Caries Detection, Part I: What Do You See?
By Dave St. Ledger on May 21, 2018 | 4 comments
The science and practice of dentistry has evolved mightily over the past 20-plus years to astounding levels of understanding and insight. Innovation and technology has exploded and is not going away ... and should not.
Patient evaluation has become more medically based. The need to discern and correlate a patient's medical and dental conditions are paramount to their overall health. But the information we need to sift through is staggering and can overwhelm even the most seasoned of clinicians. It has the power to stall treatment. If one cannot compartmentalize the fact finding, an approach to tie them together may become daunting.
Spear created a curriculum of learning to help any dentist with a methodical approach in patient education as well as their diagnosis and treatment. For those of you not yet familiar with their workshops, one in particular can have an immediate impact on your practice: Facially Generated Treatment Planning. It gives you the parameters to set up and think about all of the aspects of your patient's health looking at the esthetics, function, structure and biology (EFSB) of the patient. It is not to suggest we are looking at every case as esthetics are the most important. It is only a starting point. We all know that the foundation of great outcomes in oral health is with sound hygiene, a patient's biology.
(Click this link to learn more about comprehensive dental care.)
It would be wonderful if all dental treatments were rendered under comprehensive treatment planning. But the fact of the matter is it is not. The majority of dentistry is still tooth to tooth. And this is fine, especially for the purpose of this article: caries detection. At the end of every day, we are all tooth to tooth dentists. Why? Because each tooth still requires its own level of attention when determining bacterial infiltration or bacterial effects on the architecture that houses said tooth.
Let’s turn the EFSB model upside down for a moment and focus on one small aspect of biology: the never ending problem of interproximal caries. The bane of a tooth’s existence! They seem to occur in just about any dentition:
- People who brush poorly likely do not floss
- People who brush well likely do not floss enough
- People who brush well and floss regularly but not well enough
- People who brush and floss as well as can be expected still are subject to caries
Even that last group still must deal with the other variables of tooth decay:
- Tooth hardness; genetics and fluoride exposure
- Diet; sugar and acid levels
- Salivary flow; alkaline or acidic; serous or mucus-like; abundant or dry
According to the Center for Disease Control:
- Percent of children ages 2-17 with a dental visit in the past year: 83.0 percent (2013)
- Percent of adults ages 18-64 with a dental visit in the past year: 61.7 percent (2013)
- Percent of adults ages 65 and over with a dental visit in the past year: 60.6 percent (2012)
- Percent of children ages 5-19 years with untreated dental caries: 17.5 percent (2011-2012)
- Percent of adults ages 20-44 years with untreated dental caries: 27.4 percent (2011-2012)
What may these statistics suggest when put together?
- The untreated dental caries is a result of those who have not had a dental visit in the last year. And if it is a year, what percentage of them is more than two or three years, or longer?
- The untreated dental caries are a result of patients not having legitimate access to care.
- The untreated dental caries are the result of being informed of the caries and leaving them untreated due to:
- Fear
- Finances
- Lack of patient education
- The untreated dental caries are a result of misdiagnosis, or better stated, from under-diagnosis.
Dental caries are still about the most chronic disease prevalent among both children and adults. The National Institute of Health (NIH) stated this in a study from 1999-2004. As clinicians, as dentists, we still do not have a uniform agreement of which caries requires intervention … meaning treatment, predominantly for interproximal caries. The Class II lesion seems to be still up for discussion relative to intervention.
There are those who treat:
- At the first radiographic sign of the lesion before it gets to the dental-enamel junction (DEJ)
- Once the lesion penetrates the DEJ on a radiographic image
- Only if a lesion is seen on a black and white image; if something appears identifiable on a PA image and not a black and white image, it often is observed until the next set of images
- At the first radiographic sign, not with a Class II restoration, but with a fluoride dentrifice
Patients go to their dentist and the one thing they expect is an evaluation of their oral health relative to bacteria: gum disease and tooth decay. All of the other aspects of dentistry – esthetics, function, TMD, oral cancer screening, sleep disorder screening , diet, etc. – take a back seat to bacteria. They deserve more of a consensus on a type of lesion that can become troublesome quickly. The fourth scenario listed above is something that is actually taught in at least one dental school in the United States. It is recommended that the Class II lesion just short of the DEJ can be arrested with the use of Prevident 5000 plus. I felt compelled to report this.
The problem is in the eye test. All radiographic images are not created equal. It is very common to recognize a Class II lesion, open up the tooth and find more area of decay than you envisioned. Waiting to see if you can arrest these caries may be all for not, as they are likely more advanced than meets the eye. I would like to share with you examples of patients with lesions that were being “waited on,” “watched” or “observed.” All of them came into the office as new patients within the last few years. Without you having to toil and make a decision on what to treat, relax and look at these radiographs and their respective photograph, in an exercise of the reality of Class II lesions.
(Click this link for a course on obtaining ideal images using oral radiography.)
Note: All of the photos within show the teeth during some portion of tooth preparation. The final preparations are not the purpose of this article.
Patient 1: #12





