Restoring Discolored Endodontically Treated Teeth: Case 1
By Frank Spear on January 26, 2016 | 10 commentsThis is the first in a series of examples of the different presentations that can occur surrounding the restoration of discolored endodontically treated teeth. This series will include examples I used in a previous Spear TALK (our online discussion forum) post, but some additional cases as well.
Case 1: A discolored endodontically treated lateral incisor
When considering how to treat these cases, the first thing I look for is the presence of a post or an indirect restoration. This would mean that most likely the tooth has had some tooth preparation done. In this lateral incisor there is not a post or any indirect restoration, only the composite to seal the access (Figure 1).

In addition the radiograph shows a successful result from the endodontics that was performed years earlier. It also does show that the access itself is quite large, meaning that any tooth preparation could end up with extremely thin walls (Figure 2).

Given these conditions the decision was made to utilize internal bleaching and no restorations to correct the discoloration. The key to the safety of internal bleaching is the placement of a seal slightly above the periodontal attachment to prevent the bleach from penetrating down the canal or into the periodontal attachment. If this precaution is not taken the literature reports root resorption rates varying from 1 to 13% (Figure 3).

The typical products used for internal bleaching are sodium perborate, carbamide peroxide, and up to 35% hydrogen peroxide. The recommendations today are to not heat the bleach as it creates additional risks for resorption. Instead I generally use a walking bleach for three to four weeks, although it may require repeating from one to three times to reach maximum effect. Avoiding heat and strong bleaching agents may be especially important in teeth with thin remaining walls.
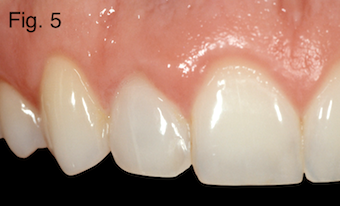
In this patient a walking bleach of sodium perborate was used for four weeks to achieve the result seen here (Figures 4 and 5). The bleach was sealed in the chamber with IRM during the four-week period.

Risk of reoccurrence of the discoloration varies dramatically in the literature, but can be as high as 50 percent by five to 10 years in some studies, meaning that the need to redo the bleaching is reasonably high. Nevertheless, in a tooth such as this one with no restorations other then the access cavity, and a very large access with thin walls, I believe re-bleaching over time represents a better choice then prepping and restoration.
Comments
February 14th, 2014
February 15th, 2014
February 18th, 2014
March 13th, 2014
April 4th, 2014
May 26th, 2014
June 18th, 2014
February 20th, 2015
April 11th, 2016
April 11th, 2016