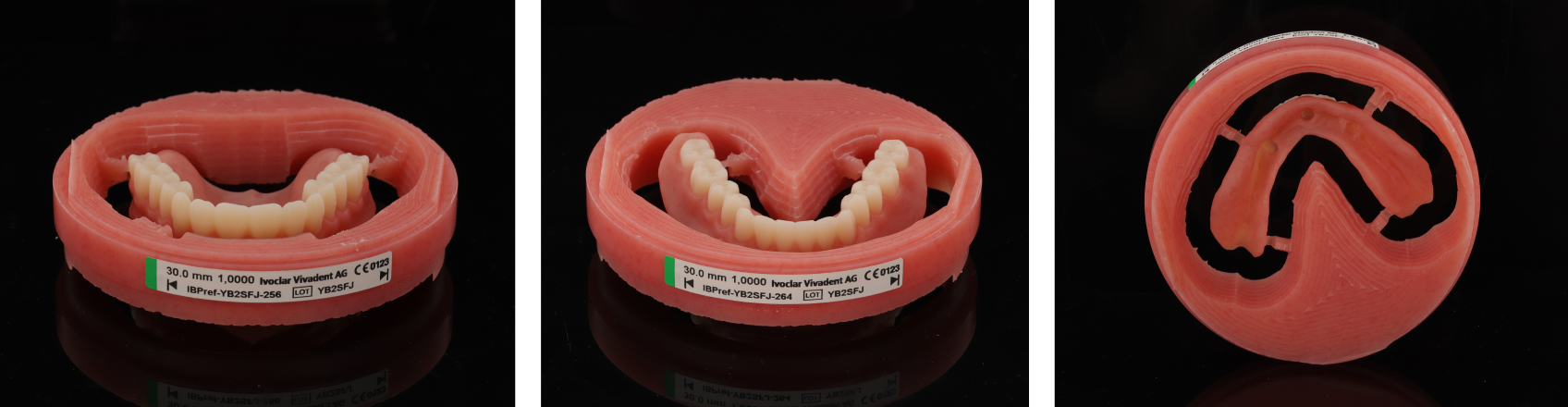
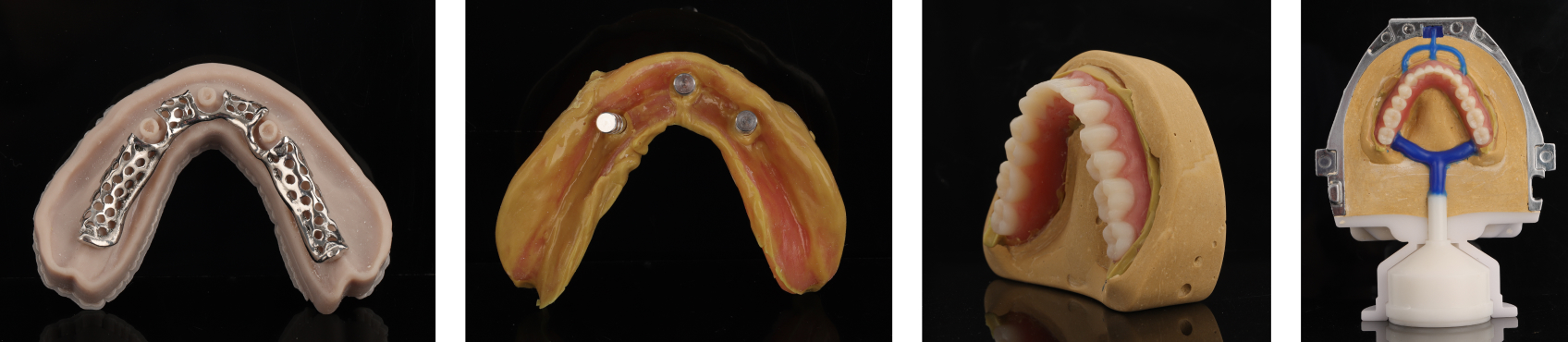
Once the final design was approved, the Denture Center lab milled the pink denture base from Ivoclar Vivadent’s Ivotion Base (Figure 18) and the teeth from the company’s Ivotion Dent Multi, a monolithic, polychromatic double cross-linked polymethyl methacrylate material (Figure 19).

Kukucka’s team used the Oversize milling process, which improves efficiencies and the accuracy, predictability, and overall strength of the restorations, largely by removing the need for manual removal of excess bonding material. In accordance with this process, both the tooth arch and denture base were milled to approximately 80% completion, while the base sockets and tooth necks were milled to precise standards.