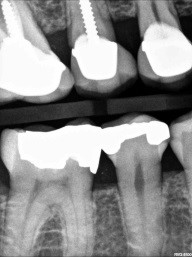
This patient presented in 2015 and brought her 2013 black and white image with her (digital jpeg) – the first images above. The second set of black and white images are from 2015. Notice the change in the interproximal caries. Even with a significant change (hypothetical) in a patient's habit and fluoride delivery, how do these types of caries arrest predictably?

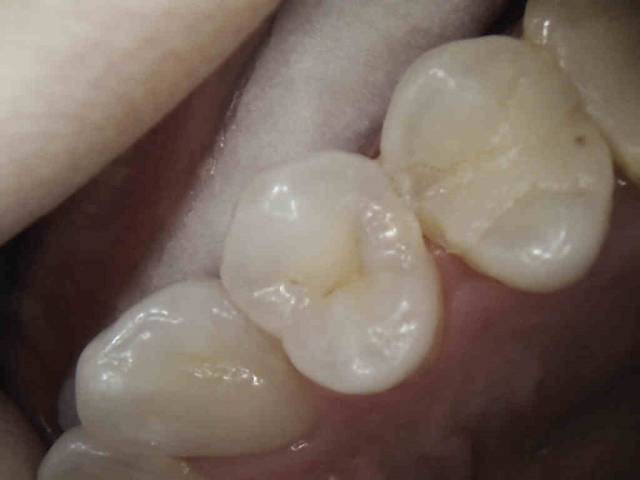
Again, the same patient, a photo of #29. Observe the black and white image again, then come back. Notice the color change at the distal ridge and the fissure (not a crack yet as it was smooth on examination). The tooth has not yet been treated.
Patient 2: #28

A similar situation with a different patient, this time with caries to the DEJ. Caries were verified under the mesial of #29 as well and were more severe.
Patient 3: #12


This is a tough one for clinicians to believe in, but the distal of #12 does, in fact, have caries. It appears less obvious and short of the DEJ. The photo mid-prep shows otherwise. Premolars, especially, are frail to begin with. Keeping any and all restorations conservative is the name of the game.
Patient 4: #12 and #13


On the black and white image, the patient has caries on #12, #13, #18, #19 and #20. We will focus on #12 and #13, especially, the mesial of #13. The black and white image is less suggestive there than on #12. The photo tells a very different story. #13 is more advanced.
Patient 5: #18

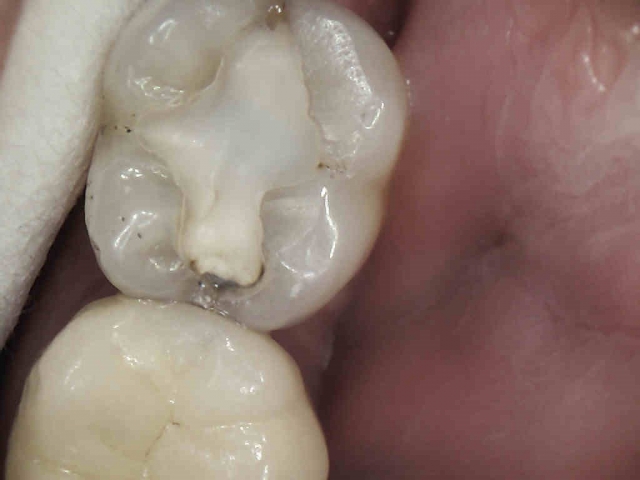
This patient was referred from a periodontist who was going to extract #19 with socket preservation. The black and white image is deceiving, as they can be sometimes. Here, the mesial does not show a definitive lesion. It is here that the clinical examination is key. Do you examine and chase cracks? If a marginal ridge has a crack that is palpable to your explorer, and it is discolored, it is leaking. The photo image shows this well. The image that follows shows quite a different story than the black and white image. Notice the crack mid-prep is still quite prevalent.

I hope this article has made you at least a little more curious to what lies beneath those marginal ridges we examine each and every day. In Part II of this series, we will examine the advancements in technology and dentifrices that exist on the market, enabling us a better chance to diagnose, restore or prevent further tooth destruction.
(Click this link for more articles by Dr. David St. Ledger.)
David St. Ledger, DDS, Visiting Faculty, Spear Moderator, Contributing Author
Comments
March 21st, 2016
May 24th, 2018
January 10th, 2019
January 10th, 2019