|
Don’t Miss This Retreat! Spear Resident Faculty member and Dr. Effie Habsha will lead the Women in Dentistry retreat, featuring two days of dental education and health and wellness activities curated specifically for female dental professionals. 11 CE credits. To learn more about the event, which will be Sept. 19–20 on the Spear Campus in Scottsdale, click the button below! |
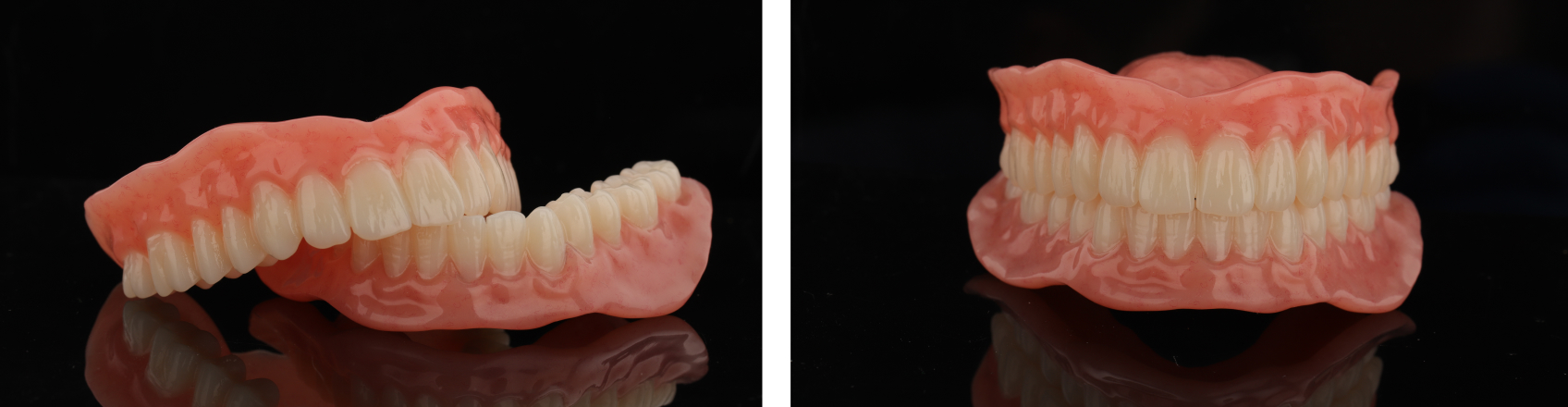
Then, the arches were bonded together (Figures 20 and 21) using Ivotion Bond, an auto-polymerizing PMMA-based material that creates a seamless chemical bond between tooth structure and the denture base.
Finally, the denture was returned to the milling machine for finishing.
Figures 22 and 23 represent the ultimate product, which satisfied the patient’s desire for optimal aesthetic results. Note that the final definitive restoration in this case involved an intraoral direct chairside conversion of the locator housings (Figure 24). The milled prosthetics are finalized with a high polish (Figures 25 and 26).
This case study demonstrates two discrete manufacturing methods — the first as previously described and the second using a metal mesh framework. The team used digital denture technology to fabricate a metal framework surrounding the three dental implants (Figure 27) and captured a closed-mouth final impression in the mandible (Figure 28) to pour a master cast. Next, the cast was embedded with the metal framework and injected with SR IvoBase molding material, which “wrapped” around the metal, increasing the strength and rigidity of the mandibular prosthesis (Figure 29). This process is very similar to a rebase modality in conventional dentures (Figure 30).
At the patient’s next appointment, the dentures required only minimal adjustments. She was thrilled with the results in terms of fit, stability, aesthetic, and phonetic function (Figures 31–33), as well as the general interdisciplinary collaborative care experience.
Conclusion
Digital dentures have revolutionized the way we conceptualize and fabricate removable prostheses. Never before have oral health care professionals in different facilities, fields, and locations been able to communicate such granular, sophisticated data as precisely and efficiently as now. The current digital denture workflows allow clinicians to capture and digitize a patient’s oral cavity with tremendous detail and to design and produce removable prostheses with extreme accuracy and predictability, minimizing the amount of postinsertion adjustments.
While the reference denture treatment framework is an effective and versatile treatment, it is yet to be recognized as a global standard for removable prosthodontics. Many clinicians are also reluctant to incorporate a digital denture workflow because of their lack of understanding and practice executing the technique. In our experience, clinicians and lab technicians often shy away from digital dentures and other emergent technologies because of a fundamental fear of the unknown: They aren’t familiar with the technology, they avoid change as a rule, or they simply don’t understand how to best implement it in their professional environments.
We expect the overwhelming evidence for the efficacy of digital denture workflows will influence these attitudes to change in time. Ultimately, the goal of removable prosthodontic rehabilitation is to improve a patient’s functional oral situation physiologically and neuromuscularly. If we do this, we improve that patient’s quality of life.
We believe, in many cases, the best means to this end is teamwork — and many of the very best possibilities for the precise connectivity and information sharing that drives effective teamwork are right in front of us in our clinical settings, workstations, and on our computer screens.
Author’s note: Thank you to Erick Kukucka, DD, and Lily Tran, my collaborators and co-authors on this case.
References
- Bidra A, Taylor TD, and Agar JR. Computer-aided technology for fabricating complete dentures: Systematic review of historical background, current status, and future perspectives. J Prosthet Dent 2013; 109:361–366.
- Anadioti E, Musharbash L, Blatz MB, Papavasiliou G, and Kamposiora P. 3D printed complete removable dental prostheses: A narrative review. BMC Oral Health 2020; 20:343.
- Janeva NM, Kovacevska G, Elencevski S, Panchevska S, Mijoska A, and Lazarevska B. Advantages of CAD/CAM versus conventional complete dentures — a review. Maced J Med Sci. 2018 Aug 20; 6(8):1498–1502.